All published articles of this journal are available on ScienceDirect.
Knee Arthritis Without Other Joint Symptoms in the Elderly With Seronegative Elderly Onset Rheumatoid Arthritis
Abstract
Elderly onset Rheumatoid arthritis (EORA) has important clinical distinctions when compared with younger onset RA (YORA). In knee arthritis of elderly patients, infection, crystal-induced arthritis or EORA should be suspected if elevation of CRP in the preoperative examination and turbid joint effusion in their knee joint are found. Furthermore, if joint swelling and effusion remain after performing total knee arthroplasty (TKA), the infection after TKA, implant debris-related arthritis and EORA should be considered. However, it is difficult to diagnose patients as EORA if Rheumatoid factor (RF) and anti-cyclic citrullinated peptide antibody (ACPA) are negative. The differential diagnosis is very important.
INTRODUCTION
Rheumatoid arthritis (RA) is characterized by inflammation of the synovium, occurring most frequently in the joints. This inflammatory process frequently leads to loss of cartilage and bone erosion. The level of joint destruction is correlated with the severity of inflammation [1, 2]. Lipsky reported that the prevalence of RA is approximately 0.8% in the general population [3]. In the USA, prevalence of RA is reported to be in between 0.55 and 1% with a prevalence of ~2% among persons above the age of 60 [4]. RA onset is variable. A steadily increasing prevalence rate of rheumatoid arthritis with age has been reported [3]. Cases with the disease beginning above the age of 60 are defined as having elderly onset. Elderly onset RA (EORA) has important clinical distinctions when compared with younger onset RA (YORA) [5, 6]. Several studies have reported a lower percentage of Rheumatoid factor positivity in EORA [7, 8]. When the patients have severe knee pain and gait disturbance, they are advised to undergo knee arthroplasty. In RA patients, total knee arthroplasty (TKA) is performed for knee arthritis of RA. In seronegative elderly onset RA patients without other joint symptoms, it is difficult to determine whether knee pain and deformities are due to RA or osteoarthritis (OA). In patients referred with severe OA, infection, crystal-induced arthritis or EORA are suggested if elevation of CRP in the preoperative examination and turbid joint effusion are found. To perform TKA, EORA should be discriminated from infection. Seronegative EORA without other joint symptoms is difficult to diagnose clearly, and if joint swelling and effusion remain after performing TKA, the infection after TKA, implant debris-related arthritis and elderly onset RA should be considered. Patients are diagnosed as seronegative EORA without other joint symptoms if rheumatoid factor and ACPA are negative; however, these patients also have the possibility of knee joint infection. The differential diagnosis of seronegative elderly onset rheumatoid arthritis is very important.
CASE 1
A 78-year-old man exhibited pain in his right knee joint for one year without any obvious cause. He was diagnosed with osteoarthritis at a nearby hospital and received intraarticular hyaluronic acid injections, but no improvement was observed. He recently demonstrated severe pain and gait disturbance, and was therefore referred to our department with suppurative arthritis.
On physical examination, mild swelling and local heat were observed in the right knee joint. Redness was not present. His range of motion was -15 to 140°. X-ray images confirmed severe arthropathic changes (Fig. 1). Laboratory tests revealed that WBC was 9700 and CRP was 1.35 mg/dl. The aspirated synovial fluid was yellowish and slightly turbid. Bacterial culture and crystal were negative. We considered RA or infection to be possible. Rheumatoid factor (RF), anti-cyclic citrullinated peptide antibody (ACPA) and anti-nuclear antibodies were negative. For arthroscopic findings, synovial hypercellularity was noted.

Histological examination revealed signs of synovitis, including proliferation of synovial tissue, infiltration of plasmacytes and neutrophils, and the presence of granulation tissue. These observations were highly suggestive of rheumatoid arthritis. Rt TKA was then performed. However, pain and swelling of the left knee and right shoulder appeared. methotrexate (MTX) was increased to 8 mg/day. The symptoms persisted. Golimumab was initiated and his symptoms subsided immediately.
CASE 2
A 74-year-old female developed pain in her right knee joint and gait disturbance without any obvious cause a year prior to referral. These symptoms increased gradually. Therefore, she was referred to our department for total knee arthroplasty.
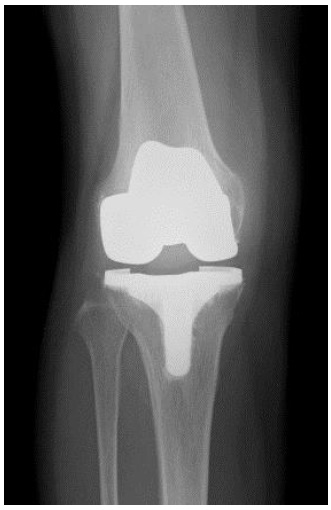
On physical examination, swelling and joint effusion were observed in the right knee joint, and tenderness was not present in the joint space. The range of motion was from 10 to 125°. The results of a meniscal test and a ligamentous instability test were negative. Radiographs showed severe arthropathic changes. Rt TKA was performed. The patient’s symptoms improved after the surgery. Six months later, she developed severe pain in her right knee joint without any obvious cause. The symptoms required transfer to an emergency room and hospitalization. Swelling, local heat and joint effusion were observed in the right knee joint, but redness was not present. Laboratory tests revealed that WBC was 4100 and CRP was 10.70 mg/dl. The aspirated synovial fluid was yellowish and slightly turbid. Bacterial culture and crystal were negative. We considered infection after TKA to be possible, and therefore performed debridement and irrigation. The patient’s symptoms improved after the surgery. However, she exhibited right knee pain and swelling 5 months later. The X-ray images showed no bone erosion or destruction of the right knee (Fig. 2). Although she had no other joint pain or swelling, we suspected she might have contracted rheumatoid arthritis. RF, ACPA and anti-nuclear antibodies were negative, while Matrix Metalloproteinase-3 (MMP3) was 173.1 μg. These findings were highly suggestive of seronegative rheumatoid arthritis. Administration of MTX was initiated at 10 mg/day, resulting in slight improvement of her right knee symptoms. No recurrence of the symptoms has been observed in six years since the surgery.
DISCUSSION
At present, EORA has important clinical distinctions if compared with younger onset. The clinical manifestations include large joint involvement, such as the knee joint and shoulder joint, acute onset of synovitis and prominent systemic complaints. In many cases, joint destruction often occurs rapidly after the onset [5, 6, 9]. In the knee joint, the elderly often have osteoarthritis and undergo conservative therapy such as intraarticular injections of hyaluronic acid. When the patients have severe knee pain and gait disturbance, they are advised to undergo TKA. The differential diagnosis is very important. Elderly patients may have several problems at the same time. The diagnostic process includes careful clinical history, physical examination, laboratory, and imaging examination. If mild swelling, local heat and turbid joint effusion in the knee joint are observed, acute suppurative arthritis, crystal-induced inflammation or EORA may be possible. When bacterial culture and crystal are negative, and RF and ACPA are negative, arthroscopic examination needs to be performed to discriminate the disease before performing TKA. If the diagnosis before performing TKA is osteoarthritis of the knee, the infection after TKA, implant debris-related arthritis and EORA should be considered when swelling, local heat and turbid joint effusion in the knee joint are observed and persist after performing TKA. If bacterial culture and crystal are negative, and the X-ray images show no bone erosion or destruction of the knee, rheumatoid arthritis should be considered.
In the treatment of rheumatoid arthritis, disease-modifying antirheumatic drugs (DMARDs) are the main drugs and should be administered as soon as possible. However, the associated risk of adverse effects and toxicity are elevated in elderly onset RA patients, and EORA patients may be less likely to receive intensive treatment. However, in many cases, the disease activity is high, and joint destruction often occurs rapidly after the onset. These patients should be treated immediately with appropriate DMARDs and biological agents [10].
CONCLUSION
In the patients who have severe knee arthritis without other joint symptoms, the differential diagnosis is very important. The diagnostic process includes careful clinical history, physical examination, laboratory and imaging examination. However, it is difficult to diagnose patients as EORA if rheumatoid factor and ACPA are negative.
LIST OF ABBREVIATIONS
| ACPA | = Anti-cyclic citrullinated peptide antibody |
| CRP | = C- reactive protein |
| DMARDs | = Disease-modifying antirheumatic drugs |
| EORA | = Elderly onset RA |
| MMP3 | = Matrix Metalloproteinase-3 |
| MTX | = Methotrexate |
| RA | = Rheumatoid arthritis |
| RF | = Rheumatoid factor |
| TKA | = Total knee arthroplasty |
| YORA | = Younger onset RA |
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.


