All published articles of this journal are available on ScienceDirect.
The Dislocating Hip Replacement – Revision with a Dual Mobility Cup in 56 Consecutive Patients
Abstract
Introduction:
Recurrent dislocations of hip replacements are a difficult challenge. One treatment option for recurrent dislocations is the use of a dual mobility cup. The aim of this study was to retrospective investigate the effect of dual mobility cups as a treatment for recurrent dislocations in a consecutive series. Materials and
Methods:
56 consecutive patients were revised in the period November 2000 to December 2010. The mean age at revision was 72 years (SD 11, range 37-92)) and median number of dislocations before revision surgery were 4 (IQR, 2-11). In all cases, revision was made with a Saturne dual mobility cup (Amplitude, Neyron, France). The mean follow-up period was 44 months (SD 30, range 0.1-119).
Results:
One patient (1.8%) experienced a re-dislocation. Three patients (5.3%) had to be revised. One due to disintegration between the femoral head and inner shell, one due to loosening of the acetabular component, and one due to infection. Harris Hip Score improved from a mean of 76 before index surgery to 87 within one year after index surgery.
Conclusion:
This study advocates the use of a dual mobility cup for treatment of recurrent dislocations of THR. However, studies with a longer follow up are needed in order to evaluate implant survival.
INTRODUCTION
Dislocation is one of the major complications following both primary and revision total hip replacement (THR). The incidence is estimated to 2-4% following primary THR. The incidence following revision surgery is even higher and has been reported to be approximately 8% [1]. Dislocation accounts for approximately one third of all revision within a five year period post-operatively and significantly affects the quality of life [2]. Treatment of recurrent dislocations is a difficult challenge.
The use of constrained components is one option for treating recurrent dislocation of THRs. The mean rate of dislocations following revision surgery with a constrained component has been reported to be 10% [3]. Furthermore, constrained components are associated with high rates of aseptic loosening in the long term. Another treatment option for recurrent dislocations is the use of a dual-mobility cup. The dual-mobility concept was introduced in the late 1970s by Bousquet and does not, in contrast to the constrained components, restrict the range of motion in the joint articulation [4]. Few studies investigating the effect of a dual-mobility cup on recurrent dislocations report a dislocation rate of in the range 1.7% to 5.5% following revision surgery [5-8].
The aim of this study was to retrospectively investigate the effect of dual-mobility cups as a treatment for recurrent dislocations of THR in a consecutive series. We focused on dislocation and implant survival following revision surgery.
PATIENTS AND METHODS
Study Design
All patients who underwent revision surgery at The Regional Hospital of Viborg between November 2000 and December 2010 due to recurrent dislocation of their THR were included in this retrospective study. Recurrent dislocation was defined as at least two dislocations. All patients before index revision surgery and within 1 year after surgery seen in our outpatient clinic recorded their Harris Hip Score [9]. Data on a number of dislocations after index revision surgery and implant survival were obtained from medical records. Implant failure was defined as exchange of one or more of the implant components performed after index revision surgery. Data from medical records were crosschecked with data from The National Patient Register in order to ensure completeness of our data on dislocation rates and implant survival. Closed reductions or revision surgery conducted in other hospitals are recorded in The National Patient Register. Where relevant, date of death was obtained from The Central Office of Civil Registration. The Danish Data Protection Agency, and the Danish Health and Medicines Authority approved this study.
Index Surgery and Implant Components
All patients with recurrent dislocations were revised with exchange of their acetabular component to an uncemented dual mobility cup. None of the patients had their femoral stem exchanged. Surgery was done through a posterior approach. Patients were post-operatively allowed full weight-bearing and encouraged not to perform flexion above 90 degrees, and internal rotation and adduction above 0 degree for 3 months.
In all cases index revision surgery was done with the Saturne dual mobility cup (Amplitude, Neyron, France). The uncemented Saturn cup consists of two parts (Figs. 1, 2). The first part is an outer shell with a large inside-diameter. The outer shell is made of stainless steel. On the outside, the shell is coated with titanium and hydroxy-apatite. It is highly polished on the inside. The outer shell articulates with the second part, an inner shell made of ultrahigh-molecular-weight polyethylene. The inner shell articulates and envelops the 28 mm femoral head which is locked into the inner shell. If necessary, the outer shell comes with two additional flanges to secure the press-fit fixation with screws placed through the ilium and a hook beneath the teardrop. The tri-polar design of the device makes it theoretically relatively resistant to dislocations [5-10].

The uncemented version of the Saturn cup. From left a 28 mm metal head, PE- liner, and outer acetabular shell. The metal head is locked into the PE-liner making the articulation constrained.
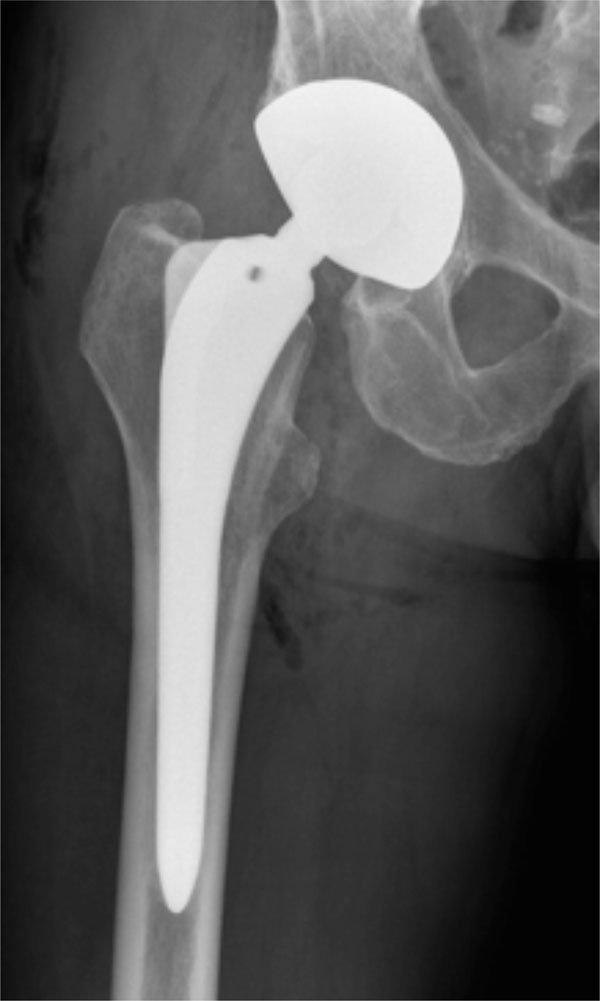
X-ray showing one of our patients after index revision surgery.
Statistics
We used means and 95% confidence intervals (CI) or median values and interquartile ranges to describe study population characteristics. Pre- and postoperative Harris Hip scores were compared using t-test. Kaplan-Meier survival analysis was performed with dislocation as primary endpoint and re-operation after index operation as secondary endpoint. Follow-up started on the day of cup-revision using the Saturn dual-mobility cup (index operation), and ended on the day of dislocation, re-revision, death or 1st of October 2012, whichever came first.
We used Intercooled Stata 9.0 (StataInc, College Station, TX) for statistical analysis.
RESULTS
Characteristics of the Study Population
The study population consisted of 56 consecutive patients (29 males and 27 females). The mean age at revision was 72 years (SD 11) and median number of dislocations before index revision surgery was 4 (IQR 2-11). 66 % of the patients presented 3 dislocations before index revision surgery. In 45 patients (80%), no previous revision surgery had been preformed prior to index revision surgery. The mean follow-up period was 44 months (SD 30).
Dislocation Following Index Surgery
At the time of follow-up, 1 (1.8%) of the hips was dislocated. Attempt of closed reduction was carried out. However, during this procedure of closed reduction the acetabulum sustained a fracture and the acetabular component displaced. The fracture and dislocation hip was managed with open reduction and revision of the acetabular component.
Survival with dislocation as endpoint after 11 years of follow up was 98% (95%CI 86%-99%) (Fig. 3).
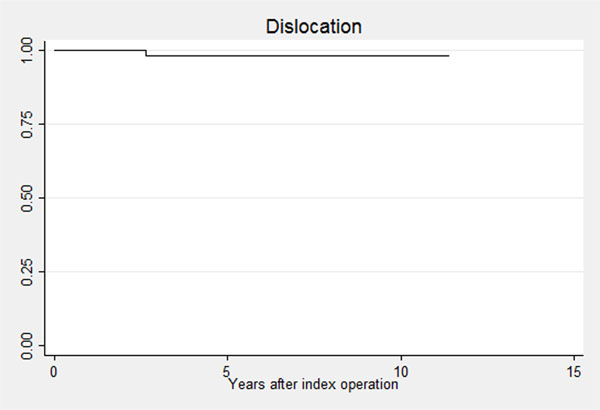
Kaplan-Meier graph with dislocation as endpoint.
Implant Survival and Clinical Outcome
Implant survival with re-revision as endpoint after 11 years of follow-up was 84% (95%CI 49%-96%) (Fig. 4). At the time of termination of follow-up, 3 (5.3%) hips had been revised. One due to disintegration between femoral head and liner, one due to infection, and one due to loosening of the acetabular component.
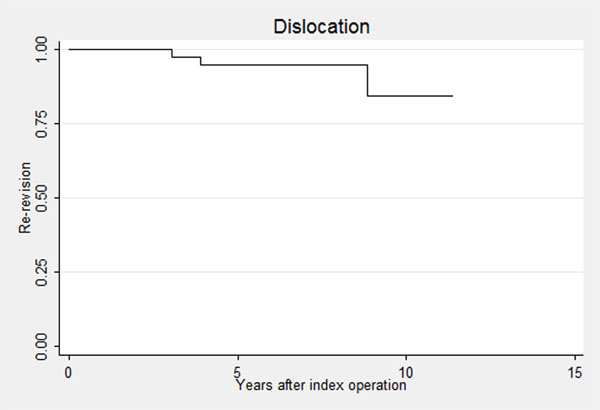
Kaplan-Meier graph with revision of any reason as endpoint.
Harris Hip Score was improved from a mean of 76 (95%CI 70; 82) before index surgery to 87 (95%CI 83; 92) within one years after index surgery (p<0.0001).
DISCUSSION
Recurrent dislocation following THR is a surgical challenge and the outcome of revision surgical can be poor [11]. We found that the use of an uncemented dual mobility cup as treatment for recurrent THR dislocation in 56 consecutive patients resulted in a dislocation rate of 1.8% after a mean of 44 mounts.
Our study is retrospective and thereby limited by the enclosed limitations related to the design. The main limitation is the risk of not being able to assure 100% follow-up on all patients since the main source of data was medical records from our hospital. However, in order to optimize completeness of the data, all patients have been crosschecked with the Danish National Patients Register. This register records among other things surgical and diagnosis codes linked to a personal identification number given to all Danish citizens.
Three major causes of dislocations have previously been described [12]: type I by extreme hip joint position, type II by muscular or soft tissue imbalance, and type III by malposition of one or more of the components. Following revision surgery the important variable for dislocation is probably soft-tissue imbalance [1]. One approach to optimize implant stability and treat recurrent dislocation is revision with a constrained liner. The limitation of this approach is the limited range of motion and relative high re-dislocation rate of 10 % [3]. In this study, we investigated the effect of an uncemented dual mobility cup. We demonstrated a re-dislocation rate of 1.8% after a maximum follow-up period of 11 years and an improvement in Harris Hip Score from a mean of 76 to a mean of 87. Our results are comparable with other studies where dislocation rates between 1.7% and 5.5% have been reported [5-13]. The stability of the dual mobility design is attributed to two factors: first, the relative large diameter head obtained by the mobile liner. Second, the relative large range of motion before impingement of the femoral neck with the metal cup [10].
Two metal-to-polyethylene articulations exist in the dual-mobility design: One between the small metal head and the liner and a second between the liner and acetabular metal cup. This dual articulation design has led to concern about increased wear rates, leading to increased implant loosening and failure [10]. In our study with 56 patients only 3 had to be revised after index surgery. Only one of these re-operations was due to aseptic loosening of the acetabular component. Another concern is disintegration between the femoral head and the liner [13]. In a study investigating the survival of 200 cemented and 28 uncemented dual-mobility cup inserting as a treatment for recurrent dislocation only 18 cups had been revised after a median follow-up of 2 years [6]. Few studies have investigated the survival of dual-mobility cup as a part of a primary THA. One of these few studies following 437 1. generation Bousquet cups and 231 2. generations cup reports a 5 years survival rate at respectively 95.6% and 99.6% [14].
The role of the dual-mobility cups in total joint replacement still needs to be defined. Few studies indicate that dual-mobility cups might have a role in reducing dislocation when treating femoral neck fractures with a joint replacement [15-16]. Other studies encourage to use dual-mobility cups as a part of primary THR [4]. Only one national registry study investigating the implant survival but not the dislocation after revision for recurrent dislocation exists [6].
CONCLUSION
In conclusion, this study suggests effectiveness of dual-mobility cups in the treatment of recurrent dislocations of THRs. However, we are still in need of long term follow-up register studies with focus on both dislocation rates and implant survival in order to determine the role of dual-mobility cups in both primary and revision total hip replacements.
CONFLICT OF INTEREST
The authors declare that they have no conflict of interest.
ACKNOWLEDGEMENTS
In memory of Jorgen Sondergaard who initiated this study and introduced the dual-mobility cup at our department.


