All published articles of this journal are available on ScienceDirect.
Ceramic Femoral Components in Total Knee Arthroplasty - Two Year Follow-Up Results of an International Prospective Multi-Centre Study
Abstract
Background:
Total knee arthroplasty can be considered as a reliable surgical procedure with a good long-term clinical result. However, implant failure due to particle induced aseptic loosening as well as the aspect of hypersensitivity to metal ions still remains an emerging issue.
Methods:
The purpose of this prospective international multi-centre study was to evaluate the clinical and radiological outcomes and the reliability of the unconstrained Multigen Plus Total Knee System with a new BIOLOX® delta ceramic femoral component. Cemented total knee arthroplasty was performed on 108 patients (110 knees) at seven hospitals in three countries. Clinical and radiological evaluations were performed preoperatively, and after 3, 12 and 24 months postoperatively using the HSS-, WOMAC-, SF-36-score and standardised X-rays.
Results:
The mean preoperative HSS-Score amounted to 55.5 ± 11.5 points and improved significantly in all postoperative evaluations (85.7 ± 11.7 points at 24 months). Furthermore, improvements in WOMAC- and SF-36-score were evaluated as significant at all points of evaluation. Radiolucent lines around the femoral ceramic component at 24 months were found in four cases. Progression of radiolucent lines was not seen and no implant loosening was observed. During the 24 month follow-up eight patients underwent subsequent surgery due to reasons unrelated to the implant material.
Conclusions:
The observed clinical and radiological results are encouraging for a long-term survival of the ceramic femoral component. Therefore, ceramic implants could be a promising solution not only for patients with allergies against metallic implant materials, but also for the osteoarthritic knee joint. Long-term follow-up is necessary to draw conclusions regarding the superiority of the ceramic knee implants concerning in vivo wear and long-term survivorship.
INTRODUCTION
Total knee arthroplasty (TKA) is one of the most successful principles in orthopaedic surgery [1]. Nevertheless, particle-induced aseptic loosening is, along with malpositioning, a major reason for implant failure especially in younger active patients. The ‘Swedish Register’ shows a cumulative revision rate of 6.5% for patients under 65 years old and 2.5% for patients over 65 years after 8.5 years of follow-up [2]. Thus the demand for a maximum clinical outcome led to improvements in implant fixation, coupling wear and specific designs in order to obtain longer survival rates and an increased range of motion [3]. Furthermore, allergies to implant materials, e.g. chromium, cobalt and nickel, have been found to cause implant failure. Skin reactions to metal ions are described as being up to 20% [4], but there are no valid clinical data on the incidence of implant allergies so far. Ceramics therefore may be a solution for patients with allergies to implant materials and may have an improved resistance to wear, followed by reduced aseptic loosening rates [5]. Since the biologic effect of wear particles depends on the material and volume of wear particles, materials with less wear are of scientific interest [3]. Meanwhile, the worldwide use of ceramics in total hip arthroplasty (THA) is justified because of its high chemical and mechanical stability, its extreme resistance to wear and corrosion, due to the lack of an electrochemical reaction and excellent tribology [6]. Nevertheless, there is still a high brittleness in alumina ceramics, i.e. there is less plastic deformation in contrast to ductile metallic or polymer materials, and low tensile strength. Therefore, stress concentration, e.g. on sharp edges, must be avoided during implantation and the implant design must consider weak spots [7, 8].
At the knee, the first biocompatible ceramic product was implanted as a unicondylar tibial surface replacement by Langer in 1972 and resulted in limited wear between the ceramic and cartilage [9]. The first alumina ceramic (Al2O3) total knee prosthesis was realised by the Kyocera Corp. (Kyoto, Japan) and implanted by Oonishi in the early 1980s [10].
In THA, articulating components are used with optimum contact contributions, resulting in limited local stresses, even if joint loads are high. In contrast, TKA requires components (especially the femoral component) with shapes and contact conditions that necessarily result in high stresses near the corners of femoral resections (tension stress) and at the points of contact with the polyethylene (shear stress). In a finite-element-analysis (FEA) 3-D models of the ceramic femoral component surrounding the femoral bone stock and the connecting bone cement revealed critical stresses, when considering the femoral bone stock morphology [11]. Stresses close to the fatigue limit of 1150 MPa provided by BIOLOX® delta ceramic could be found in the intersections of resection surfaces and at the sharp change of sections at the distal part of component [12].
By using the BIOLOX® delta ceramic (CeramTec, Plochingen, Germany), it was possible to develop a femoral component with a tensile strength that meets the demands for application in TKA. BIOLOX® delta ceramic is a composite matrix material containing 82% vol. alumina (Al2O3) and 17% vol. zirconia (ZrO2) providing good mechanical characteristics in terms of strength and resistance [13]. Furthermore, the low friction coefficient of the novel BIOLOX® delta ceramic causes a change in load.
The purpose of this international prospective multi-centre study was to evaluate the clinical and radiological two year follow-up of the total knee prosthesis with a BIOLOX® delta ceramic femoral component.
MATERIALS AND METHODS
Lima Corporate (Villanova di San Daniele, Udine, Italy) in collaboration with CeramTec provided BIOLOX® delta ceramic femoral components with a design identical to those made of a cobalt-chromium alloy for the Multigen Plus Total Knee Replacement System, which is available and in use since 1997 (Fig. 1). Therefore, the surgeon was able to use the well-known instruments as well as retain the intraoperative possibility of choosing the most appropriate implant material for the patient. The Multigen Plus Ceramic Knee is a non-constrained surface replacement consisting of a symmetric, cruciate-retaining (CR), cemented BIOLOX® delta ceramic femoral and metal (TiAl6V4) tibial components. The fixed-bearing standard ultra-high molecular weight polyethylene liner (UHMWPE) is available in different thicknesses (10 mm, 12 mm, 14 mm, 17 mm and 20 mm).
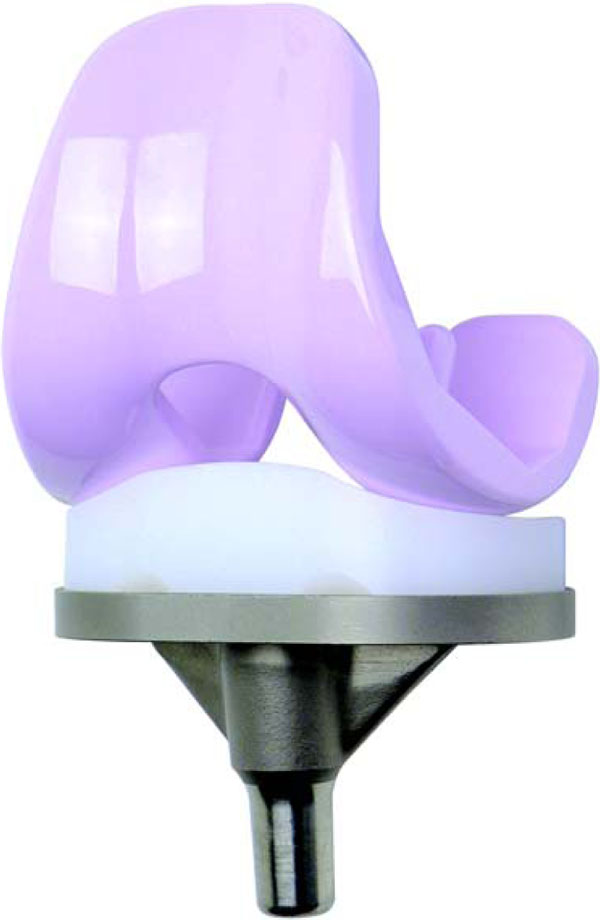
Ceramic Multigen Plus Knee with BIOLOX® delta ceramic femoral component.
Enrolment of the Study Group
A total of 108 patients were enrolled in the study at seven centres (three in Germany, three in Italy and one in Spain). Two patients underwent bilateral TKAs in a period greater than one year. Two patients included in the study underwent bilateral TKAs outside of the enrolment time frame. The study group included 81 (73.6%) TKAs in female and 29 (26.4%) TKAs in male patients. Surgery was performed on 48 (43.6%) left and 62 (56.4%) right knees. The average height and weight of the patients were 165.9 ± 7.7 (150–185) cm and 79.0 ± 11.7 (52–103) kg respectively. BMI and age was 28.7 ± 3.5 (19.1–33.6) and 67.7 ± 6.0 (48–75) respectively.
The study was performed as a prospective non-comparative study for the clinical and radiological evaluation of the BIOLOX® delta ceramic femoral component and was classified as evidence based medicine (EBM) level 4. Inclusion criteria were the indication for primary TKA due to primary osteoarthritis or rheumatoid arthritis. Severe instability or deformity without the possibility for a stable surface replacement was determined as contraindication. Further contraindications for study enrolment were an age of more than 75 years old, BMI > 33 kg/m2, any kind of infection, severe osteoporosis, patient history of tumours, as well as post-traumatic osteoarthritis and contra lateral TKA or joint replacement of the operated limb within one year. Haemophilic patients, patients with neurosensory or neuromotor deficits, which affects product evaluation or rehabilitation of the patient and patients with chronic and progressive severe diseases or known incompatibility or allergy to the used products were additionally excluded from the study. This study was ethics committee approved and all patients gave informed written consent.
Intra- and Perioperative Management
All patients underwent a standard surgical procedure by one or a maximum of two experienced orthopaedic surgeons at each centre, using the Payr approach. The learning curve was reduced by sufficient experience with the identical metallic femoral component of the Multigen Plus Knee System. Implant size and the angle of the femur were determined preoperatively on standard anterior-posterior, lateral, whole leg (anterior-posterior) and Merchant view X-rays. Cementation was achieved with high-viscosity bone cement. Before reconstruction of the quadriceps pulley, a shaping and denervation of the patella and an optimal soft tissue balancing was obligatory in all cases. Prevention of deep vein thrombosis and pulmonary embolism was accomplished by a daily subcutaneous application of a low molecular weight heparin and anti-thrombotic stockings during the hospital and rehabilitation stay. All patients underwent full weight-bearing with two crutches beginning on the second postoperative day after drain removal.
Clinical and Radiological Evaluation of the Patients
Clinical evaluations were performed preoperatively as well as at 3.1 ± 0.5, 12.1 ± 1.1 and 25.3 ± 3.6 months postoperatively using the HSS-, WOMAC- and SF-36 score [14]. The HHS score has a maximum of 100 points and considers subjective functional (62%) as well as objective examination criteria (38%). The domains include pain (30 points), function (22 points), range of motion (18 points), muscular strength (10 points), deformity (10 points) and instability (10 points).
Radiological evaluation were performed by standard anterior-posterior and lateral X-rays taken on day 5 postoperatively, providing a baseline and at each point of the evaluation. Radiolucent lines and osteolysis of the femoral and tibial bone stock and implant positioning were evaluated by three independent observers. Implant position was measured by the medial distal femur angle (MDFA), medial proximal tibia angle (MPTA), posterior distal femur angle (PDFA) and posterior proximal tibia angle (PPTA).
Statistical Analysis
All data were stored and analysed using the SPSS statistical package 15.0 (SPSS Inc. Chicago, Illinois, USA). Descriptive statistics were computed for continuous and categorical variables. The statistical evaluation included means and standard deviations (SD) of continuous variables, frequencies and relative frequencies of categorical factors. For continuous variables the interval mean ± SD are presented. Comparisons were performed by the Friedman-test (FR) and the Wilcoxon test (WI), respectively between the time points of clinical and radiological evaluations. Test selection was based on evaluating the variables for normal distribution employing the Kolmogorov-Smirnov test. All p values resulted from two-sided statistical tests and values of p < 0.05 were considered to be statistically significant. If necessary, adjustments of the alpha level were carried out by Bonferroni correction. That means that we have lowered the level of significance to 0.05/6 = 0.008 for paired comparisons between the four time points of evaluation.
RESULTS
Overall, 110 total knee arthroplasties were enrolled in the study, but the number of evaluated knees was reduced to 104 at 3 months, 102 at 12 months and 96 at 24 months. At 3 months, six patients could not be evaluated as one patient had died due to myocardial infarction and three patients withdrew consent for personal reasons. In one case, the patient was lost to follow-up for unknown reasons. An intensive effort to find out the reason did not yield any results. One patient was not evaluated at 3 months for personal reasons, but was followed up at 12 and 24 months. Three patients dropped out at the 12 months evaluation, one patient due to a gastric cancer that required a prolonged hospital stay, one patient with a bilateral implantation underwent explantation of one TKA due to early infection and one patient was not evaluated at 12 months but underwent the 24 month follow-up. At 24 months seven patients could not be evaluated as one patient had died due to natural reasons, four patients withdrew consent for personal reasons and in two patients the implant was explanted due to infection. One of these cases was caused by postoperative opening of the knee joint because of direct trauma one week after hospital discharge and revision surgery with change of insert could not prevent prolonged infection. Five patients underwent reoperation due to reasons unrelated to the implant materials without revision of the ceramic component. One patient underwent osteosynthesis due to a periprosthetic fracture after trauma, in two patients a retro-patellar replacement was inserted at one year postoperatively, in one patient there was a change of insert due to traumatic instability and in one patient an arthrolysis was performed in order to improve poor range of motion.
HSS-, WOMAC- and SF-36 scores improved significantly (WI test p < 0.001) from the preoperative to the postoperative evaluations at 3, 12 and 24 months (Table 1). Improvements in all scores were seen especially up to 12 months, whereas differences in all scores between 12 and 24 months were small. Significant improvements were seen in the domains of pain, function, muscular strength, deformity and instability. Range of motion and correspondent domain motion was evaluated as non-significantly decreased at 3 months in comparison to the preoperative assessment (WI test p = 0.013). The 12 and 24 months evaluation revealed significant improvement of domain motion and range of motion in comparison to the 3 months (WI test p < 0.001) and non-significant improvement in comparison to the preoperative assessment (WI test p ≥ 0.022). Nevertheless, the early postoperative period up to 3 months showed the highest decrease in pain and functional derogation.
Mean Pre- and Postoperative HSS-, WOMAC- and SF-36 Score Values Including Domains of HSS Score and Range of Motion
| Preoperative (I) | 3 Months (II) | 12 Months (III) | 24 Months (IV) | FR-Test | WI-Test | |
|---|---|---|---|---|---|---|
| HSS score (100) | 55.5 SD 11.5 | 77.2 SD 10.3 | 85.6 SD 8.9 | 85.7 SD 11.7 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.387 |
| Pain (30) | 10.1 SD 6.6 | 22.9 SD 5.8 | 26.3 SD 5.1 | 26.6 SD 5.9 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.355 |
| Function (22) | 12.6 SD 4.3 | 16.9 SD 3.5 | 18.6 SD 4.0 | 18.9 SD 3.3 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.761 |
| Motion (18) | 13.6 SD 1.9 | 12.9 SD 1.7 | 14.0 SD 1.9 | 13.8 SD 2.7 | p<0.001 | I vs II p=0.013 I vs III p=0.087 I vs IV p=0.066 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.971 |
| Muscular strength (10) | 7.6 SD 2.6 | 8.7 SD 2.1 | 9.5 SD 1.3 | 9.6 SD 1.0 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p=0.002 III vs IV p=0.423 |
| Deformity (10) | 7.1 SD 2.8 | 9.0 SD 2.0 | 9.8 SD 0.5 | 9.8 SD 0.8 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p=0.002 III vs IV p=0.967 |
| Instability (10) | 8.1 SD 1.5 | 9.7 SD 0.7 | 9.6 SD 0.9 | 9.6 SD 0.9 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p=0.050 III vs IV p=0.740 |
| WOMAC score (100) | 48.1 SD 16.6 | 63.9 SD 18.5 | 74.1 SD 17.4 | 71.5 SD20.0 | p<0.001 | I vs II p<0.001 I vs III p<0.001 I vs IV p<0.001 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.961 |
| SF-36 score (100) | 49.1 SD 17.6 | 56.2 SD 21.3 | 63.9 SD 19.2 | 62.3 SD 22.6 | p=0.001 | I vs II p=0.004 I vs III p<0.001 I vs IV p<0.001 II vs III p=0.007 II vs IV p=0.010 III vs IV p=0.786 |
| ROM | 108.8° SD 15.7° | 103.3° SD 13.3° | 112.3° SD 15.1° | 112.6° SD 15.0° | p<0.001 | I vs II p=0.013 I vs III p=0.087 I vs IV p=0.022 II vs III p<0.001 II vs IV p<0.001 III vs IV p=0.792 |
Standard deviation (SD) and p-values for the Friedman (FR) and Wilcoxon (WI) test are presented. Significant differences are marked with bold letters.
Radiological Results
The positioning of the implant in the postoperative radiographs is demonstrated in Table 2. An intraoperative intramedullary valgus alignment between 5° and 9° depending on the preoperative valgus of the femur was used and the pre-defined implant slope was 7°. Implant positioning was considered as optimal (aberrance < 3°), as fair (> 3° and < 5°) and as poor (> 5°). Changes in implant position or migration during the 24 month follow-up were not observed in any cases (Fig. 2).
Implant Position Measurement Demonstrated by the Medial Distal Femur Angle (MDFA), Medial Proximal Tibia Angle (MPTA), Posterior Distal Femur Angle (PDFA) and Posterior Proximal Tibia Angle (PPTA).
| Implant Position (Number of Patients in %) | |||
|---|---|---|---|
| Optimal (<3°) | Fair (3°-5°) | Poor (>5°) | |
| MDFA | 55 (50.0%) | 32 (29.1%) | 23 (20.9%) |
| MPTA | 46 (41.8%) | 47 (42.7%) | 17 (15.5%) |
| PDFA | 73 (66.4%) | 29 (26.4%) | 8 (7.3%) |
| PPTA | 31 (28.2%) | 39 (35.5%) | 40 (36.4%) |
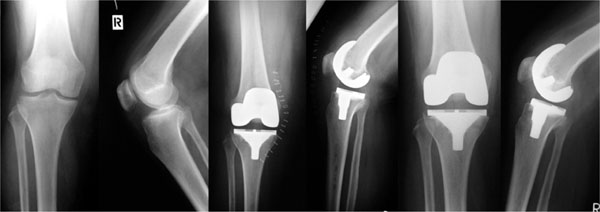
X-rays of a 75-year-old female preoperative, 5 days and 24 months after the implantation of a Delta Ceramic Multigen Plus Knee with BIOLOX® ceramic femoral component.
Radiolucent lines around the femoral ceramic component at 24 months were found in 3 cases in one zone and in 1 case in two zones. All radiolucent lines measured up to a maximum of 1 mm and were located between the bone and cement (Fig. 3). Radiolucent lines around the tibial component were found in 17 cases after 24 months follow up. Zone 1 (n=8) and zone 4 (n=9) showed the majority of radiolucent lines, up to 2 mm, which were located between the bone and cement. Progression of radiolucent lines was not seen around the femoral and the tibial component in any case. Within the clinical evaluation, implant loosening cannot be assumed in any case.
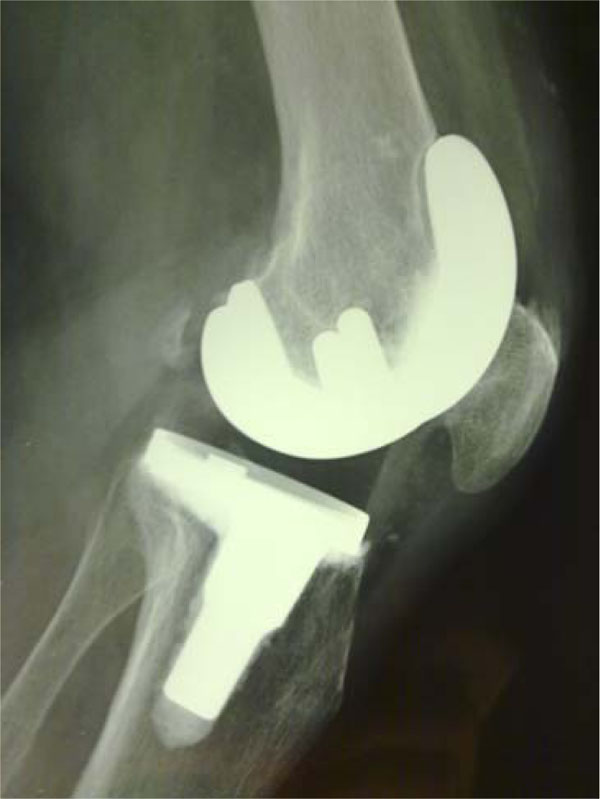
Lateral X-ray 12 months after implantation of a Delta Ceramic Multigen Plus Knee with BIOLOX® ceramic femoral component. A radiolucent line up to 1 mm is seen in Zone 1.
DISCUSSION
Since the number of primary TKAs, especially in younger patients, is increasing, the demand for the best available outcome, including higher mechanical loading and optimal kinematics (maximum range of motion) has become more important for excellent long-term function and stability. Wear is one major reason for implant failure in TKA [3]. The biologic effect of wear particles depends on the material and volume of wear particles. Furthermore, modern TKA components are made of titanium or cobalt-chromium alloys. Cobalt-chromium and nickel have the greatest potential to cause allergic reactions [4]. Bioinert ceramic implants are an option for metal sensitive patients and can reduce the release of wear particles. Therefore, ceramic implant designs for TKA were developed [3, 5, 13, 15].
In this prospective international multi-centre study, we examined a total knee replacement system with the BIOLOX® delta ceramic femoral component concerning early radiological and functional outcome. The study was performed as a prospective non-comparative study for evaluation of the ceramic femoral component. The first limitation of the study is that selected patients were not consecutive or randomised and the degree of the deformity was, in general, moderate. The reasons for these limitations were correlated with the nature of the study and with proving the clinical reliability of the newly developed ceramic femoral component.
The radiological evaluation revealed radiolucent lines around the femoral ceramic component in four cases. In contrast, we observed radiolucent lines on the tibial side in up to 16%. This may be due to a stress-shielding phenomenon and is described up to 17%. Progression can usually not be expected if a malalignment is non-existant [16, 17].However, subsequent follow-up investigations have to be performed to clarify if the progression of radiolucent lines influence clinical results and implant survival rates.
The clinical evaluation showed significant improvements in all scores from the preoperative to the postoperative evaluations. The early postoperative period (up to 3 months) revealed the highest decrease in physical and psychological functional derogation, with the exception of range of motion [1]. Aarons et al. [18] evaluated differences of the early functional outcome after TKA and THA. After THA, patients showed significant improvement in physical function and quality of life after 7 weeks, but in patients with TKA, these early effects could not be evaluated. Within the first 7 postoperative days, psychological aspects improved similarly in the TKA and THA groups, due to the relief of preoperative stress and depression. With regard to these findings, range of motion as a functional aspect improved most between 3 and 12 months. Overall, improvement can be expected to a minimum of 2 years postoperatively and were seen in the study [19].
We observed a higher HSS score of 85.6 points at 3 months postoperatively in comparison to 75.6 points using a different non-constrained surface replacement knee system [1]. The clinical outcome of the Multigen Plus Knee with a BIOLOX® delta ceramic femoral component demonstrates results comparable to other studies, which reported a mean postoperative (1 year) HSS score between 85.0 to 93.0 points [20, 21]. Evaluations of other ceramic TKAs showed a HSS score of 86 points after a follow up between 2 and 10 years [22-24]. Bin et al. [20] evaluated the range of motion of a knee system in both standard and high flexion designs. Achieving an excellent HSS scores in both study groups (HSS score 92.0–93.0), significant differences in range of motion were found (129.8° ± 5.2° versus 124.3° ± 9.2°). TKAs using ceramic components evaluated range of motions between 113°–124° [23, 24]. The Multigen Plus Knee, as a standard design prosthesis, shows a slightly reduced range of motion at 112.3° ± 15.1° (range 70°–150°). However, the comparability of different clinical studies is compromised by some influencing factors, such as implant design, preoperative function and the demographics of the study patients.
Oonishi et al. [10] reported the results of 108 patients mainly treated with surgery with cementless total alumina prosthesis. There were 9 cases of aseptic loosening with implant dislocation at a follow-up between 5 and 8 years. Therefore, fixation of ceramics without cement is not recommended and the Multigen Plus Knee in our study was only implanted with PMMA cement with a cement layer of approximately 2 mm. Leyen et al. [25] recommended that ceramic knee endoprostheses should be fixed with bone cement. Bone cement can act as a force transmitter between bone and ceramics with two different Young’s modulus. Experimental testing showed that thinner cement layers lead to an increase in tensile bond strength [25]. A recently published in vitro study rejected the hypothesis that cemented ceramic TKA femoral components are more prone to mechanical loosening [26]. Furthermore, future efforts have to be made to modify ceramic surfaces in order to realise cementless fixation by bony in-growth, in the event of allergies to bone cement components.
Material fractures are considered a problem of ceramics in joint arthroplasty. Long-term results (follow-up ranging from 5 to 10 years) of 105 cemented alumina ceramic knee prostheses (Kyocera Corp., Kyoto, Japan) showed a tibial plate fracture in one case, but the fracture of metal implants have also been reported [22, 24, 27]. BIOLOX® delta ceramic is a composite matrix material containing aluminium oxide (Al2O3) and zirconium oxide (ZrO2), which has improved the mechanical characteristics in terms of strength and resistance. In the case of ceramics, once the elastic limit has been overcome due to a defect, the crack will propagate and a complete fracture will occur. Zirconium oxide particles, which are finely distributed in the stable alumina matrix, will change phase from tetragonal to monoclinic once there is a crack. This phase change increases the particle volume up to approximately 5%, which helps reduce energy consumption and can stop crack propagation by closing the crack space [15].
We observed four fractures of the BIOLOX® Delta ceramic femoral condyle during the implantation procedure at the beginning of the study, with no consequences for the patients. However, no fractures of the implanted components were observed during the 24 month follow-up. Failure analysis showed that the fracture lines were located in the corners of the femoral resection. Fractures may happen during the surgery procedure due to an inadequate anterior and posterior bone resection resulting in high tension stress during the impaction of the femoral condyle with a hard instrument (hammer). Finite-element analysis confirmed this fact [11]. Therefore, a precise intraoperative preparation of the bone stock and the use of a newly developed additional resection template for an extended anterior and posterior resection are required to avoid stress concentration by reducing wedge loading during impaction. The additional resection leads to an adequate thickness of the cement layer [25].
CONCLUSIONS
The good short-term results of the present study indicate a successful implementation of the Multigen Plus Knee with BIOLOX® delta ceramic femoral component in clinical application. Ceramic implants are a promising solution for patients with allergies against metallic implant materials [28, 29]. However, careful intraoperative handling has to be considered using ceramic femoral components. A long-term prospective comparative study with the ceramic and metallic Multigen Plus Knee is in progress in order to compare the clinical results and implant survival rates.
CONFLICT OF INTEREST
Some authors have received benefits for personal or professional use from a commercial party NOT related to the subject of this article. In addition, benefits have been or will be directed to a research fund, foundation, educational institution, or other non-profit organisations with which one or more of the authors are associated.
ACKNOWLEDGEMENT
Declared none.


