All published articles of this journal are available on ScienceDirect.
Functionality and Safety of an Ultra-Congruent Rotating Platform Knee Prosthesis at 5.6 Years: More than 5- Year Follow-Up of the e.motion® UC-TKA
Abstract
Background:
Mobile bearing TKA prostheses were designed to minimize polyethylene wear by increasing implant conformity and reducing stresses between the articulating prosthesis components. It is the purpose of this study to assess the mid-term functionality and clinical outcome associated with a highly congruent mobile platform design, the e.motion® UC total knee prosthesis.
Material and Methods:
Functional and clinical outcomes were assessed after an average of 5.6 years (5.1 – 6.0 years) after total knee arthroplasty in 28 patients (24 women), aged 77.8±7.5 years. The Knee injury and Osteoarthritis Outcome Score (KOOS) was assessed. Secondary outcomes included the Knee Society Score (KSS), radiological evaluation of radiolucent lines and recording of adverse events.
Results:
The average KOOS subscore for the activities of daily life was 77.8 points after 5.6 years. Both the clinical and functional KSS improved at 2.4 and 5.6 years. Two patients showed radiolucent lines at 5.6 years. Adverse events over 5.6 years included 3 subluxations, 1 tilting and 1 misalignment of the patella. None of the prostheses were revised.
Conclusion:
This pilot study shows promising outcomes for the e.motion® UC prosthesis. In the small sample, the implant performed comparably to the LCS prosthesis (the gold standard). There were no loosenings or revisions observed at 5.6 years.
INTRODUCTION
Primary total knee arthroplasty (TKA) has become a routine operation for the treatment of various severe diseases of the knee joint and is bound to gain in importance as the population ages. TKA aims at restoring the knee's normal function by reconstructing its anatomical mobility while ensuring long-term survival of the implant. Functions of daily life such as walking and climbing stairs are of obvious importance in outcome, allowing the patients a return to an independent life. Implant loosening and polyethylene wear are recognized as major causes of late failure in TKA [1, 2]. The mobile-bearing TKA prostheses, which are characterized by a polyethylene insert that articulates with a metallic femoral component and a metallic tibial tray [1], were designed to minimize polyethylene wear by increasing implant conformity and reducing stresses transmitted to the fixation interface [3]. The e.motion® ultra-congruent (UC) prosthesis is a mobile-bearing TKA prosthesis that features a rotating meniscal component with a highly congruent design. The objectives of this new implant are to avoid contact stress peaks while providing good stability and mobility also in the absence of a posterior cruciate ligament. More specifically, the constant distal radius from -5° to 90° of flexion allows high stability in the midstance phase through a constant ligament tension, thereby reducing the incidence of paradox movement [4]. The primary objective of this pilot study was to assess the general functionality of the e.motion® UC prosthesis in daily life activities, 5.6 years after the TKA index surgery. The results were benchmarked against the Low-Contact Stress knee replacement (LCS; DePuy, Warsaw, Indiana), whose performance at 5.6 years was reported by Lygre and colleagues in 2010 [5]. The secondary objective was to investigate the safety and radiological findings (e.g. early loosening) of the e.motion® UC prosthesis, as well as the knee pain experienced by the patients 5.6 years after the TKA surgery.
MATERIAL AND METHODS
Between March and June 2006, 32 UC rotating platform knee prostheses (e.motion® UC knee endoprosthesis, Aesculap, Tuttlingen, Germany) were consecutively implanted in 32 patients who had unilateral TKA at a private hospital in Angoulême, France. The functionality and safety of the e.motion® UC prosthesis were assessed at an average of 5.6 years (5.1 – 6.0) after surgery as part of the routine clinical care. Intermediate follow-up visits occurred at approximately 3 months, 1.1 and 2.4 years. Because all the tests were part of the routine clinical assessment of patients undergoing TKA (with no additional invasive examinations), the study was approved by the medical committee of the private hospital, as required by French law [6]. In accordance with the 1964 Declaration of Helsinki, all patients provided written informed consent on the day of the 5-year visit, before their inclusion in the study.
Surgical Procedure
The e.motion® UC prosthesis is CE-marked, classified as a Product class III and licensed for medical application to patients (Fig. 1).

Photograph of the e.motion® UC knee prosthesis (Aesculap, Tuttlingen, Germany) featuring a mobile-bearing ultracongruent rotating platform design.
The TKA surgery was performed by the same surgeon (Dr. J.-B. C.). A kinematic navigation system (OrthoPilot®, version 4.2, Aesculap, Tuttlingen, Germany) was systematically used to accurately restore the axial alignment of the implants and to balance the ligaments, aiming at a stable kinematics of the knee [7, 8]. The posterior cruciate ligament was sacrificed in all patients.
Outcomes
Demographics and medical history were obtained 0 to 5 days before surgery. The following Charnley categories applied to knee arthroplasty were calculated: (A) only one knee involved, (B) both knees involved, or (C) comorbidities affecting normal locomotion [9,10].
Knee Injury and Osteoarthritis Outcome Score
The patient´s perception of pain and function was assessed using the knee injury and osteoarthritis outcome score (KOOS) [11-13], which was only distributed at 5.6 years. KOOS is a 42-item, valid and reliable [11,12], self-administered questionnaire that covers 5 dimensions: pain (9 items), other disease-specific symptoms (7 items), activities of daily living (ADL, the primary outcome, 17 items), sport and recreation function (5 items), and knee-related quality of life (QoL, 4 items). Each dimension was scored from 0 (extreme knee problems) to 100 (no knee problems) [11], in accordance with the description given at <www.koos.nu>. The French version of the questionnaire was used [14].
Knee Society Score
The Knee Society Score (KSS) questionnaire was developed as an objective measure of the knee in patients having TKA [15]. It was filled out 0 to 5 days before surgery and at the different follow-up visits. Two scores, each graded from 0 (worst score) to 100 (best score), were calculated: the clinical KSS (using physical examination data such as knee range of motion, and self-reported pain) and the functional KSS (self-reported functional ability during walking) [16].
Radiological Evaluation
Standing antero-posterior, standing medio-lateral and skyline X-rays at 90° of the knee were taken at 2 and 5.6 years to look for evidence of radiolucent lines and subluxation/dislocation. Dislocation of more than 3mm out of the central line was considered a subluxation. Regarding identification of radiolucent lines the methodology described by the American Knee Society was used [17].
Safety Evaluation
All adverse events, complications and any other health-related problems were documented.
Statistical Analysis
The KOOS data at 5.6 years were presented using boxplots. The clinical and functional KSS were compared between pre-surgery and the 2-year visit using a Wilcoxon test. All statistical procedures were performed with SAS, Version 9.2 (SAS Institute Inc. Cary, NC, USA, 2008) with a level of significance set at p<0.05.
RESULTS
During the 5.6-year follow-up, 1 patient died from causes unrelated to knee surgery, 2 patients could not attend the final follow-up visit for medical reasons (persecution mania, severe Parkinson’s disease) and 1 patient was lost to follow-up. The remaining 28 patients were considered for analysis (Table 1).
Characteristics of the 28 Patients who Received an e.motion® UC Knee Prosthesis and Duration of the Follow-Ups
| Mean | ± | SD | Range | |||
|---|---|---|---|---|---|---|
| (min | ; | max) | ||||
| Preoperative Characteristics | ||||||
| Age (years) | 72.4 | ± | 7.5 | (60.0 | ; | 84.0) |
| Height (cm) | 161.8 | ± | 8.0 | (150.0 | ; | 177.0) |
| Weight (kg) | 76.8 | ± | 14.5 | (55.0 | ; | 120.0) |
| BMI (kg/m2) | 29.3 | ± | 5.2 | (23.0 | ; | 42.0) |
| Characteristics at the final follow-up visit (5 years) | ||||||
| Age (years) | 77.8 | ± | 7.5 | (65.5 | ; | 89.7) |
| Duration of the follow-ups | ||||||
| 5-year visit (yrs) | 5.6 | ± | 0.1 | (5.2 | ; | 6.0) |
| 2-year visit (yrs) | 2.4 | ± | 0.3 | (1.9 | ; | 2.7) |
| 1-year visit (yrs) | 1.1 | ± | 0.2 | (0.8 | ; | 1.4) |
| 3-month visit (mths) | 2.9 | ± | 0.7 | (0.07 | ; | 4.0) |
SD: standard deviation.
BMI: body mass index, kg/m2 (= weight/height2).
Twenty-four patients were female (85.7%) and 31 of the patients had a primary diagnosis of idiopathic gonarthrosis. One patient suffered from congenital dislocation of the patella. Thirteen patients had a follow-up visit at 1 year (avg 13.8 months, 9.9-16.6); the data from this visit were therefore not included in the analysis. At 5.6 years, X-rays and KSS could be obtained in 18 patients. Five patients had had prior orthopedic interventions on the knee: arthroscopy (N=3), femoral osteotomy (N=1) and curettage of tibial tuberculosis (N=1). The proportion of patients in each Charnley category was: (A) 22%, (B) 22% and (C) 56%. Half of the knees operated were right knees (N=14). The tibia component was cemented for all patients while the femoral component was cemented for 6 patients (21.4%) and cementless for 22 patients (78.6%). Patella resurfacing was performed in 12 patients (42.9%). The mean operating time was 96.8 minutes (SD 11.6 min, range 80-120 min). The overall survival rate of the 28 prostheses was 100 % at 5.6 years. In 3 of the 4 patients who did not attend the 5-year visit, the prosthesis was still in place at the last visit completed. One patient was lost to follow-up but had a three-year follow-up with the prosthesis in place, reporting restrictions in the contralateral knee, with a total KSS of 180 points.
Pain Relief and Functional Improvement
The scores obtained on each of the 5 dimensions of the KOOS questionnaire are presented in Fig. (2). The average score for ADL was 77.8 points (SD 16.7; range 35.3-100) (Table 2).
Comparison in the KOOS Subscales Between Patients who Received the e.motion® UC Knee Prosthesis and Patients who Received the LCS Prosthesis (Lygre et al., 2010)
| e.motion® UC Prosthesis (Follow-Up: 5.6 Years) | LCS Prosthesis | Difference Between Prostheses | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Resurfaced (N=12) | Non-Resurfaced (N=16) | Weighted Mean (N=28) | Resurfaced (N=184)1 | Non-Resurfaced (N=180)1 | Weighted Mean (N= 364) | (e.motion® – LCS), Weighted Means2 | |||||||||
| Mean | ± | SE | Mean | ± | SE | Mean | ± | SE | Mean | ± | SE | ||||
| ADL | 77,5 | ± | 18,7 | 78,1 | ± | 15,8 | 77,8 | 70,8 | ± | 1,9 | 71,6 | ± | 2,1 | 71,2 | 6,6 |
| Pain | 83,1 | ± | 22,9 | 84,9 | ± | 13,9 | 84,1 | 76,1 | ± | 1,8 | 75,8 | ± | 2 | 76 | 8,1 |
| Symptoms | 82,1 | ± | 19,9 | 86,6 | ± | 11,9 | 84,7 | 78 | ± | 1,5 | 79,9 | ± | 1,5 | 78,9 | 5,8 |
| Sports | 37,1 | ± | 21,2 | 37,8 | ± | 38,6 | 37,5 | 35,9 | ± | 2,3 | 38,3 | ± | 2,6 | 37,1 | 0,4 |
| QoL | 70,8 | ± | 23 | 73,8 | ± | 19,1 | 72,5 | 59,6 | ± | 2,3 | 62,3 | ± | 2,3 | 60,9 | 11,6 |
SE: standard error; UC: ultra-congruent; LCS: low-contact stress
The Knee injury and Osteoarthritis Outcome Score (KOOS) is a 42-item self‑administered questionnaire that covers 5 dimensions: pain (“Pain”, 9 items), other disease‑specific symptoms (“Symptoms”, 7 items), activities of daily living (“ADL”, 17 items), sport and recreation function (“Sports”, 5 items), and knee-related quality of life (“QoL”, 4 items).
1 Data kindly provided by Dr Lygre (Publication: Lygre SH, Espehaug B, Havelin LI, Vollset SE, Furnes O. Does patella resurfacing really matter? Pain and function in 972 patients after primary total knee arthroplasty. An observational study from the Norwegian Arthroplasty Register. Acta Orthop. 2010; 81 (1): 99-107.)
2 Weighted mean = ((mean resurfaced *184)+(mean non-resurfaced*180))/364.

Knee injury and osteoarthritis outcome score (KOOS) 5.6 years following total knee arthroplasty (TKA) with the e.motion® UC knee prosthesis.
The graph shows the median (horizontal bar in the box), the 25th and 75th percentiles (top and bottom of the box) and the min to max values (whiskers).)
The Knee Society Scores (both functional and clinical) improved significantly between surgery and the 29 months follow-up visits (Table 3, p<0.0001).
e.motion®-Prosthesis Followed Up for 5.6 Years. Summary Data for KSS-Total Score
| Interval | N | Mean | STD | Minimum | Maximum |
|---|---|---|---|---|---|
| FU0: preOP | 28 | 70.18 | 23.30 | 19.00 | 111.00 |
| FU1: 6Months | 25 | 141.60 | 35.50 | 52.00 | 199.00 |
| FU2: 1 Year | 13 | 150.00 | 35.35 | 79.00 | 198.00 |
| FU3: 2-3 Years | 25 | 166.48 | 38.56 | 45.00 | 199.00 |
| FU4: 5-6 Years | 18 | 160.33 | 31.17 | 99.00 | 198.00 |
At 5.6 years, the functional and clinical KSS were 68.1±31.5 and 91.7±7.2 points (N=18).
The Knee Society Scores (both functional and clinical) improved significantly between pre-surgery and the 2-year follow-up visits (Table 3, p<0.0001). At 5.6 years, the functional and clinical KSS were 68.1±31.5 and 92.3±5.8 points (N=18).
To rule out a positive selection of the four patients who could not be examined at 5 to 6 years their maximum available follow-ups between 6 months and 3 years were examined regarding the total KSS. The score values of the patients at these timepoints were 145 (4 months) 192(1 year), 180 (3 years), and 188 (3 years). The corresponding averages at these timepoints were 141.6(4 months), 150.0(1 year), and 166.5 (3 years) (see Table 3). Therefore it can be concluded that the patients that came for follow-up were not a positive selection.
Radiological Findings
At 29 months, only 1 radiolucent line thicker than 1 mm was found (zone 1, tibia, antero-lateral view). Four radiolucent lines with a thickness of 1 mm or less were found: zone 1, femur, lateral view (N=2) and zone 4, femur, lateral view (N=2). At 5.6 years, no radiolucent lines thicker than 1 mm were found in the 18 patients for whom X-rays were available (Fig. 4). Radiolucent lines with a thickness of 1 mm or less were found in 3 patients: 1 patient had 1 line (zone 4, tibia, antero-posterior view), and 2 patients had 2 lines (zones 1 and 7, femur, lateral view). At 29 months, tilting and subluxation of the patella were observed in 2 patients, respectively. At 5.6 years, 1 patient´s patella was misaligned (off by 3 to 12mm at 90°, see Fig. 3). Another patient showed a 10-mm subluxation that healed with no further complications (this patient had a transfer of the anterior tibial tuberosity when she received the e.motion® prosthesis, due to a congenital dislocation of the patella).
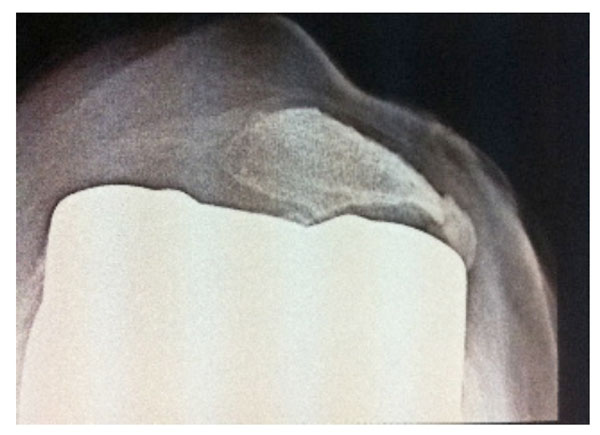
At 5.6 years, 1 patient´s patella was misaligned (off by 3 to 12mm at 90°).
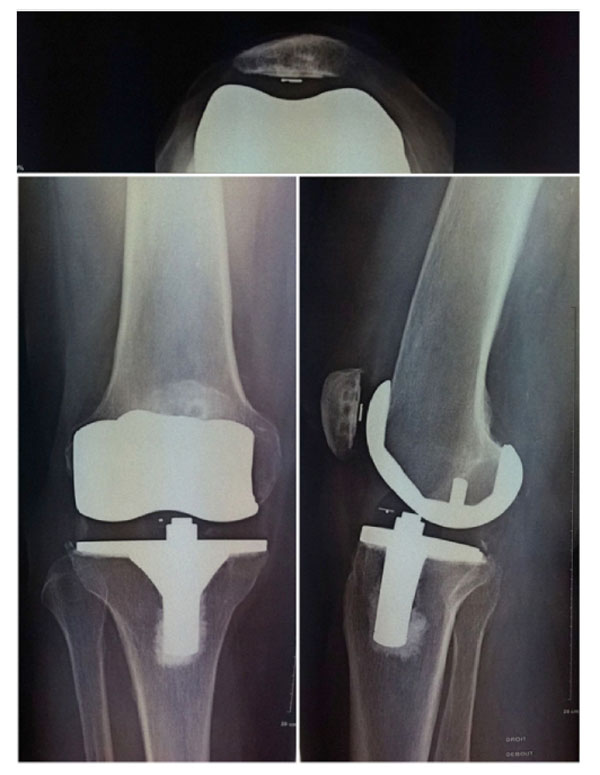
X-rays of the e.motion® UC knee prosthesis 5.6 years after surgery in a 70-year-old man. Top: skyline view (knee angle 90 degrees); left: antero-posterior view (standing); right: lateral view (standing).
Safety
No adverse events were reported during the surgery. Four patients (14%) reported persistent knee pain at the 5-year visit. One of these 4 patients also showed a lack of mobility in the operated knee. Another patient showed early signs of ipsilateral coxarthrosis approximately 6 years after surgery (operated left). There were two serious adverse events, which were not considered related to the surgery procedure or the prosthesis. One patient fell and sustained a fracture of the left femur (1/3 distal) and right tibia/fibula 21 months after surgery. This patient had had a long-term deficit in his foot flexors that had not been investigated and at the 1-year visit, he reported pain in the right external popliteal sciatic nerve, localized near the fibular neck. Another patient sustained a fracture of the left femoral neck approximately 5.7 years after surgery, due to osteoporosis.
DISCUSSION
Out of 32 patients who received the e.motion® UC prosthesis the general functionality and safety could be assessed in 28 patients approximately 5.6 years following TKA index surgery. Functionality in daily life activities, as assessed by the KOOS, was higher with the e.motion® UC prosthesis than with various prostheses reported in 364 Norwegian patients [5]. Functionality and knee pain, as assessed by KSS, has also markedly improved 29 months following the e.motion® implantation. The KSS data at the final visit (N=18) suggest that the improvement was maintained at 5.6 years. The e.motion® UC prosthesis also demonstrated good safety. Five years after surgery, 3 patients showed minor radiolucent lines (<1 mm) on femur and tibia. Three patellar problems were observed and none of the complications were related to the prosthetic design. The general functionality of the e.motion® UC prosthesis was benchmarked against the LCS prosthesis (Table 2) because it has a very similar design concept and is one of the most widely used knee implants. The data on the LCS prosthesis was obtained in a large cohort (N=364) of Norwegian patients who were surveyed after an average of 6.5 years following surgery and had similar characteristics than the e.motion® patients [5]. The LCS patients were slightly younger at surgery (69.0 years, vs 72.4 years for the e.motion® patients) and at the follow-up visit, during which the KOOS questionnaire was distributed (75.5 vs 77.8 years). In the present study, 56% of the patients had comorbidities affecting locomotion (Charnley category C) at the time of surgery. The proportion was higher in the Norwegian study (65%); however, the data were collected at follow-up (i.e. in older patients). The proportions of female patients (85.7% vs 72.0%) and resurfaced patellae (42.9% vs 50.5%) were also similar between the two studies. The KOOS score for ADL obtained with the e.motion® UC prosthesis was 6.6 point higher than the score obtained with the LCS prosthesis [5]. Such a difference may not be considered clinically significant: it is lower than 8-10 points, which was suggested as the minimal clinically significant change for KOOS [11]. Also the number of e.motion UC-patients benchmarked against LCS was too low to finally conclude on a clinical difference between the systems. The differences measured in ADL scores between the e.motion® and the LCS prostheses could be explained by differences in the prosthetic design but also the patients´ pre-operative characteristics. For example, patients with lower preoperative scores for knee function tend to have lower postoperative scores [18]. Unfortunately, the influence of this factor could not be assessed because the KOOS was only evaluated at follow-up in both studies. The scores for the other 4 dimensions of the KOOS were also higher in the e.motion® patients than the LCS patients: the difference ranged from +0.4 (Sports) to +11.6 points (QoL). The e.motion® UC prosthesis seems to perform slightly better than prostheses such as the AGC, Genesis I and Nexgen (except for the subscale “Sports” in resurfaced knees operated with Nexgen) [5]. There was a marked improvement in both the functional and clinical KSS over the 29 months following surgery with the e.motion® UC prosthesis. Data at 5.6 years (in 18 patients) suggest that the improvement in KSS was maintained over time. These findings are consistent with the decreased knee pain and improved functionality following the e.motion® implantation, as indicated by the KOOS. The prosthesis also showed good stability and alignment, as assessed by the surgeon for the clinical KSS. The most common cause of revision of mobile-bearing TKA is bearing-related issues, including chronic instability, bearing subluxation, bearing dislocation, or bearing wear [19]. The e.motion® UC prosthesis was found to have good stability and no loosening at 5.6 years. Except for 2 cases of patella subluxation (1 being in a patient with congenital dislocation of the knee and patella), and 1 case of patellar misalignment, there were no other subluxations or dislocations of the bearings. The good results regarding stability of the knees could also be due to an optimized alignment and soft tissue management provided by the kinematic navigation system used in all patients of this study.
Radiolucent lines, which tend to be more frequent in uncemented TKA [20], were rare. In this pilot study, the tibial plateau was cemented in all patients, which most likely contributed to the good implant seat. None of the patients who completed the 5-year follow-up had their prosthesis revised and none of the complications were related to the prosthesis design. Bearing issues have been reported with the LCS prosthesis, with a prevalence of lower than 2% [21]. Several factors may have contributed to the relatively low rate of complications in this pilot study: the surgical technique with attention to soft tissue balancing [3], the innovative design of the prosthesis, and the computer-assisted navigation system [22]. Biomechanical investigations conducted in vitro showed that the gravimetric wear rate for the e.motion® UC prosthesis was 2.3 mg/106 cycles [4], which is relatively low compared with the wear rates of mobile-bearing designs with good long-term clinical outcome (6.6 to 16 mg/106 cycles) [1, 23, 24]. This is a promising result for the e.motion® UC prosthesis, considering the long-term survivorship of an implant is related to the wear of the bearing surface [25].
CONCLUSION
This pilot study is the first to report mid-term outcomes of the e.motion® UC prosthesis. In a small sample, the implant performed comparably to the LCS design (as reported by Lygre et al. [5]) regarding clinical and functional outcomes. The 5-year results for this new prosthesis need to be confirmed in the longer term, with larger groups of patients.
CONFLICT OF INTEREST
The author was paid by Aesculap AG for organizing the 5-year follow-up experiments. There are no other conflicts of interest.
ACKNOWLEDGEMENTS
We would like to thank Gaële Ducher of Scinopsis for writing the article. This study was funded by B. Braun Aesculap, Tuttlingen.


