All published articles of this journal are available on ScienceDirect.
Fractures and Alcohol Abuse – Patient Opinion of Alcohol Intervention
Abstract
Purpose:
To clarify patient opinions about alcohol intervention in relation to surgery before investigating the effect in a Scandinavian multi-centre randomized trial.
Material and Methods:
A qualitative study. Thirteen consecutive alcohol patients with fractures participated after informed consent. They were interviewed during their hospital stay. The number of participants was based on the criteria of data-saturation. The analysis followed the applied qualitative framework model aimed at evaluation of specific participant needs within a larger overall project.
Results:
All patients regarded alcohol intervention in relation to surgery as a good idea. They did not consider quit drinking as a major problem during their hospital stay and had all remained abstinent in this period. About half of the patients were ready or partly ready to participate in an alcohol intervention. Patient opinions and their readiness to participate were expressed in four groups, which also reflected their readiness to stop drinking in the perioperative period, their general acceptance of supportive disulfiram as part of an alcohol intervention as well as their awareness of postoperative complications.
Conclusion:
This study clarified that the patients found alcohol intervention relevant in relation to surgery.
INTRODUCTION
Alcohol intake is an independent risk factor for patients undergoing surgery [1]. For elective surgery 4 weeks preoperative alcohol cessation can half the frequency of postoperative complications [2], which is implemented for elective procedures in several surgical departments [3]. Hitherto, no studies have focused on reduction of postoperative complications after emergency procedures, such as fractures, though pathophysiological studies indicate a positive effect [4]. The effect of alcohol cessation intervention on complications after acute surgery is therefore still unknown.
A new Scandinavian patient education program [Scand-PEP] is based on the previous preoperative program [2] and inspired by perioperative smoking cessation programs [5, 6]. Scand-PEP is scheduled with weekly meetings to support minimum 6 weeks alcohol cessation; including alcohol withdrawal prophylaxis and supervised disulfiram. The first meeting will be conducted before or soon after the operation. All meetings take place in the orthopaedic department.
Whilst developing the Scand-PEP a qualitative study was conducted to clarify patient opinions about alcohol intervention in relation to surgery before evaluating Scand-PEP in a multi-centre trial. Qualitative interviews alongside randomised clinical trials remain uncommon, but are increasingly being advocated [7] for ensuring best evidence-based practice including patient preferences [7, 8]. Correspondingly, this qualitative study adds knowledge on alcohol patient preferences, where the results can be used to improve patient recruitment and intervention. This information will be useful in the subsequent Scandinavian multi-centre RCT, which aims at evaluating the effect of Scand-PEP on postoperative complications for alcohol patients in acute fracture surgery.
MATERIAL AND METHODOLOGY
Design
A qualitative study based on Ritchie & Spencer’s model for an “applied qualitative framework” [9]. This model was developed especially for research aimed at evaluation of specific participant needs within a larger overall project and therefore very well suited for the aim of this study. This qualitative model implies that both the pre-specified topics and questions from the interview guide as well as additional comments and responses that emerge in the interviews are answered and analysed.
Participants
Thirteen consecutive fracture (mainly hip fractures) patients (8 men) admitted to orthopaedic department at Bispebjerg Hospital from December 2008 to February 2009 aged 28-78 (median 57) drinking at least 21/14 drinks per week for men/women according to the recommended maximum drinking limits in Denmark [10] participated in individual interviews after informed consent. Eight of the patients drank at least 5 drinks per day, where the risk of postoperative complications is 300-500% increased compared to 0-2 drinks per day [4]. Patients were excluded if they had severe alcohol dependence (symptoms of delirium or seizures), insufficient language proficiency or reduced ability for giving informed consent (including ebriation and drug influence). Of 19 eligible patients, three refused to participate, two were discharged and one was transferred to another department before inclusion, thereby 13 patients were included in the study.
All but two patients were daily smokers. Three of the patients were at risk of malnutrition (BMI < 20.5) [11] and two were overweight (BMI > 25). No patients were employed (ten retired and three were unemployed); eight of the 13 patients had none or a very short education. Seven of the patients lived alone, four were living with a partner or cohabitant, one was living in a shelter and one was homeless.
The number of participants needed in an interview study cannot be estimated by power calculations. Instead the criterion of ‘data saturation’ was used, which indicates when it is considered unlikely that any new data would surface by conducting further interviews [12]. Patient inclusion was therefore concluded after 13 interviews as the same answers and comments kept emerging.
Procedure
Eligible patients were identified based on information on alcohol intake registered in the medical records. The interviews lasted 20-50 minutes and were conducted in the orthopaedic department during hospital stay. Ten of the 13 patients had undergone osteosynthesis at the time of the interview.
In the written and oral information as well as in the interviews it was emphasized that the Scand-PEP was not a specific offer in which the interviewed patients could participate, and that the purpose of the interviews was solely to gain insight into patient opinions about alcohol intervention in relation to surgery. All patients admitted to the hospital were routinely informed about the free alcohol programs in the community.
A semi-structured interview guide was developed and tested on a pilot patient. A semi-structured interview guide is organised around a set of predetermined open-ended questions, but also allowing for additional questions emerging from the dialogue between the interviewer and interviewee [13]. No major changes were made after the pilot, and this interview was therefore included in the study. The interview guide contained four major pre-specified research topics including a presentation of the Scand-PEP (Table 1). To open the interview session the patients were encouraged to speak freely about their surgical pathway. They were given short information on alcohol and the increased risk of postoperative complications as well the effect of alcohol cessation intervention in relation to surgery. At the end of the interview the focus changed to smoking (see themes and answers in Table 2).
The Scand-PEP Presented for the Interview Patients
| Patient Education | Intervention and Monitoring |
|---|---|
|
1st meeting - Level of motivation, alcohol profile, ambivalence, pros and cons |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
|
2nd meeting (after 1 week) -Dependence, withdrawal symptoms (experiences and expectations) |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
|
3rd meeting (after 2 weeks) - Relapse (description and management) |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
|
4th meeting (after 3 weeks) -Benefits by short and long term alcohol cessation |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
|
5th meeting (after 4 weeks) - Alcohol cessation or reduced intake following intervention |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
|
Follow-up (after 3 6 9 and 12 months) - Alcohol profile |
- Supervised disulfiram, withdrawal treatment and B-vitamins, blood and urine test |
Interview Guide with Pre-Specified Topics and Answers
| Opening Questions: Experience of Hospital Stay, Previous Surgery/Complications |
|
|
| The patients were satisfied with their hospital stay and expressed trust and faith in the staff. Most patients had undergone complication-free surgery in the past. |
|
|
|
|
|
| The patients considered postoperative complications as important. |
| The information was sparse. |
|
|
|
|
|
| All the patients described previous attempts to reduce or quit drinking for shorter or longer period. All but two were satisfied with the supportive alcoholfree setting in the orthopaedic department. They did not regard quit drinking as a major problem during their hospital stay; all had remained abstinent in this period. Half of them would reduce or quit drinking in the postoperative period |
| Most of the patients expected complication-free surgery. |
|
|
|
|
|
| The patients thought that Scand-PEP was a good idea. |
| They had no suggestions for improvement in general, but they all had comments on the use of supervised disulfiram intake. Nine had previous experiences with disulfiram, and two were currently using it to support alcohol cessation. |
| Three patients described disulfiram as essential for completion of an alcohol intervention program, which was not commented by the others. |
|
|
|
|
|
| Nine of 11 smokers did not smoke during the hospital stay. |
| Four patients used nicotine replacement therapy during their hospital stay. |
| None of the patients planned to continue smoking cessation following discharge. |
| Half of the smokers had tried to quit smoking in the past, and four patients were positive towards a combined alcohol and smoking intervention. |
To strengthen credibility the interviewer’s pre-understanding of the alcohol patients and their possible opinions about alcohol intervention was assessed.
Analysis
The interviews were tape-recorded and transcribed. The analysis included five phases [9]; most importantly construction of a thematic framework, which drew on both a priori themes specified in the interview guide as well as other key findings from the interviews. All transcripts were coded according to the thematic framework. The final interpretation included a grouping of patient opinions on alcohol intervention. The grouping was determined during the interview process and the four groups are defined in the results.
The study profile including the analysis and interpretation is illustrated in Fig. (1).
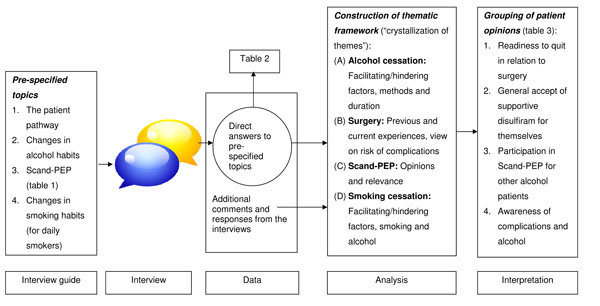
Study profile (flow chart).
RESULTS
Grouping of Patient Opinions on Alcohol Intervention
Patient opinions and their readiness to participate in Scand-PEP were expressed in four groups, which also reflected their readiness to stop drinking in the perioperative period, their general acceptance of supportive disulfiram as part of an alcohol intervention as well as their awareness of postoperative complications (see Table 3).
Grouping of Patient Opinions on Alcohol Intervention (Quotes are Given in Italic Text)
| Readiness to Enter Scand-PEP/Patient Opinions | Readiness to Quit in Relation to Surgery | General Accept of Supportive Disulfiram for Themselves | Participation in Scand-PEP for Other Alcohol Patients | Awareness of Complications and Alcohol |
|---|---|---|---|---|
|
Group 1 (3 patients): YES “ I would like to try such things, you see. I would really like to try such things, so I’m totally okay with that”, (interview 4; woman, age 60). |
YES | YES | YES | HIGH |
|
Group 2 (3 patients): PARTLY, yes “ That is a difficult one. Yes... I don’t know. I’m not sure. That is I would like to maintain my freedom, and that does not necessarily mean freedom to drink, but that is freedom to control my own life in that way, well without destroying life of course. Do you understand what I mean, or is it totally in vain?”, (interview 3; woman, age 50) |
YES | PARTLY | YES | MIXED |
|
Group 3 (4 patients): PARTLY, no ”Well, I think it’s a good idea for those who will benefit from it, I really think so. And then there are always a few who are just as insane as I am”, (interview 9; man, age 66) |
PARTLY | NO | YES | LOW |
|
Group 4 (3 patients): NO “ No, I wouldn’t want to at all. Not when it is just alcohol and alcohol, because I’m not an alcoholic, and therefore I cannot answer that question. Then you need to get in touch with the real alcoholics”, (interview 13; man, age 78) |
NO | NO | YES, FOR THE “ REAL ALCOHOLICS” | LOW |
1:. Alcohol Intervention Relevant for all Patients (Including themselves)
This group was very positive towards the Scand-PEP including supportive disulfiram. They regarded it as a program they would like to participate in. They focused on undergoing surgery and the high risk or experience of complications could be a determining factor to quit drinking following surgery.
2:. Alcohol Intervention Relevant for All Patients, but Partly Relevant for themselves
The second group was also positive towards changing their own alcohol habits in relation to surgery, but they were ambivalent towards the Scand-PEP, as own participation in an alcohol intervention triggered conflicting feelings and opinions.
3:. Alcohol Intervention Relevant for All Patients, but Scarcely for themselves
The third group of patients were ambivalent towards changing their alcohol habits and sceptic towards the Scand-PEP and its relevance. They did not think they would benefit from participating or that alcohol cessation in relation to surgery could prevent any possible complications.
4:. Alcohol Intervention Only Relevant for “Severe Alcoholics”, but Not themselves
The last group of patients had no desire to change their alcohol habits. They also had the most negative attitude towards participation in the Scand-PEP, which was seen as appropriate for “real alcoholics” only, and not for themselves.
DISCUSSION
Alcohol cessation intervention in acute fracture surgery may be followed by reduction in both alcohol intake and the development of complications. The opinion among the patients was that the Scand-PEP was relevant for nearly all alcohol patients in relation to surgery. However, the patient approach was clearly related to their individual readiness to change alcohol habits. To our knowledge this is the first study that assessed alcohol patients’ opinions about alcohol intervention aimed at reducing postoperative complications.
Other studies have shown that surgical patients seemed motivated to change drinking habits [14, 15] and to accept alcohol screening as routine procedure [16, 17]. Besides, emergency patients participating in alcohol intervention found the setting appropriate, the information useful and the intervention staff respectful [18].
Parallel to our study on alcohol, other qualitative studies have examined surgical patients’ experience with other lifestyle interventions aimed at reducing the development of complications. Patients were satisfied and motivated by being offered smoking cessation intervention as part of their surgical pathway [19, 20]. Also about 80% of elective surgical patients wanted the hospital to support them in changing lifestyle in relation to surgery after short information about their increased risk of complications [21].
We found that the alcohol patient opinions were equally distributed in four different groups. The most positive patients were characterized by readiness to participate in the Scand-PEP, being ready to quit drinking, accepting supportive disulfiram for themselves and a high awareness of the association between alcohol and postoperative complications, whereas other patients were characterized by the opposite as well as regarding the Scand-PEP as relevant for “alcoholics” only and not themselves.
These results are useful when designing an alcohol intervention as the results fit well into the stages of change model, which defines and characterise the five stages a person is expected to pass during behavior change: pre-contemplation, contemplation, preparation, action and maintenance [22]. The model also supplies the staff with knowledge about how to act and support the person at each stage. From the pre-contemplation to the preparation stage the focus is on influencing attitudes to changing habits by providing education, information, advice and encouragement. From the action stage and onwards the focus is on supporting behavior change until the person has achieved a permanent lifestyle change [23].
This model is helpful in the clinical situation, in which you may misinterpret ambivalence as lack of motivation instead of an important criterion of changing, or you may spend unnecessary time on persuading patients, who are ready to change habits.
In the upcoming Scandinavian trial, it may be easy to include patients in the preparation or action stage. To ensure a high inclusion and completion rate in the overall trial, we can use the present results to adjust the information of the initial meeting and make an extra effort to reach out to the patients in the pre-contemplation and contemplation stage. Furthermore, patients in the intervention group will receive the Scand-PEP, which support the changing process through education, advice and encouragement aimed at alcohol cessation in the peri- and postoperative period.
The study has both strengths and limitations. Firstly, patient inclusion was continued until data saturation, which is crucial in qualitative methodology. Thus, including more than 13 patients would probably not have altered the results of the study. Secondly, the grouping of patient opinions found by using a qualitative design could not have been found in a traditional questionnaire survey, where only the pre-specified themes and answers are investigated. Here, additional topics from the interviews were integrated together with the pre-specified themes. Thirdly, the interviews were conducted among alcohol patients in one of the orthopaedic departments participating in the coming multi-centre trial. However, despite the similarities in setting and patients it cannot be assumed that the positive interview patients would actually follow the Scand-PEP. Furthermore, the option to actually participate and receive Scand-PEP may prompt another approach compared to the interview setting. Also the generalisation may be reduced because Denmark has a higher average alcohol intake and a long tradition for the use of disulfiram in treatment of alcohol abuse compared to other Nordic countries [24, 25]. Therefore, it is possible that patients in Norway and Sweden would have different opinions and experiences, which would limit the generalisation to the other two countries that participate in the trial. Nevertheless, adding an interview study to a randomised trial may improve its completeness and performance. In the multi-centre trial we can now anticipate and meet patient opinions during recruitment and intervention, e.g. by using the stages of change model.
CONCLUSION
In conclusion, this study clarified that the patients found Scand-PEP relevant in relation to surgery. About half of the patients were ready or partly ready to participate in an alcohol intervention. Patient opinions and their readiness to participate were expressed in four groups, which also reflected their readiness to stop drinking in the perioperative period, their general acceptance of supportive disulfiram as part of an alcohol intervention as well as their awareness of postoperative complications.
TRIAL REGISTRATION
The Scientific Ethical Committee for the Capital Region of Denmark [2008.11.11, H-C-2008-119] approved the study.


