All published articles of this journal are available on ScienceDirect.
Congenital Knee Dislocation: Which Classification to Follow?
Congenital knee dislocation (CKD) was first reported by a Swiss physician Chatelaine, in the year 1822 [1], but even after the passage of two centuries, the exact treatment protocol is still debatable. CKD is a hyperextension deformity of the knee with anterior tibia displacement, present at birth. It may be idiopathic or syndromic (Larsen’s syndrome, arthrogryposis multiplex congenita, myelomeningocele) [2-4]. The incidence of CDK is 1/100,000 in live births [5, 6]. To make it simple, it is 1% of the incidence of congenital hip dislocation [7, 8]. The exact etiology remains unknown. CDK manifests in the second half of pregnancy [9]. It has been associated with certain factors, including extrinsic factors such as intrauterine packaging disorders, breech presentations, and intrinsic factors like genetic malformation, but most of the cases are sporadic.
Neuromuscular imbalances have also been implicated to be a risk factor for CDK. In most cases, changes may occur in quadriceps muscles and cruciate ligaments, and even contractures may develop. The deformity may be unilateral or bilateral and mostly affect girls, but some literature reports equal distribution [1, 10, 11].
Orthopaedic surgeons have limited exposure to this deformity and only two major articles have been published in over the past decade proposing new or modified classifications for the management of CDK. Still, there is a lot of debate regarding which classification system to follow as treatment guidelines.
Which way forward?
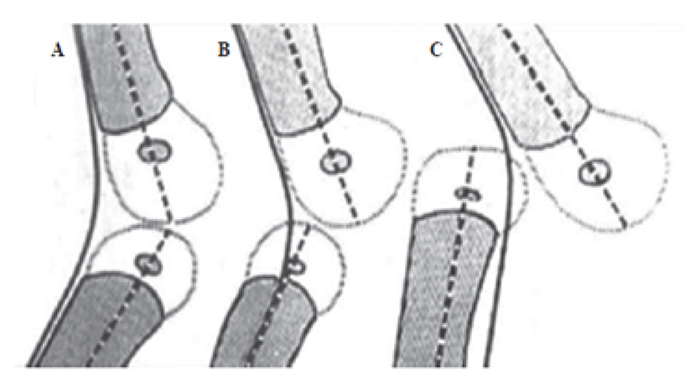
Leveuf J. and Pais C. classification [12] separates the deformity into three subgroups (Fig. 1). Grade 1 is the most common type and not a true dislocation and accepted as congenital hyperextension. Nearly 15 to 20° of hyperextension can be detected and passive range of flexion is maximum 90°. In Grade 2, congenital subluxation with joint incongruency is observed. Passive flexion of the knee is impossible and 25 to 40° of hyperextension can be achieved. In Grade 3, there is no contact between the joint surfaces of tibia and femur. This classification is based only on radiological views without an assessment of clinical manifestations.
Laurence classification is based only on a retrospective assessment of the success or failure of non-operative treatment [13], which cannot be used in planning of treatment tactics.
According to Abdelaziz T.H. grading system of CDK (Table 1), based on the initial range of passive knee flexion [2], serial casting is performed in patients with grade I (GI). In GII CDK in neonates (babies up to the age of 1 month), serial casting is started. A maximum of four weekly manipulations and castings are attempted. If a range of flexion >90° is achieved, serial casting is continued, but if the range of flexion remains <90°, it is necessary to proceed to PQR.
In babies older than 1 month, when first seen, percutaneous quadriceps recession (PQR) is performed from the start. V-Y quadricepsplasty (VYQ) is indicated in patients with GIII CDK or in recurrent cases. We feel that age more than one month or grade III CKD itself should not be a qualifying criteria for PQR/VYQ, rather clinical examination and response to treatment should guide further management.
| Grade | Range of Passive Flexion | Radiology |
|---|---|---|
| GI | >90° | Simple recurvatum |
| GII | 30-90° | Subluxation/dislocation |
| GIII | <30° | Dislocation |
According to Mehrafshan M. et. al. [14] reduction and stability criteria, there are 3 types of CKD. Type I is easily reducible CDK, with reduction snap when the femoral condyles pass in flexion, remaining stable. Type II is “recalcitrant” dislocation, reducible by posteroanterior “piston” but unstable, with iterative dislocation once posteroanterior pressure on the condyles is relaxed. Type III is irreducible dislocation.
This classification of CDK, based on neonatal clinical examination ahead of any treatment, looks promising and has better prognostic value. Initial examination also notes the number of transverse anterior skin grooves, range of motion (hyperextension, maximum flexion and global range: flexion + extension). The greater the number of anterior skin grooves, the more recent the in utero origin of dislocation, while the absence of grooves indicates long-standing dislocation. Flexion is more impaired in type III than type II and less impaired in type I, which corresponds to quadriceps retraction and also indicates the duration of in utero dislocation.
We found Mehrafshans’ classification more practical and having better prognostic value. In our opinion, the treatment of children with CKD should be started early after detailed clinical assessment with conservative methods, including serial manipulation and casting. Surgical interventions like V-Y quadricepsplasty (VYQ), percutaneous quadriceps recession (PQR), and other soft tissue procedures should be reserved for resistant cases and for older age children. Over the age of 2 years, the Ilizarov apparatus can be used for stiff knee deformity [15].
FUNDING
None.
CONFLICT OF INTEREST
The author declares no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


