All published articles of this journal are available on ScienceDirect.
Minimally Invasive Percutaneous Plate Osteosynthesis Does Not Increase Complication Rates in Extra-Articular Distal Tibial Fractures
Abstract
Background :
Selection of a treatment method in cases of unstable, nonarticular distal tibial fractures is still a matter of discussion. Intramedullary nailing, which is a “gold standard” for tibial shaft fractures, does not always work for this specific transition area between diaphysis and metaphysis. Instead, new minimally invasive techniques with special implants are popular.
Aims :
To determine the functional and radiological results of distal tibial fractures treated with minimally invasive percutaneous plate osteosynthesis (MIPPO) technique.
Study Design :
Retrospective cohort analysis.
Methods :
Thirty distal tibial fractures treated with MIPPO method, between January 2006 and December 2010, were evaluated retrospectively. All patients were classified according to AO/OTA classification. Period of hospital stay, time of fracture union, time to allow full weight bearing, early and late complications were inquired. Functional outcomes were assessed by AOFAS scores.
Results :
There were 13 male and 17 female patients with an average age of 44.26 (range, 22-77 years). One superficial infection and one malunion were observed. Two patients were revised for the loss of reduction and healed uneventfully. According to the AO/OTA classification, 23 patients were 43-A1 (76.6%), 3 were 43-A2 (10%) and 4 were 43-A3 (13.3%). Post-operative mean stay of patients at the hospital was 2.6 ± 1.42 days (range, 1-7 days). Mean full weight-bearing period of the patients was found out as 13.16 ± 2.6 weeks (range, 10-22 weeks). The mean period of union of fracture for patients was found out as 19.8 ± 2.99 weeks (range, 16-34 weeks).
Conclusion :
Treatment of distal tibial fractures with MIPPO method provides a successful treatment strategy as long as used as per the technique, and it respects and does not harm soft tissues which allows early callus formation and rapid healing that enable the patient to walk as early as possible after the operation. The overall clinical and functional outcome is still good despite minor complications.
INTRODUCTION
Selection of a treatment in cases of unstable distal tibial fractures that do not extend over the joint is still a matter of discussion [1, 2]. Various treatment methods such as external fixation, intramedullary (IM) nailing and plate osteosynthesis are described for distal tibial fractures [2-4]. Locked IM nailing is accepted as golden standard in tibial shaft fractures [1, 3]. However, there are concerns about using IM nailing in the distal tibia including the difficulty of fixation of nail in the tibia because of the dimensional change in between the diaphysis and the metaphysis and the risk to advance to the ankle [2].
As a result of open reduction and internal fixation with wide soft tissue dissection and potential periosteal injury, there may be high infection rate, delayed union and non-union [1, 4]. Recently, minimally invasive percutaneous plate osteosynthesis (MIPPO), applied by indirect reduction has been a successful treatment method in cases of lower extremity complex fractures [5, 6]. The studies suggest that hematoma loss has negative effect on bone healing [7]. The real goal with MIPPO is to protect osteogenic hematoma in the fractured region and the arterial nutrition in the bone from iatrogenic soft tissue damage [8]. Vascular injection studies have shown that MIPPO technique preserves periosteal circulation in the highest level when compared with classical open technique [8, 9]. With the increase in findings which indicate the significance of biological factors in bone healing, the practice of opening the fracture line by means of anatomical reduction and stable fixation and cleaning the hematoma and then freely stabilizing fractured fragments shifted to the practice of protecting fracture hematoma [10-12].
Locking compression plating (LCP) provides angular stability for fixation of fractures [13]. The anatomical shape of the plate prevents malalignment of the fracture, and provides right angular and axial weight distribution [8]. Locked screws prevent the plate from applying pressure on the bone and do not harm periosteal circulation [5]. The goal with the implants used is to obtain an easy fracture union without disrupting the biological structure.
Our goal with this study is to evaluate the results of our patients with extra articular distal tibial fractures whom we treated using MIPPO technique with LCP plate, in terms of functional and radiological results, period of stay in the hospital, period of union, period of bearing weight and the complications.
MATERIALS AND METHODS
Thirty distal tibial fractures of 30 patients treated with MIPPO method between January 2006 and December 2010 were evaluated retrospectively. Post-operative early and late complications such as deep or superficial infections, delayed union, nonunion, malunion, implant failure, period of hospital stay and time of fracture union were inquired (Table 1).
The distribution of the cohort in terms of gender, age and AO/OTA classification.
| n | |
|---|---|
| Gender Male Female |
17 13 |
| Age | 44.26 (22-77 years) |
| AO/OTA Classification 43-A1 43-A2 43-A3 |
23 (76.6%) 3 (10%) 4 (13.3%) |
The follow-up period, postoperative stay, total period of stay, full weight bearing, union periods and AOFAS scores of the patients.
| Mean | ± SD | |
|---|---|---|
| Follow-up period | 14.46 months | ± 3.73 months |
| Post-operative stay at the hospital | 2.6 days | ± 1.42 days |
| Total period of stay at the hospital | 4.6 days | ± 1.95 days |
| Full weight-bearing period | 13.16 weeks | ± 2.6 weeks |
| Period of union of fracture | 19.8 weeks | ± 2.99 weeks |
| AOFAS Score | 88.3 | ± 10.8 |
Fractures extending to the ankle joint, pediatric fractures, stress fractures and pathologic fractures were excluded.
All fractures were reduced closely and stabilised with a plaster splint immediately after admission in emergency service. The patients with severe soft tissue injury and oedema were treated with elevation and cold application till soft tissue was healed and the oedema disappeared.
All patients were classified according to AO/OTA classification [14].
Surgical Technique
The patient was laid down supine on the operation table. A pillow was placed under the buttock. Manual traction under fluoroscopy was applied for indirect reduction of the fracture and the alignment was obtained. The reduction was checked with fluoroscopy to achieve reduction compatible with the criteria of Kretek et al. [15]: rotation less than 10o, cortical contact more than 50%, shortening less than 10 mm, angulation less than 5o coronal and 10o in sagittal plane.
All patients with lateral malleolar fractures and fibular shaft fractures along with shortening were operated with 1/3 tubular plate in order to adjust length and alignment. Anatomic LCP plate or precontoured flat metaphyseal LCP plate of 3.5 - 4.5 mm has been applied from a small incision over the medial malleolus, well away from the fracture line. The plate was temporarily fixed by means of a K wire on its proximal and distal point, and its compatibility with the bone was checked under fluoroscopy in AP and lateral plan. Afterwards, the plate was taken closer to the bone by means of one cortical screw. At least 3 locking screws passing through both cortices were applied on each fracture fragment according to the bone quality. After the operation, all patients were routinely followed by elevation, cold and bandage application on the extremity. Antibiotic prophylaxis with first generation cephalosporin was applied to all. As of day one, the patients started passive and active knee and ankle exercises. They were mobilized by means of double crutches stepping on the intact extremity. The patients were evaluated at the second week, first, third, sixth months and a year after the operation for both clinical and radiological control. During clinical examination, any wound problem, deformity, ankle and knee range of motion and patients’ compliance to the rehabilitation protocol were observed. With bidirectional radiographic examination, callus formation was inquired [16]. According to callus formation, full weight bearing was started (Fig. 1). Functional outcomes were assessed by AOFAS scores.
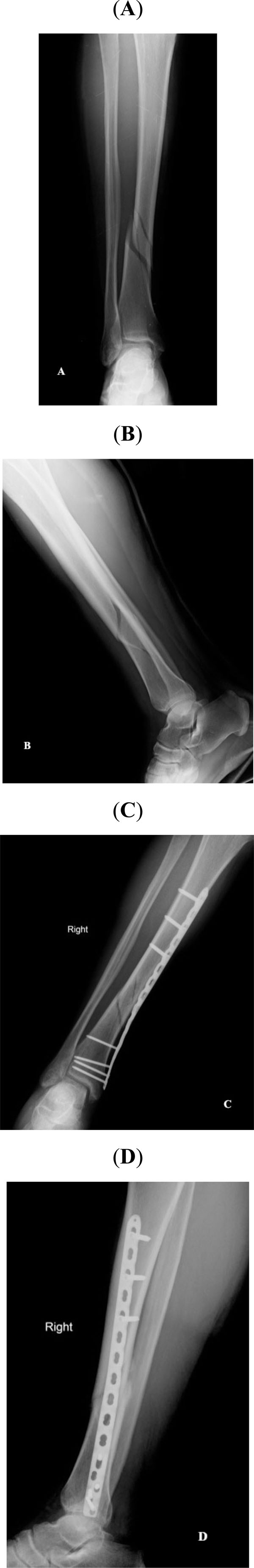
(A, B) Anteroposterior and lateral radiograph of a 34 years old male patient having distal tibial fracture. (C, D) Anteroposterior and lateral radiograph of the same patient at postoperative 2nd month.
Statistical Analysis
Collected data were analyzed in SPSS for Windows 11.5 package program. Mean and standard deviations were calculated for numerical variables while frequency and percentage were calculated for categorical variables.
Informed consent was obtained from each patient.
RESULTS
There were13 male and 17 female patients with an average age of 44.26 (range, 22-77 years). According to the AO/OTA classification, 23 patients were 43-A1 (76.6%), 3 were 43-A2 (10%) and 4 were 43-A3 (13.3%). According to the Gustillo-Anderson classification, 2 patients (6.6%) had type 1 open fracture (Table 1). We performed operation on 17 of the patients (56%) in the first 24 hours while we operated 10 of them (33%) in the first 72 hours. Seven of the patients with lateral malleolus fractures were treated by open reduction and internal fixation with 1/3 tubular plate. 11 of the patients having minimally displaced fibula shaft fracture were followed by conservative treatment. One of the patients had medial malleolus fracture, and it was fixed by open reduction and internal fixation.
Post-operative mean stay of patients at the hospital was 2.6 ± 1.42 days. Mean total period of stay at the hospital was 4.6 ± 1.95 days. Mean follow-up period of the patients was 14.46 ± 3.73 months. Mean full weight-bearing period of the patients we followed up, was found as 13.16 ± 2.6 weeks. The mean period of union of fracture for patients was found as 19.8 ± 2.99 weeks. The mean AOFAS score was 88.3±10.8 (range, 54-98). There were 18 (60%) excellent, 7 (23.3%) good, 3 (10%) fair and 2 (6.7%) bad results (Table 2).
In terms of complications, one of our patients developed superficial infection, resolved with antibiotherapy and debridement. We did not experience any deep infection or osteomyelitis. During follow up, we observed angulation in sagittal plane in one and in coronal plane in two patients. Sagittal plane angulation was 10 degrees and followed conservatively and healed without any problem. Two coronal plane (valgus) angulations were revised (one with again a LCP plate at fourth month and the other with an intramedullary nail at third month). They both healed well after revision.
DISCUSSION
Diaphyseal-metaphyseal bone region is under risk in terms of periosteal blood flow. MIPPO technique preserves the hematoma in the fractured area while at the same time it prevents iatrogenic soft tissue injury and additional osseous-vascular damage that happens in open surgery [17, 18]. Large surgical exposures, which are required for absolute fixation, gave way to the minimally invasive techniques in which aligning two adjacent joints of long bones anatomically or nearly anatomic position without any rotation is generally sufficient. The method employed involves using plates and screws internally in a similar way to the principles of external fixator. Among its most important advantages is that it gives minimal damage to the periosteum due to minimal contact with the bone. Currently, sufficient stability for early functional treatment and sufficient instability for speeding up the healing have begun to be the essential principles of fracture healing [11]. Therefore, we aimed to analyse the results of distal tibial nonarticular fractures treated in line with these principles, with MIPPO technique, on this particular area of tibial bone where alternative techniques are still debateful. We inquired whether this technique is efficient in both clinically and functionally. We also explored whether this technique, by considering the biology of fracture healing excessively, provides early healing and union with early functional improvement. Our results suggest that, although this fracture type is prone to early and late complications naturally, MIPPO is simple, reliable and effective if applied according to the rules of the technique.
There are some limitations of our study. First is the retrospective nature of the study. Another limitation is the lack of a control group that we may compare the results.
In case series, positive results have been published with regard to infection and nonunion rates with MIPPO technique [1, 19]. In contrast, Lau et al. reported 7 cases of late infections among 48 patients (15%) that were operated with MIPPO technique, during a 3-year follow up [20]. They concluded that MIPPO fixation of distal tibial fractures is safe and efficient although complications such as late wound infection and skin impingement by the implant are relatively common. We had only one patient who developed superficial infection, and that patient was healed with antibiotherapy without a necessity for surgical intervention.
Borg et al. [21] reported surgical technique and results of a series of 21 patients. They reported that 14 patients had fracture reduction being anatomic or close to anatomic without angulation. They reoperated 2 patients due to malreduction. In early post-operative period, we have observed anatomic or close anatomical reduction except 1 patient who had 10o angulation to anterior. The patient did not accept a revision and the fracture healed uneventfully.
Unlike the case with absolute fixation, biological techniques call for alignment in the manner of bridging without applying compression to the fracture line. In that way, relative fixation is obtained. Such fixation is elastic. Micromotion occurs in the fracture line, and stability begins to develop along with the formation of callus [11]. Callus that is formed within biological system falls within secondary callus formation unlike absolute fixation. Medullar and periosteal callus provides healing in such bones [22, 23]. Number of the screws to be used as per plate-screw intensity must be 0.4 to 0.5 times lesser than the number of all holes of the plate. Filling all holes and putting the screws too close to the fracture line will cause stress intensity, and elastic fixation will be disrupted [24]. Abiding by these rules, we observed 18o of valgus angulation in one of our patients at the 3rd month follow-up, who was revised with tibial intramedullary nail; 20 o of valgus angulation in the other at 4th month, who was revised again by MIPPO, also. We experienced that these losses of fixation were due to stress intensity. We believe that surgical technique has great significance in MIPPO, sustainability of fixation system and healing of fracture as a result.
In a study carried out by Redfern et al. [1], 20 patients with unstable, closed distal tibial fractures were operated with MIPPO. They suggested partial weight bearing (10-15 kg) in the post-operative first day without a need for plaster cast. They reported that average full weight-bearing period is 12 weeks (range, 8-20 weeks), and average union period is 23 weeks (range, 18-29). We allowed our patients to bear weight as early as tolerated, and we did not face any implant failure due to early weight bearing. We found that average full weight-bearing period of our patients is 13.16 weeks (range, 10-22 weeks) and average union period is 19.8 weeks (range, 18-34 weeks), which are similar with the literature [19, 25, 26].
CONCLUSION
We have obtained quite satisfactory results with MIPPO for the distal diaphyseal-metaphyseal tibial fractures. Considering other methods that can be used for the same areas, we have not come across with major complications that may affect the result. MIPPO method provides a successful treatment strategy as long as used as per the technique, and it respects and does not harm soft tissues in cases of distal tibial fractures. It also enables early mobilization and rehabilitation without any external support. The overall clinical and functional outcome is still good despite minor complications.
CONFLICT OF INTEREST
There is no conflict of interest in connection with this paper. There was no financial contribution to the work being reported.
ACKNOWLEDGEMENTS
Declared none.


