RESEARCH ARTICLE
Traumatic Floating Knee: A Review of a Multi-Centric Series of 172 Cases in Adult
J.-M. Feron*, 1, P. Bonnevialle2, G. Pietu3, F. Jacquot11
Article Information
Identifiers and Pagination:
Year: 2015Volume: 9
First Page: 356
Last Page: 360
Publisher ID: TOORTHJ-9-356
DOI: 10.2174/1874325001509010356
Article History:
Received Date: 21/02/2015Revision Received Date: 26/04/2015
Acceptance Date: 18/5/2015
Electronic publication date: 31/7/2015
Collection year: 2015

open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
Abstract
The traumatic floating knee in adults (FK) is a combined injury of the lower limb defined by ipsilateral fractures of the tibia and femur. The first publications emphasized the severity of injuries, the bad results after conservative treatment, the most severe functional outcome in case of articular fracture and the frequency of associated cruciate ligament injuries. The surgical management of FK has been highly modified according the improvement of the fracture fixation devices and the operative techniques. This retrospective multicentric observational study included 172 adults with a FK injury admitted in emergency in 5 different level I or II trauma centers. All the patients data were collected on an anonymized database. Results were evaluated by the overall clinical Karlström’s score at latest follow-up. Fracture union was assessed on X-rays when at least 3 out of 4 cortices were in continuity in two different radiological planes. A statistical analysis was performed by a logistic regression method. Despite some limitations, this study confirms the general and local severity of this high-energy trauma, mainly occurring in young people around the third decade. A special effort should lead to a better initial diagnosis of associated ligamentous injury: a tear of PCL can be suspected on a lateral-ray view and a testing of the knee should be systematically performed after fixation of the fracture under anesthesia. Secondary MRI assessment is sometimes difficult to interpret because of hardware artifacts. The timing of fracture fixation is discussed on a case by case basis. However, a first femoral fixation is recommended except in cases of tibia fracture with major soft tissue lesion or leg ischemia requiring the tibia fixation first. Also a tibia stabilized facilitates the reduction and fixation of a complex distal femur fracture. The dual nailing remains so far for us the best treatment in Fraser I FK. Further prospective studies are needed to validate treatment algorithms, best fixation techniques in order to decrease the rate of complication and improve the functional outcome of floating knee injuries.
INTRODUCTION
The traumatic floating knee in adults (FK) is a combined injury of the lower limb defined by ipsilateral fractures of the tibia and femur. The word was introduced first time by McBride and Blake [1]. This disruption of the skeletal integrity on each part of the knee is usually the result of a high energy trauma that explain the high rate of associated lesions and complications.
According to Fraser et al. [2] The FK includes various patterns: bi-diaphysis fractures (type I), mixed diaphysis fracture on a bone and epiphyseal fracture on the other (type II A, B) and bilateral epiphyseal (IIC) (Fig. 1). The first publications emphasized the severity of injuries, the bad results after conservative treatment [3-10], the most severe functional outcome in case of articular fracture [11-13] and the frequency of associated cruciate ligament injuries [14, 15]. The surgical management of FK has been highly modified according the improvement of the fracture fixation devices and the operative techniques [16-23]. The FKprognosis in the context of high-energy trauma is reserved [24-30] and application of principles the orthopaedic damage control finds its place [31, 32]. The objectives of this multicenter study were to determine the patterns of the lesions, the care management and the outcomes in order to identify the prognosis factors and to optimize therapeutic solutions.
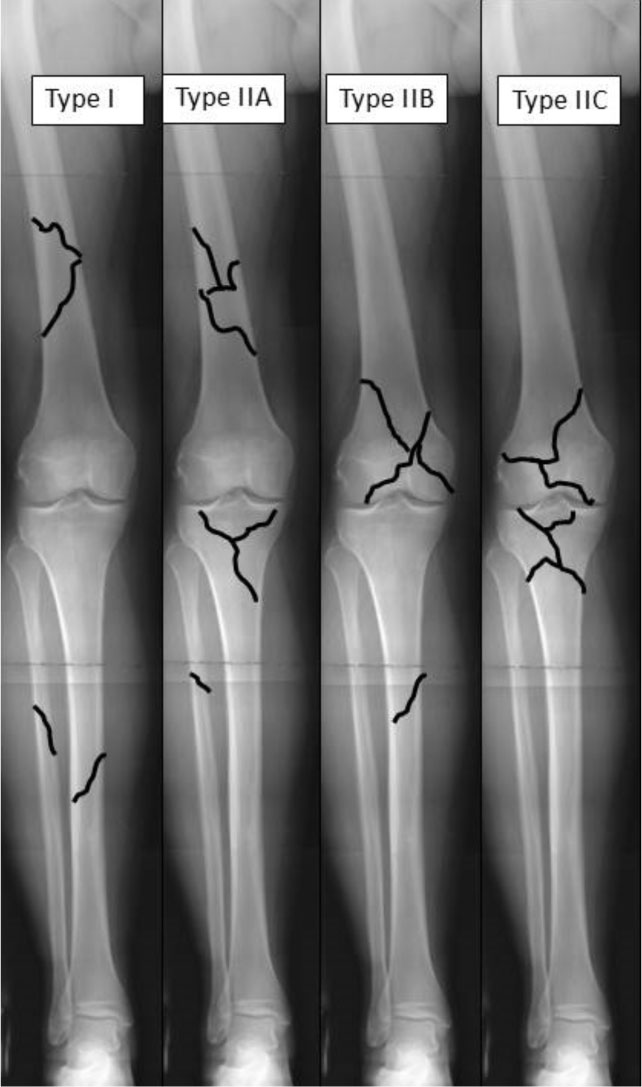 |
Fig. (1). Schematic representation of the Fraser's classification. |
 |
Fig. (2). Dual nailing ( femur retrograde ad tibia anterograde ) using a single knee approach. |
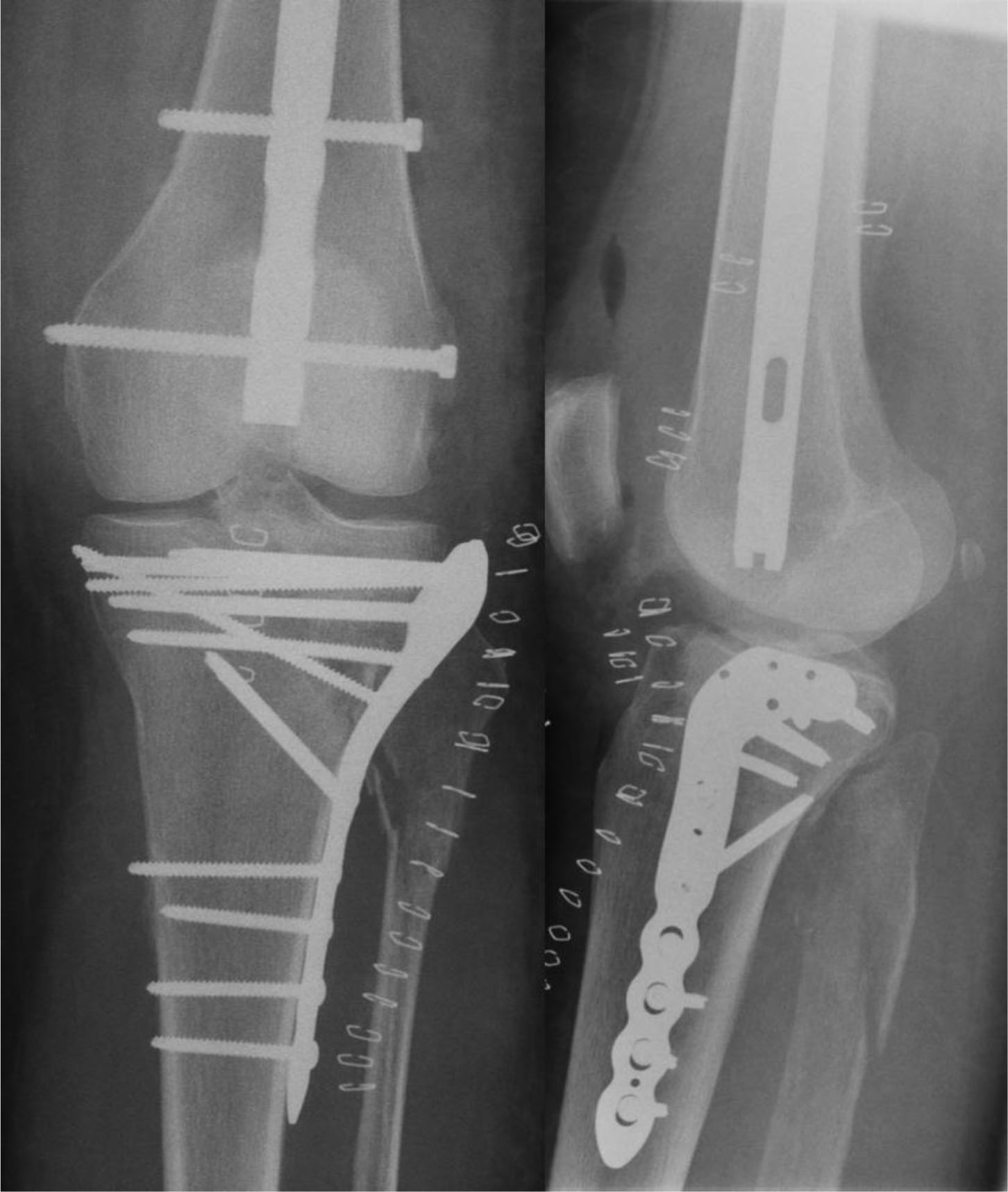 |
Fig. (3). Combined (plate and nail) fixation. |
Results according to Karlström and Olerud score.
| Karlström & Olerud Score |
@12 Months (n= 116) |
@ 24 Months (n=89) |
|---|---|---|
| Excellent | 23 (20%) | 15 (17%) |
| Good | 38 (33%) | 33 (37%) |
| Fair | 35 (30%) | 30 (34%) |
| Bad | 20 (17%) | 11 (12.5%) |
MATERIALS AND METHODS
This retrospective multicentric observational study included 172 adults with a FK injury admitted in emergency in 5 different level I or II trauma centers. All the patients data were collected on an anonymized database (FileMaker pro®). Data included patient’s demographics, AO classification of fractures [33], the Injury Severity Score (ISS) [34]. The FK was classified according the Fraser’s classification. Characteristics of surgical treatment were detailed for each patient as well the occurrence of complications and the length of stay to hospital discharge.
Results were evaluated by the overall clinical Karlström’s score at latest follow-up [6]. Fracture union was assessed on X-rays when at least 3 out of 4 cortices were in continuity in two different radiological planes. A statistical analysis was performed by a logistic regression method using the Statview® software
Among the 172 patients, 37 were women and 135 were men. Age ranged from 15 to 93 years (mean 31) but 50% were less than 25 years old at the time of injury. The most common cause of injury was a traffic accident in 90% of cases. The left sides was more affected than the right (60.5% vs 39.5%) The mean ISS was 19.5 (9-75), it was greater than 18 in 64 patients (37.3%). Among these multiple injured patients, 38% had a severe head injury, 25% a combine head-thorax injury and 68% (n=117) had one or more other limb fracture. The associated fractures on the contralateral limb involved the femur in 28 cases, the tibia plateau in 22 cases and the tibia pilon in 7 cases.
The fracture was open in 38% of cases at the femur level and in 57% at the tibia level.
Eleven patients were in ischemia at admission, 17 patients presented a sciatic nerve palsy and 4 patients had a compartmental syndrome of the leg.
According the Fraser’s classification we had 71.5% type I, 8.2% type IIA, 11.6% type IIB and 8.7% type IIC
Fixation of all femur fractures was performed in emergency mainly by IMN (n=123, 34 were retrograde nailing) (Fig. 2), 23 external fixation (EF), 12 plates (PL) and 13 combined techniques (Fig. 3).
The tibia fractures were treated by IMN (93), EF (43), and PL (11), combined techniques (11) and 14 non-displaced fractures conservatively. An anterograde femur and tibia nailing was the treatment. For a little more of the half of the series (n=88), an anterograde IMN at both level was performed.
Fractures were fixed within 6 hours after admission in 62% of patients. The femur was first fixed in 73.6% of cases using a traction table in 53%.
The average operating time was 95 minutes (45-210) for the femur and 75 minutes (30-200) for the tibia. The cumulative average operating time for both sites was 167 minutes with a maximum of 300 minutes.
Among the 11 patients in ischemia, 6 had a repair vascular surgery on the popliteal artery and the ischemia time varied between 180 and 600 minutes. Delayed soft tissue coverage by flaps was necessary in 9 patients.
The overall average length of stay in hospital was 30 days (3-165), 100 patients needed to stay in ICU over five days.
RESULTS
The mean follow up was 34.2 months (1.3 to 136.8). The follow up was more than 12 months for 126 patients (73%) and more than 2 years for 97 patients (56%). Five patients early died from multi-organ failure due to multiple trauma injuries. Early systemic complications occurred in 24 case (14%): 5 ADRS (fat embolism) and 7 DVT without pulmonary embolism. 56 patients (32.6%) presented local complications directly related to the FK; the most severe were 6 compartmental syndrome and 10 secondary skin necrosis. Non-union at one of the both site occurred 36 times (21%) including 22 septic cases. Forty-one surgical revision surgery were performed, ten time for bone grafting.
The clinical result was assessed by the Karlström and Olerud score. At 12 months (n = 116) the results were excellent in 23 patients (20%), Good in 38 (33%), fair in 35 (30%) and bad in 20 times (17%) (Table 1). Over 2 years (n = 89) the results were almost similar: excellent 15 (17%), good 33 (37%), 30 fair (34%) and bad 11 (12, 5%).
At latest follow 19 patients (13%) complained of a knee pain and swelling. Loss of knee extension was more than 5° with a maximum of 40° in 13 patients. The mean active knee ROM was 114° (0 - 150), 9 out of 10 patients had an active flexion over 90°. Instability was present in 11 knees, all these knees had a central pivot injury initially diagnosed. Failure of anatomical reduction of an articular surface was present in 16 knees. 20 patients had a malalignment (>7° deviation) of the injured limb in frontal plane (10 in varus and 10 in valgus) or in the sagittal plane (6 flessum and 10 recurvatum)
The Karlstrom’s score was significantly dependent to the level of the femoral fracture: when the fracture involved the middle third of the femur, we found 66.2% of good or excellent results while they drop to 12.5% when located at the distal third fracture and none at the proximal third. The others factors lowering the rate of excellent and good results were the presence of a comminuted fracture (32% vs 66.3%), the opening of the fracture (14% vs 35%). The extra-articular lesions, FK type Fraser I, had less bad results (10.6%) than in case with at least one articular fracture, FK type Fraser II (42.4%). The occurrence of septic complications impaired negatively the result with 42% of bad results instead of 15% when there is no history of infection. In the cases with an associated vascular injury, there was only 10% of good results without any excellent.
The mean knee ROM is correlated with the type of FK. It was 114.4° in FK type I. In type II FK, the results depend of the location and number of articular fractures, the mean knee ROM was 121° in type II A, 99.4° in type IIB and 77.1° type IIC. Unsurprisingly we find the same factors that have negatively affected the overall score of Karlstrom affecting the joint mobility: better mean ROM for middle third fracture of the femur (122°) the proximal and the distal (respectively 97° and 77.5°). In open fracture the mean ROM decreased with the opening of the fracture (71° vs 115.6°)
The statistically significant risk factors of non-union were the age, sex (24.3% women vs 16.2% men), side of FK (22.1% left vs 16.2% right), the tibia fracture AO42C (50%, 13/26 cases), the femur fracture AO 32C (44%, 12/27 cases). The Fraser type did not seem to influence the risk of non-union (I 22%, IIA 7.1%, IIB 20%, and IIC 13%)
The larger subgroup of FK in this series was the bi-diaphysis fractures (Fraser I) mainly treated by IMN (n=75). We compared femoral anterograde IMN (n=56) and femoral retrograde IMN (n=19). We found no significant difference in the occurrence of nonunion, Karlström’s score or knee ROM between the two nailing techniques. However, there was a significant difference in femoral fixation operative time including the patient positioning: the average time for retrograde nailing was shorter (132 minutes) than for the anterograde nailing (177 minutes). The cumulative operating time of the FK including patient’s installation was 155 minutes when retrograde nail was used and 240 minutes in the anterograde group (p < 0.0001).
DISCUSSION
This study has significant limitations especially the multicentric character, with a quantitative uneven recruitment between the five different centers spread over time (2000-2006), the retrospective setting based on the clinical and radiological data, and an insufficient follow-up to assess joint degeneration over the time. Nevertheless this study is interesting by its large number of cases compared with the series of the recent literature not exceeding few dozen of cases [13, 21, 28].
The epidemiological data and the clinical results confirm what has been published previously. The real incidence of this uncommon lesion remains unknown. The FK is a complex injury much more than a simple ipsilateral fracture of femur and tibia. FK occurs mainly in high velocity trauma like MVA and the frequent associated lesions can be life threatening. Severe complications like early amputations occur with a prevalence of 6% to 27% in the literature, consequences of crush member injuries or prolonged ischemia [13, 16, 18, 23]. Likewise the mortality rate at admission was reported reaching 5.6% to 8.6% [9, 18]. Our study does not include the patients deceased at admission nor the patients treated by primary amputation but within the first week, 3.5% of patients died and 2.9% needed a leg amputation. The most common mechanism of injury was a traffic accident in 9 out of 10 patients, this prevalence of high energy trauma is a feature of all published series [22, 29 Likewise, the associated lesions are common and the mean ISS was around 20 with one third of the cases over 18. All the complications we met: open fractures, compartmental syndromes, vascular injuries, sciatic nerve palsy are highlighted in the previous literature [9, 11, 16, 18, 24, 25]. The ligament injuries are probably underestimated if we refer to the frequency of associated lesions in a prospective MRI study in femur fractures [35]. These lesions often hidden in emergency have several patterns. All type of ligamentous injuries are estimated between 10% and 50%, and between 2% to 10% for the central pivot rupture [2, 9, 11, 12, 14, 15, 18, 24]. In this series, 16 patients had an initial diagnosis of a cruciate ligament and 5 a delayed diagnosis because of a knee instability, representing 12% of the cases. A lack of information about the strategy and timing in cases of surgical repair did not permit further analysis.
The incidence of non-union is rather high (20%) in our study, compared with the rate of recent literature varying from 4% to 11% for the femur and from 3% to 30% for the tibia [21-27, 29, 30]. The predictive factors have been emphasized in the statistical analysis above. Specificity of FK injury makes it difficult to interpret the score Karlström and Olerud [6], also it is incompletely adapted to assess this multilevel lower limb trauma [36]. However, this large series confirm the worst results when one of the fracture involve an articular surface as previously known [21, 23, 26, 36]. Considering the functional outcome, an older age, a vascular lesion, a Fraser type II FK, an open fractures, the amount of fracture comminution, a central pivot lesion are contributing factors of poorer results. The detrimental role of smoking on wound and bone healing has not be evaluated like in other studies [25]. Thus, the Fraser classification of FK remains valid for the overall prognosis: the results worsen between type I and II, then from II A to II C. IMN has demonstrated its effectiveness on fracture healing and its safety in the tibia and femur diaphysis fractures. It was the gold standard in FK Fraser I and we have been able to compare anterograde IMN at both level and the single knee approach combining a retrograde femoral IMN and an anterograde tibia IMN [37-39]. If there is no difference on a functional point of view, the gain in overall operating time is significant, due to a single installation in prone position, either on a standard X-ray transparent table or a traction table depending of the experience of the surgeon. The main criticism of the retrograde IMN technique is to compromise a secondary repair of cruciate ligaments or injure the cruciate ligament insertions. In epiphyso-metaphysis fracture, the variability of techniques used here do not allow, as in any series of the literature, to give strong recommendation [23, 30]. The potential improvement using locking plates and minimal invasive procedure (MIS) could not be evaluate due to a too small number of patients treated by this emerging technique at the time of study.
The principles of damage control orthopaedic (DCO) when patient is unstable or facing complex articular fractures or severe soft tissues lesions is the best safe solution. Definitive fixation, often requiring a long operating time, is delayed till the conditions are best for the patient [30-32].
Conclusion
Despite some limitations, this study help to clarify the FK injury, the management of this unusual lesion and the prognosis factors. It confirms the general and local severity of this high-energy trauma, mainly occurring in young people around the third decade. A special effort should lead to a better initial diagnosis of associated ligamentous injury: a tear of PCL can be suspected on a lateral-ray view and a testing of the knee should be systematically performed after fixation of the fracture under anesthesia. Secondary MRI assessment is sometimes difficult to interpret because of hardware artifacts. The timing of fracture fixation is discussed on a case by case basis. However, a first femoral fixation is recommended except in cases of tibia fracture with major soft tissue lesion or leg ischemia requiring the tibia fixation first. Also a tibia stabilized facilitates the reduction and fixation of a complex distal femur fracture. The dual nailing remains so far for us the best treatment in Fraser I FK. Further prospective study are needed to validate treatment algorithms, best fixation techniques in order to decrease the rate of complication and improve the functional outcome of floating knee injuries
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
We thank for providing us with their cases the members of the GETRAUM (Group of study and research in trauma care) of the SOFCOT: J.-C. Bel, F. Molinier, H. Niéto, L. Obert and L. Pidhorz.







