All published articles of this journal are available on ScienceDirect.
10-Year Survival of Acetabular Reinforcement Rings/Cages for Complex Hip Arthroplasty
Abstract
Introduction :
Acetabular reinforcement rings/ cages (AR) are commonly used for reconstruction of bone defects in complex hip arthroplasty. The aim of this study was to retrospectively investigate the 10-year survival rate of Ganz reinforcement rings and Burch-Schneider cages used in a single institution.
Material and Methods :
Between September 1999 and June 2002 all ARs, implanted in one institution, were identified. All patients had regular clinical and radiographic follow-up and were included in this study. Their prospectively collected clinical and radiographic data was retrospectively analyzed. In case of death before the 10-year follow-up examination, patient’s families or their general practitioner was contacted by telephone. The main outcome measures were survival of the ARs and kind of revision surgery.
Results :
The 10-year survival rate was 77.7%. At 10-year follow-up, 5/60 (8,3%) patients could not be located and had to be excluded therefore. 27/55 (49,1%) were dead, whereof 22 had no revision of the ARs before death (after a mean of 66 months; range: 0 - 123). Of the remaining 28/55 (50,9%) patients, 23 patients (24 ARs) had no revision of the ARs.
Conclusion :
Despite the high mortality rate of this study’s collective, ARs for complex primary or revision total hip arthroplasty provided predictable long term results.
Level of Evidence :
Clinical investigation.
INTRODUCTION
Acetabular reinforcement rings/ cages (Ganz Rings and Burch-Schneider Cages) (ARs) are commonly used for reconstruction of severe bone defects in complex hip arthroplasty [1-5]. They are implanted in revision hip arthroplasty with periprosthetic acetabular bone resorption in most of the cases, in deficient dysplastic acetabula or in primary total hip arthroplasty on occasion.
The Ganz Ring (Fig. 1) – also known as acetabular roof reinforcement ring with hook – has been used by Ganz routinely for acetabular reconstruction since 1989 [2]. It is designed for reconstruction of acetabular floor or cavitary defects and smaller defects of the lateral border of the acetabular rim. Further on it allows the anatomical restoring of the center of rotation. An intact inferior part of the acetabulum is required for anchoring the hook in the incisura acetabula. Concerning the survivor rate of this implant long-term results of 10 years are available [2, 4, 6-9]. When the inferior border of the acetabulum is deficient for anchoring the hook a different implant is needed. The Burch-Schneider Cage (Fig. 2) – also known as ‘anti-protusio cage’ – was designed by Burch in 1974 and subsequently modified by Schneider in 1975 [10, 11]. With the use of the Burch-Schneider Cage more severe bone defects of the acetabulum rim and the cranio-lateral border of the acetabulum can be treated and larger areas of acetabular bone loss can be bridged. Safe fixation of the proximal flange to the ileum and insertion of the nose into the ischium is required for primary stability of the implant. It was Müller using the Burch-Schneider Cages in revision hip arthroplasty since 1975 [10] who firstly presented long term results after 5 and 8,5 years of 76 % and 79 % implant survival rate. [5, 10, 11] In the meantime, there are several studies revealing long-term results of 10 years or more [7, 12-17].
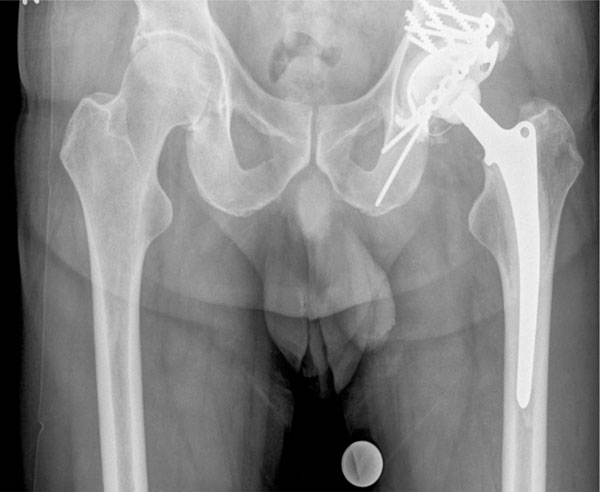
Implantation of a Ganz Ring.
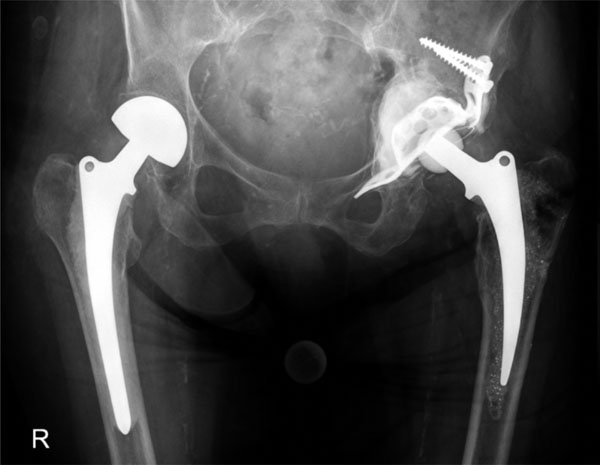
Implantation of a Burch-Schneider cage.
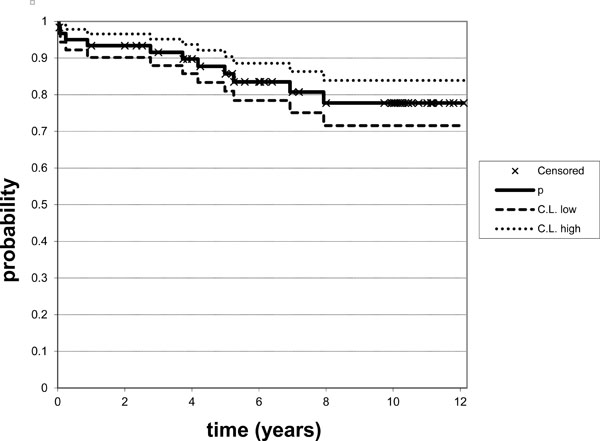
Kaplan-Meier implant survival analysis showing a 77,7% survival rate after 10 years.
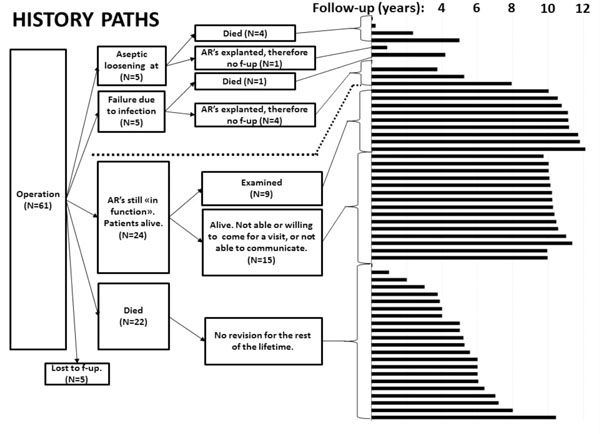
History paths (Patient/ AR-information).
It was the aim of this retrospective clinical study to investigate the 10-year results of ARs implanted in our center in the period from 1999 until 2002. Main outcome measure was survival of the ARs. End point was revision surgery for any reason.
MATERIALS AND METHODS
Between September 1999 and June 2002 all ARs implanted in our hospital were identified. A total of 61 ARs (42 Ganz Rings, 19 Burch-Schneider Cages) in 60 (one bilateral) consecutive patients (male: 34, female: 26; mean age 72 years; range: 47 - 92) had been implanted in the observed period of time. The decision to use the Ganz Ring or the Burch-Schneider Cage was made intraoperatively depending on the extent of the bone defects. No bone substitutes were used. The surgical approach was either lateral or anterolateral.
The indications for the implantation of the 61 ARs were following: aseptic loosening in 38 cases, septic loosening in 2 cases allowing a one-step implant revision and re-implantation after a two-step implant revision/Girdlestone procedure in 9 cases, dislocation of the cup after primary total hip replacement in 3 cases and fractures with severe acetabular bone defects in 9 cases (Table 1).
Indications for the implantation of ARs.
| Aseptic loosening | 38 |
| Septic loosening (1 step) | 2 |
| Septic loosening/ Re-Implantation (2 step) | 9 |
| Fractures with acetabular bone defects | 9 |
| Dislocation of the cup after primary THR | 3 |
A regular clinical and radiographic follow-up after primary total hip arthroplasty or revision hip arthroplasty is routinely conducted in our center after 10 years. The local IRB approved the study. All patients were traced and invited to clinical and radiological follow-up 1, 5 and 10 years after surgery. In case of unavailability or death family members or the general practitioner were contacted. All living patients contained a physical examination, a clinical score (Harris Hip Score) and a two-plane X-ray evaluation after ten years. 9/61 patients could finally fulfill the examination. All deceased patients were taken into the study – in every case the status of the implant could be identified.
We used Kaplan-Meier survival analysis to calculate the survivorship curve.
RESULTS
Kaplan-Meier survival analysis revealed a 10-year survival rate of 77.7 % (95 % CI: 0.72-0.84. Fig. 3). At 10-year follow-up, 5/60 (8,3 %) patients were lost to follow-up and had to be excluded therefore. 27/55 (49,1%) were dead, whereof 22 had no revision of the AR before death (after a mean of 66 months; range: 0 - 123). Of the remaining 28/55 (50,9%) patients, 23 patients (24 ARs) had no revision of the ARs after a mean follow-up of 123.2 months (range: 120 - 139). 46 of 61 ARs had not been revised at the 10-year follow-up (Fig. 4).
10/55 (18,2%) ARs had been revised after a mean time of 35 months (minimum of 1 and a maximum of 99 months). The reasons for revision were following: septic loosening leaving a Girdlestone situation after removal (5 (9,1%)) and aseptic loosening requiring complete acetabular revision (5 (9,1%)).
Further complications without revision of the ARs were reported in 4 (7,2%) patients having dislocations followed by closed reduction without further operation and 2 (3,6%) persons having revisions of the cemented inlay because of mal-positioning leaving the ARs in place.
All living patients had a 10-year radiographic follow-up. There were no relevant radiographic differences between the two implants used, however we did not analyze any radiographic details.
If AR’s have been revised or explanted for any reason (septic or aseptic loosening) there was no rationale for a follow-up examination that would bring no information about the implant. We therefore did not want to discomfort the patients and only interviewed those that were still alive.
Only 9 living patients could finally fulfill the examination.
DISCUSSION
This retrospective clinical study investigated the 10-year results of 61 acetabular reinforcement rings/cages (Ganz Rings and Burch-Schneider Cages) (ARs) implanted in revision hip arthroplasty in most of the cases but also in complex hip arthroplasty between 1999 and 2002. Our study showed a 77,7% implant survival rate after 10 years with revision of the ring/cage as the end point.
Due to the mean age of 72 years of our patient´s collective at the time of surgery we decided to investigate only the implant survival rate. This was a consequence of the relatively high average age of 82 years at the 10-year follow-up. Secondly, only 9 living patients could have been seen for clinical and radiographic examination. The small number of 9 available patients provided us with limited information and brought no information about the implant. It affected us to exclude the initially planned examination parameters like clinical scores (e.g., Harris-Hip-Score) and functional and radiographic outcome. Not knowing about the radiological outcome and about any radiological lucency or loosening is a weakness of this study. On the other hand it is a strength of this study that we could identify every single acetabular implant´s history between 1999 and 2002 despite the average age of 82 years of our patient´s collective.
27/55 patients (49,1%) had died from causes unrelated to the operation procedure at the 10-year follow-up. Compared to the study of Siebenrock et al. [8] who had a mortality rate of 33% ours is higher. This can be explained by the almost 10-year higher average age of 72 years at the time of surgery compared to their 63 years on average. Gerber et al. [6] reported even a lower mortality rate of 24% after 10 years with a mean age of 69 years at the time of surgery. Schlegel et al. [4] manifested a mortality rate of 24% but the mean follow-up period contained only 4 years. Jones [7] reported a 13% mortality rate after a mean follow-up of only 7 years. In summary the reasons for the relatively high mortality rate of 49,1% remain unclear and can only be explained by the increasing co-factors and complications of the patients with the increasing age at the time of the operation.
Regarding only the mean age of 72 years at the time of the surgery and comparing it with other studies our series revealed higher average values [6, 8, 13, 18, 19].
Looking at the share of patients which had been lost to follow-up we are equal to others with 8,3% (5/55 patients) in our collective [6, 11, 20].
The first long-term results using Burch-Schneider Cages for acetabular revision arthroplasty were published in 1992 by Berry et al. [10]. in 1995 by Peters et al. [20] and in 1998 by Gill et al. [11] They showed implant survival rates of 76% (32 hips) after 5 years, 100% (28 hips) after 33 months and 79% (58 hips) after 8,5 years on average. Lately reported follow-up periods of 10 years or more demonstrated survivorship rates of 87,5% (56 hips) after 11.7 years and 72,2% (18 hips) after 13,5 years published by Regis et al. [15,16] Elder studies by Wachtl et al. [17] and Bonnomet et al. [13] with long-term results indicated survival rates of 78,9% (38 hips) after 12 years and 78% (21 hips) after 10 years on average.
Regarding the implantation of Ganz Rings for acetabular revision arthroplasty the earliest long-term results published by Gill [2] in 1999 showed a survivorship rate of 93,9% (33 hips) after 6,7 years on average. Longer follow-up periods were presented by Uchiyama et al. [9] and Gerber et al. [6] with 80% (30 hips) and 81% (50 hips) survival rate after 10 years and by Siebenrock et al. [8] with 92% (36 hips) after 11,4 years on average.
CONCLUSION
Despite the high mortality rate of our study’s collective, Acetabular Reinforcement Rings/ Cages for complex primary or revision total hip arthroplasty provide predictable long term results. Our study showed a 77,7% implant survival rate after 10 years and similar long-term results compared to the current literature. We will carry on using the implants.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.


