All published articles of this journal are available on ScienceDirect.
Patellofemoral Arthroplasty: A Systematic Review of the Literature
Abstract
Identification and management of patients with isolated patellofemoral osteoarthritis are challenging. Many of these patients present at a young age and it is important to distinguish degenerative change in the patellofemoral articulation from the other various causes of anterior knee pain. Once the diagnosis of isolated patellofemoral arthrosis has been made non-operative and conservative surgical techniques should be exhausted fully before prosthetic arthroplasty is considered. This review focuses on the use of arthroplasty for isolated patellofemoral arthrosis, in particular comparing the use of total knee against selective patellofemoral joint replacements.
INTRODUCTION
Isolated patellofemoral osteoarthritis (PFOA) is a relatively common condition occurring in up to 24% of patients over fifty years of age, with a higher frequency in females [1-3]. The aetiology of PFOA is multifactorial, and as with other forms of arthritis, trauma, obesity and inflammatory processes have been implicated. Furthermore, owing to the unique morphology of the patellofemoral joint, instability, abnormal patellar tilt and anatomical dysplasia are thought to play a major role in the development of degenerative changes [4].
As with other arthritic conditions the preliminary management of most patients with PFOA consists of primarily non-operative approaches. However although interventions such as activity and lifestyle modifications and physical therapy have been shown to decrease the symptoms of PFOA they ultimately do not alter the course of the disease for many individuals [5-7].
There are numerous operative interventions which seek to address PFOA without resorting to arthroplasty.
Soft-tissue realignment surgery is based on the principle that the patella is eccentrically loaded (usually laterally) in many patients with PFOA and this is the primary cause of degeneration and pain. Offloading this force can slow the progression of the disease and alleviate symptoms [8]. Anteromedial transfer of the tibial tuberosity and lateral retinacular release are two such techniques which have been shown to be beneficial in select patient groups, either alone or in combination [6-8].
Autologous chondrocyte implantation is advocated in younger patients who often have chondral defects rather than diffuse cartilage loss and in whom maltracking of the patella has been ruled out or corrected. Two studies with long term follow-up have shown favourable results with regards to functional outcome and delay of arthroplasty [9, 10].
There are currently no studies which have investigated the role of arthroscopy in isolated PFOA but arthroscopy has been shown to be ineffective in generalised arthritis of the knee when compared to placebo or optimized medical and physical therapy [11, 12]. Historically patellectomy has been used for patients with anterior knee pain and PFOA with reasonable results reported at long term follow-up [13]. However due to the crucial role of the patella in aiding quadriceps function this is not a procedure in widespread use today.
For those patients who are not suitable for any of the above measures or in whom they have been unsuccessful, arthroplasty should be considered. Logic would dictate that in the face of isolated patellofemoral arthrosis, replacement should be reserved for this compartment only. There is, however, a strong body of evidence which advocates the use of Total knee Arthroplasty (TKA) in isolated PFOA, with the proponents citing more predictable and favourable outcomes when compared with Patellofemoral Arthroplasty (PFA). This study aims to investigate the evidence available for both forms of arthroplasty for the treatment of PFOA.
METHODS AND STUDY IDENTIFICATION
Independent computerised searches were carried out on the 4th of January 2012 by two of the authors (PT and SP) on the following databases up to January 2012;
- MEDLINE (Pubmed)
- The Cochrane Library: CENTRAL (Central Register of Controlled Trials)
Terms used with Boolean operators were: (patella-femoral OR patell* OR femoropatell* OR femoro-patell*) AND (arthroplasty OR replacement OR resurfacing).
Studies excluded were those that were not in the English language, were not fully published articles or were review articles. Further grounds for exclusion was at the discretion of the reviewers and comprised but was not limited to factors such as poor or incompletely described methodology, low patient population (<20) or studies reporting results from treatment of conditions other than osteoarthritis as the primary indication for surgery.
RESULTS
The QUOROM [14] flow diagram for included studies is shown below (Fig. 1). The search identified 14 eligible studies reporting results from PFA [15-28] and 3 studies reporting results from TKA [29-31] in the treatment of isolated PFOA. There are no published randomised controlled trials comparing PFA to TKA for isolated patellofemoral arthritis, although one has been proposed [36]. There is one study [37] which compares PFA to TKA however this was a retrospective study with no randomisation.
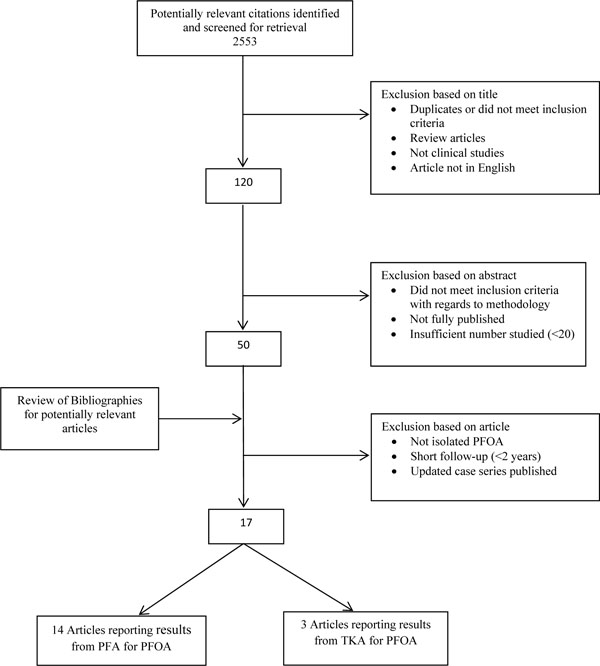
QUORUM flow diagram for included studies.
STUDIES REPORTING RESULTS FROM PATELLOFEMORAL ARTHROPLASTY
The prosthesis with the greatest reported numbers in the studies reviewed was the Avon which is produced by Stryker (New Jersey, USA). There was only one study which reported results from a custom made prosthesis [23].
Summary of All Included Papers
| Study | PFA/ TKA | Prosthesis | Knees (Patients)* | Age | M:F | Follow Up (Years) | Outcomes and Results | Complications and Revision |
|---|---|---|---|---|---|---|---|---|
| Ackroyd et al. [15] | PFA | Avon | 109 (85) | 68 (46-86) | 10:75 | 5.2 (5-8) | 5-year survival (revision as endpoint): 95.8% (95% CI 91.8% to 99.8%). At five years Median Bristol pain score improved from 15/40 pts (IQR 5-20) to 35 (IQR 20-40)
Median MKS from 10 (IQR 6-15) to 25 (IQR 20-29) Median OKS 18 (IQR 13-24) to 39 (24-45) Successful results (Bristol pain score of at least 20 at five years) 80% (66) of knees |
Early complications in 6 pts; delayed wound healing, post op haemarthrosis, synovial inflammation
Patellar instability requiring re-alignment in 1pt 25pts (28%) had progression on OA requiring revision in 4 knees (4.2%) No cases of deep infection, wear, loosening or fracture |
| Kooijman et al. [16] | PFA | Richards II | 56 (51) | 50 (30-77) | 27:24 | 17 (15-21) | Mean survival of 17.8 years (95% CI 16.3 to 19.4)
Mean CKSS at 15 years inc failures - 167/200 Patient subjective judgement; 86% report Good/Excellent at mean f/u of 17 years |
Early complications in 4 pts - DVT
Early MUA, arthroscopy or debridement in 18% Revision to TKR in 10 knees due to progression of OA (17.8%) at mean 15.6 years Loosening rate of 2% requiring revision |
| Tauro et al. [17] | PFA | Lubinus | 62 (48) | 66 (50-87) | 10:49 | 7.5 (1-20) | Cumulative survival at 65% at 8 years (CI 49-77)
BKS improved from 55 (29-86) to 81 (42-100) in unrevised knees Satisfactory outcome (BKS>80) in 28 of 62 knees (45%) Patient report of pain: 53% no pain, 26% mild pain, 21% moderate pain |
Revision rate of 28% (21 knees)
15 had patellar maltracking - 5 revised to TKR, and 10 to Avon PFA) Progression of arthritis in 7 knees (6.5%) 2 patellar fractures No loosening. Infection rate not stated. Authors discontinued use of prosthesis following results |
| Argenson et al. [18] | PFA | Autocentric | 66 (66) | 57 (21-82) | 26:31 | 16.2 (12-20) | Cumulative survival 58% at 16 years (including death from unrelated causes)
Knee society pain score improvement from 53.1 (43-70) to 78.5 (60-100) Knee society function score improvement from 40.6 (10-80) to 81.2 (40-100) |
Revision for progression of OA in 14 of 57 to TKA at an average of 7.3 years (1-12)
Revision for loosening in 11 of 57 |
| Mont et al. [19] | PFA | Avon | 43 (37) | 49 (27-67) | 29:8 | 7 (4-8) | Kaplan-Meier survival 95% at 5 years and 82% at 7 years
KSOS improvement from 64 (57-68) to 87 (50-100) KSFS improvement from 48 (45-50) to 82 (20-100) |
Revision for progression of OA in 2 patients at 10.5 months to TKA.
Revision for all other causes in 3 patients (all to TKA) |
| van Jonbergen et al. [20] | PFA | Richards II | 181 (157) | 52 (±14) | 59:98 | 13.3 (2-30.6) | Cumulative survival (clinical failure as endpoint) 84% at 10 years (95% CI 78%-90%) and 69% at 20 years (CI 59%-79%)
Primary diagnosis, sex, or age at time of surgery did not significantly affect survivorship. Rate of revision in obese (BMI>30 Kg/m2) higher (P=0.0.2) |
95 further surgical procedures performed on 69 knees (38%) during the follow up period; further PFA for loosening, malposition or wear in 18 (10%), Removal of prosthesis due to infection (1) or malposition (2), conversion to TKA in 23 (13%) for progression of OA and other procedures including MUA, arthroscopy or arthrotomy in 51 (28%) |
| Cartier et al. [21] | PFA | Richards II+III | 79 (70) | 60 (36-81) | 9:41 | 10 (6-16) | Cumulative survivorship 75% at 11 years
KSOS; 77% excellent, 14% fair & 9% failures. KSFS; 72% excellent, 19% fair, and 9% failures. Patients reported 47 of 59 knees as pain free and 12 knees as causing moderate or worse pain Stair climbing/descending normal in 91% |
Further surgery required in 13 knees (5 minor)
Revision for progression of OA to TKR: 8 knees Polyethylene wear: Substantial - 1, Moderate - 5 Patellar snapping in 2% |
| Odumenya et al. [22] | PFA | Avon | 50 (32) | 66 (42-88) | 9:23 | 5.3 (2-10) | Cumulative survival 100% at 5 years.
Median OKS 30.5 (IQR 22.25-44.25) |
2 Revisions in the same patient at 6-8 years due to pain and progression of OA. 11 of 50 knees showed progression of TFOA on follow up radiographs.
No loosening, infection or periprosthetic fracture |
| Sisto & Sarin [23] | PFA | Custom (CT aided design) | 25 (22) | 45 (23-51) | 6:16 | 6 (2.6-10) | Cumulative survival 100%
18 Excellent (Knee society score>90) 7 Good (Knee society 80-90) KSOS improvement from 52 (30-60) to 91 (82-96) KSFS improvement from 49 (24-76) to 89 (81 to 94) mean range of active flexion improved from 110° (85°-120°) preoperatively to 122° (110°-130°) at the time of final follow-up. |
No subsequent operations at time of latest follow up
No reports of pain during walking. No reports weakness, instability or night pain 3 Patients had anterior knee pain when ascending/descending stairs which al resolved within 6 months. No progressive radiolucent lines or other lucencies >2mm found around the implants |
| Sarda et al. [24] | PFA | Avon | 44 (40) | 62 (43-84) | 9:31 | 4.5 (3-8) | MKS improvement from 10 (5-21) to 25 (11-30)
KSFS improvement from 57 (23-95) to 85 (27-100) Patient questionnaire; 85% Excellent/Good, 12% Fair, 5% Poor |
2 revisions to TKA; 1) Progression of OA at 18months
2) Persistent pain/clicking at 3 years
No cases of deep infection |
| Mohammed et al. [25] | PFA | Lubinus, FPV and Avon | 101/91
46 Lubinus 30 FPV 25 Avon |
57 | 1:3** | 4 (0.5-8) | 73 % did very well (Authors’ own measure/statement taken to mean that these patients did not require further surgery and had no residual stiffness) | 28 patients requiring 35 operations in total (18 arthroscopic debridement, 8 lateral retinacular release, 3 tibial tuberosity transfer, 2 MUA for stiffness and 4 revision to TKA. 1 deep infection.
No mechanical failure or radiological loosening. 1 deep |
| Wagenberg et al. [26] | PFA | Autocentric | 24 (20) | 63 (38-81) | 9:15 | 4.8 (2-11) | Cumulative survival 75% at mean of 4.8 years with revision as the end point. | Additional interventions in 21 of 24 knees.
7 of 24 revised to TKA for progression of TFOA Authors abandoned use of this prosthesis. |
| Leadbetter et al. [27] | PFA | Avon | 30 (25) | 48 (25-73) | 2:23 | 2 (0.5-6) | Procedure considered successful in 25 of 30 knees (83%) by authors own criteria. The subjective outcomes for twenty-five knees were rated by the patient as good to excellent. | 17 knees reported to be occasionally mildly painful. Six knees painful with stairs only, 2 knees painful with stairs and walking.
1 failure of technique resulting in femoral notching and 4 cases of stiffness requiring MUA. 2 revisions to TKA |
| Starks et al. [28] | PFA | Avon | 37 (29) | 66 (30-82) | 8:21 | 2 (at review) | Median OKS 39 (IQR 32-44)
Median KSOS 95 (IQR 90-100) Median MKS 28 (IQR 21-30) All but on patient satisfied at the year review |
2 patients underwent further surgery - 1 patellar resurfacing and 1 patellar fracture |
| Meding et al. [29] | TKA | AGC | 33 (27) | 52 | 6:21 | 6.2 (2-12) | KSFS improvement from 55 (35-80) to 83 (45-100)
KSPS improvement from 5 (0-20) to 44 (20-50) When compared to a matched group of TCOA no significant difference in any component of KSS or range of motion. |
No revisions, re-operations, manipulations or clinical loosening. One case of 1mm radiolucency.
No clinical thrombosis or infection. |
| Laskin et al. [30] | TKA | Genesis | 48 (48) | 67 (54-85) | N/A | 7.4 (3-10) | PFOA group (A) to matched group of TCOA (B)
Patients in the PFOA group had significantly better outcomes; KSPS - 47 (A) vs 40 (B), KSS - 96 (A) vs 88 (B), ROM - 122° (A) vs 117° (B), Bipedal stair climbing - 82% (A) vs 72% (B), Rising independently - 74% (A) vs 68% (B) (All p<0.05) |
3 patients in Group A and 4 patients in Group B complained of anterior knee pain when climbing or when standing from a sitting position. Of these 7 only 1 had patellar tilt on merchant view
No other complications declared by authors. |
| Mont [31] | TKA | PCA, Duracon & IB-2 | 30 (27) | 73 (59-88) | 9:18 | 7 (4-11) | 28 Excellent (KSS>90), 1 Good (KSS 80-89) and 1 poor (KSS<70).
KSOS improvement from 50 (20-64) to 93 (67-100) KSFS improvement from 49 (20-80) to 86 (60-100) |
One patient with poor result due to patellar tendon rupture following fall.
5 reported pain during normal walking No reported clinical loosening, infection or thrombosis No reported revision or further surgical procedures |
** Number represents value used for survival and/or statistical analysis, **Expressed as approximate ratio (exact numbers not disclosed by authors), TCOA – Tri-compartmental Osteoarthritis, TFOA – Tibiofemoral Osteoarthritis.
Number of Prosthesis by Type in Studies Reviewed
| Prosthesis | Manufacturer | Number |
|---|---|---|
| Avon | Stryker, New Jersey, USA | 338 |
| Richards | Smith & Nephew, UK | 316 |
| Lubinus | Waldemar Link, Hamburg, Germany | 98 |
| Autocentric | Depuy, Indiana, USA | 90 |
| FPV | Wright Medical, UK | 30 |
All of the included studies specified isolated PFOA as the primary diagnosis and the indication to embark on surgery. There were several studies that were identified in the literature which had good numbers and sound methodology however the primary pre-operative diagnosis was not restricted to PFOA [38,39]. One particular study by Starks [28] and colleagues reported results of the Avon PFA and give an excellent independent verdict of the prosthesis, however, within their population they included one patient who had had a failed autologous chondrocyte implantation of the patella. As the pathology of this condition is limited to the patellofemoral joint and as it was an isolated case, its impact on the overall study was deemed to be small and hence it was included in this review.
Other studies which cited PFOA as the primary diagnosis and had adequate methodology were not included as their series were smaller in comparison to others [40-42]. We chose a minimum cut-off study population of 20 prostheses/knees (after loss to follow up) for this review.
Seven studies included a pre-operative assessment [15, 17-20, 23, 24] whereas the other 7 studies included only a postoperative assessment of the patient. There were two studies [15, 18] which had published preliminary results from their series [43, 44] previously in the literature. The earlier studies were therefore not included in this review.
Two studies were identified that reported on custom prostheses for PFA [23,40]. The studies by Merchant [40,41] were not included because of low patient numbers.
STUDIES REPORTING RESULTS FROM TOTAL KNEE ARTHROPLASTY
Three studies were identified from the search. Two of these studies compared a cohort of patients with isolated PFOA with a matched group [29, 30].
Meding et al. [29] reported on 27 patients who had undergone 33 TKAs and were all younger than 60 years of age, and compared this group with another identical in number (27 patients - 33 TKAs) with primary tibiofemoral OA (TFOA). The comparison group was also matched according to surgeon, gender, bilaterality, and age. Body mass index was matched within 2kg/m2. Similarly Laskin et al. [30] compared their group of 44 knees with PFOA to another group of 46 knees with tricompartmental OA (TCOA) and matched for gender and age but not for any other criteria. Of note their TCOA group had significantly higher body mass.
The third study by Mont et al. [31] had no comparison group but reported pre-operative assessment and outcomes from their use of three different prostheses in their group of 30 knees in 27 patients. The Knee Society objective and functional scores [32] were used to report on results.
The three included studies on TKA for isolated PFOA have an average of 7 years follow up and feature a combined total of 111 prostheses [29-31]. Functional and objective outcome scores are comparable to TKA and amongst the best when compared to PFA. Additionally there have been no reported cases of revision of any of the prostheses. This had led to authors to conclude that this may be the best course of action for patients with isolated PFOA.
DISCUSSION
Isolated patellofemoral arthrosis is a disabling condition which occurs commonly in younger, more active patients who often have otherwise normal articular cartilage in the tibiofemoral compartments of their knee. A logical approach to surgical intervention would therefore be one that seeks to address only the abnormality whilst preserving as much of the normal anatomy and native kinematics of the patients knee. This is the idea behind patellofemoral arthroplasty, however, its implementation has not always been successful. The first reported series of replacement of the patellofemoral joint was by McKeever in 1955 [45] who recognised that there was room for improvement in the management of patients with advanced but isolated PFOA. These patients commonly underwent patellectomy, which McKeever viewed as an operation that was cumbersome and one that provided altogether unsatisfactory outcomes for the patient [45]. He proposed his own design of a Vitallium shell to replace the arthritic patellar surface and reported reasonable results albeit with short follow up. Although there were several variations and improvements of the design in the following years, nevertheless when two surfaces of different hardness articulate, the softer surface will undergo a much higher rate of attrition. Therefore this prosthesis was abandoned due to concerns regarding trochlear wear. The first reports of total patellofemoral replacements did not emerge until 1979 following the introduction of the Lubinus glide [46] and Richards [39] prostheses.
Following Lubinus’ own early report on the prosthesis [46], the first study to declare medium to long-term results of the Lubinus prosthesis was published in 2001 by Tauro and colleagues [17]. They reported a cumulative survival of 50% with revision or moderate pain as the end point. The authors cited that the asymmetrical trochlear design of the Lubinus and with the necessity to fit the trochlear component anatomically meant that no adjustment can be made to improve tracking, congruence and contact. They stipulated that it was perhaps this feature which made the patella susceptible to tilt, malalignment, impingement and wear, ultimately resulting in failure. The authors found these results unacceptable and subsequently abandoned use of the prosthesis, changing to the Avon.
Results from the Autocentric prosthesis, while slightly better than that of the Lubinus, are also disappointing [26, 44]. Van Wagenberg [26] recently reported a failure rate of 25% at 4.8 years with many additional surgical interventions required and generally poor patient satisfaction. They did however find that certain factors such as high BMI and patella alta or baja were predictive of progression of tibiofemoral arthritis and subsequent revision. The study by Argenson [44] has the longest reported follow up for this series and they also cite survival of 58% at 16 years with revision for progression of osteoarthritis in 14 of 57 knees at an average of 7.3 years, and revision for loosening in 11 of 57 knees.
The Richards prosthesis, however, has been reported on more extensively in the literature with more favourable results [16, 20, 21]. Blazina [39] was the first to publish results on this prosthesis with a mixture of Richards I and II (the Richards I was discontinued during his use in the reported series). The Richards II differed from the Richard I in that the femoral component had a tongue-like extension of the groove towards the femoral notch. The Richards III is a further modification by Cartier [21] and colleagues which incorporates spurs rather than a peg for bone fixation which is a more conservative approach reducing the amount of cement required. This design was however only reserved for revision procedures. Contrary to the Lubinus which has fallen out of favour [17] (although mostly in the last decade), the Richards II is still advocated by certain groups. The recent study by van Jonbergen [20] reporting on 185 prostheses (the largest reported series on the Richards prosthesis) cites reasonable long-term results with the Richards II with 84% survivorship at 10 years and 69% at 20 years. Similarly Cartier [21] reported 75% survivorship at 11 years in their series of 79 Richards II and III. These results, while encouraging and far superior to those of other designs such as the Lubinus, are nevertheless inferior to outcomes following TKA. With this in mind, the Avon PFA was designed by surgeons of the Bristol Knee Group to emulate the successful reproduction of patellofemoral joint mechanics afforded by TKA designs, and in this particular case the Stryker Kinemax Plus TKA [8].
Unsurprisingly the largest reported series of the Avon PFA originates from the Avon Orthopaedic Centre in Bristol. Ackroyd et al. published early results in 2005 [43] reporting the insertion of 306 Avon PFAs at their centre with 2 year follow up available in 124 and 5 year follow up in 33. The more recent study [15] from the same centre and from the same cohort of patients reports on 109 Avon PFAs with a minimum follow up of 5 years. They cite a 5-year survival of 95.8% (with revision as the end point) and good improvements in functional outcome scores in this group. However when the thresholds for moderate or severe pain were included in the analysis the survivorship was 88% at 5-years. These results are nevertheless encouraging and have been emulated by independent centres [19, 22, 24, 27, 28]. Mont et al. [19] recently reported on their series at a mean follow-up of 7 years and cited a 95% survival at 5 years but falling to 88% at 7 years.
The most common reason cited for failure requiring revision in all of the above studies is the progression of TFOA. The rates vary between studies and prosthesis, but it is unclear whether this happens at an accelerated rate because of altered knee kinematics following PFA, or that the increased level of activity afforded by the improved level of function causes natural progression of disease. Nicol et al. [47] investigated possible reasons for this by undertaking a radiological study of knees which had displayed progression of TFOA following the Avon PFA. They found that 40% of those knees with TFOA progression had surface damage of the articular cartilage of the femoral condyles documented at the time of operation. In addition they found that progression of TFOA was much less likely in cases where the primary pathology of PFOA was trochlear dysplasia or patella-femoral malalignment rather than primary. This was a finding echoed by others previously [21,44] who reported on series where their selection criteria primarily included patients with trochlear dysplasia or malalignment rather than primary PFOA.
With the consideration that PFA often fails due to a poor implant design or geometry which does not accurately emulate the patient’s own anatomy, Sisto and Sarin of the Los Angeles Orthopaedic Institute presented their results of custom-made prostheses for PFA [23]. A pre-operative computer tomography scan is carried out which maps the patients femur and using specialised software the prosthesis is designed to mimic normal kinematics by recreating the alignment and depth of the trochlear groove and repositioning the patella anteriorly to improve quadriceps function. Additionally the custom fit of the prosthesis means there should be no bone resection from the femur unless to debride osteophytic areas at the margins of the implant footprint. Sisto and Sarin’s reported results are excellent with no further procedures, no revisions and improvements in functional scores equal to TKA being achieved [23]. However, by the author’s own admission, costs are greatly increased with this prosthesis. On average the total cost for the implant including the cost of the CT scan will be 50% higher, although this is still less than that of “high performance” TKA designs. Nevertheless this is only the only centre which has produced results from this method and hence no firm conclusions should be drawn until an independent centre can reproduce the same results.
CONCLUSIONS
Patellofemoral arthroplasty is certainly a technically demanding procedure with narrow indications.
Nevertheless a patellofemoral arthroplasty has the advantage of being a less invasive operation, with quicker post-operative recovery and preservation of bone stock, with the option to convert to TKA at a later time. Evidence presented from the studies above points to certain poor prognostic factors which should be considered when selecting patients for PFA (Table 3). With newer, more anatomical prosthetic designs and with strict selection criteria, PFA can provide highly satisfactory outcomes.
Patient Characteristics Relating to Poor Outcome in PFA
| Patient Characteristics Relating to Poor Outcome in PFA |
|---|
|
|
| Evidence of tibiofemoral osteoarthritis prior to surgery |
| BMI>30 Kg/m2 |
| Prior meniscectomy |
| Patella alta or baja |
| Ligamentous instability |
ACKNOWLEDGEMENT
None declared.
CONFLICT OF INTEREST
None of the authors have a conflict of interest to declare in relation to the production of this manuscript.


