All published articles of this journal are available on ScienceDirect.
Cement Arthrodesis of the Knee with a Custom Long Recon Nail After Failed Total Knee Arthroplasty: Surgical Technique and Results
Abstract
Background and Objective:
Persistent periprosthetic joint infection (PJI) is a devastating complication after Total Knee Arthroplasty (TKA). We hypothesize that our novel treatment algorithm utilizing a customized knee spanning recon nail combined with an antibiotic eluting cement spacer improves ambulation status and prevents recurrent PJI in patients with failed TKA and severe bone loss.
Methods:
In a retrospective case series, 15 consecutive patients who underwent knee arthrodesis after failed ipsilateral TKA secondary to infection from 2004-2017 with at least 1 year of follow-up were enrolled. The average age of patients at the time surgery was 68 (range 50-81) years with an average follow-up of 3.2 (range 1-6) years. Post-surgical ambulation status and eradication of index infection were analyzed as primary outcomes using McNemar’s test for before-and-after study design with p<0.05 for significance.
Results:
Cement arthrodesis significantly improved ambulation with 67% (10/15) of patients unable to ambulate before arthrodesis and 93% (14/15) of patients able to ambulate at final follow-up (p=0.004). The complication rate was 20% (3/15). There were no periprosthetic fractures. Amongst patients who presented with active PJI, 91% (10/11) had eradication of their index infection final follow-up (p=0.002). Overall prevention of recurrent index infection was 93% (14/15) (p=0.0001).
Conclusion:
Cement arthrodesis utilizing a custom knee spanning recon nail combined with an antibiotic eluting spacer improves ambulation status and prevents or treats recurrent infection in the majority of patients who have failed total knee arthroplasty.
1. INTRODUCTION
Knee arthrodesis should be strongly considered as a limb-sparing procedure in the setting of failed Total Knee Arthroplasty (TKA) with severe bone and/or soft tissue loss [1-17]. The crude incidence of arthrodesis after TKA is cited between 0.21 and 1.11% [1, 18-20]. The most common indication for knee arthrodesis after TKA is a persistent Periprosthetic Joint Infection (PJI) after staged revision procedures proved unsuccessful [1, 21]. , [22] Revision TKA in the setting of infection confers a 7% lifetime risk of arthrodesis or amputation [23]. Notably, patients undergoing fusion for the end-stage treatment of persistent knee PJI tend to have better function and ambulatory status when compared to alternative treatment with amputation [24]. Other indications for arthrodesis after failed TKA include extensor mechanism dysfunction, soft tissue compromise, and severe bone loss, with almost half of patients having more than one indication [1].
Knee arthrodesis has been performed for over 2000 years, with evidence of a clinically healed knee fusion demonstrated from radiographic studies of an Egyptian mummy dating from the classical era (Appendix 1). In the modern era, primary stability of the knee can be achieved by external fixation typically with an Ilizarov apparatus, internal fixation with a plate, or intramedullary nailing [7, 25-28]. each technique offers its own set of advantages and drawbacks as a salvage procedure for failed TKA. External fixation has the benefit of avoiding placement of implants directly into a potential nidus of infection, theoretically providing a lower risk of intramedullary dissemination. Despite predisposing the patient to pin site infections, the success rate for eradicating infection can be higher in patients treated with external fixation when compared to internal fixation methods [1, 29]. The cosmetic and functional disadvantages of external fixation are obvious as the fixators are very cumbersome to patients and necessitate a prolonged course of treatment prior to removal. Arthrodesis with internal knee spanning plate and screw constructs is currently uncommon and puts excessive stress on the already damaged soft tissue envelope, predisposing to wound healing issues. Additionally, plate fixation typically subjects the patient to an extended period of protected weight bearing. Alternatively, intramedullary nailing allows for full weight bearing with a significantly higher fusion rate than an external fixation [1]. With traditional arthrodesis techniques, the bone ends must be coapted to successfully fuse which often results in significant shortening of the limb. Furthermore, the bone remnants are often sclerotic and have compromised potential for healing.
We have designed a technique utilizing a customized recon nail combined with a cement spacer as an alternative to amputation in the setting of failed total knee arthroplasty. The implant spans the knee with two different radii of curvature and diameters to accommodate the distinct morphology of the femur and tibia. Additionally, the design features prophylactic fixation into the femoral neck, given the increased risk of geriatric fractures in this susceptible patient population. A static cement spacer containing appropriate antibiotics intercalates with the distal femur and proximal tibia. This rebar-in cement construct protects against axial loading to prevent limb shortening while optimizing bending strength. The spacer elutes high concentration antibiotics to prevent or treat the recurrent infection. Using a before and after study design, we assessed our hypothesis that our novel cement arthrodesis protocol improves ambulation and prevents or treats recurrent infection after failed TKA.
2. MATERIALS AND METHODS
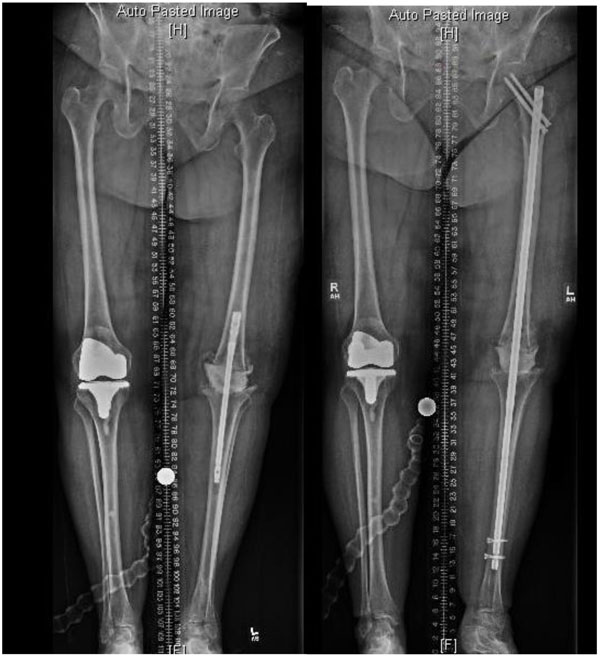
After Institutional Review Board approval and informed consent were obtained, 15 consecutive patients were retrospectively identified who underwent cement arthrodesis of the knee by the senior author after a failed ipsilateral TKA from 2004-2017. These patients were deemed to not be candidates for replantation arthroplasty by the referring surgeon secondary to significant bone loss with limb shortening, poor soft tissue envelope, or refractory infection. Patients who were deceased (5), unreachable (3), or had less than 1-year follow-up were excluded. Patients were given the option of above knee amputation or cement arthrodesis, preoperatively. If there was a concern for persistent infection upon presentation to the senior surgeon, as indicated by Musculoskeletal Infection Society criteria [30], the patient would undergo a 2 stage procedure in which the affected knee initially underwent irrigation and debridement with placement of a temporary antibiotic spacer and treatment with systemic antibiotics (Fig. 1). Definitive arthrodesis was then performed upon normalization of inflammatory markers for at least 2 weeks after cessation of antibiotics administration. All other patients had negative inflammatory markers at presentation without concern for persistent infection and underwent definitive knee arthrodesis in a single stage. Standing long leg AP radiographs were used for preoperative templating a few weeks prior to guide fabrication of the custom nail (Smith & Nephew, London, UK) to the desired length and diameter. The exact dimensions varied dependent on the patient’s size but in general, implants were around 800mm in length with a femoral diameter of 11.5mm and tibia diameter of 10.0mm.
There were 7 men and 8 women enrolled with an average age of 68 (range 50-81) years at the time of surgery. Hospital records were retrospectively reviewed to determine the number of revision surgeries prior to the arthrodesis, length of follow-up, index infection organism, medical comorbidities, ambulatory status, and postoperative complications. The postoperative patient-reported outcomes were measured by administering an SF-12 survey to the patient at final follow up. Postoperative ambulation status and successful eradication of index infection as indicated by the Delphi consensus standard [31] at final follow-up were recorded as primary outcomes. Statistical analysis on primary outcomes comparing patients before and after surgery was performed using the McNemar’s test for paired nominal variables with two-tailed p<0.05 for significance. No funding was used for this study.
3. SURGICAL TECHNIQUE FOR DEFINITIVE ARTHRODESIS
After adequate anesthesia is obtained, the patient is placed supine on a fracture table. Only the ipsilateral foot is sterilely prepped and draped initially. A 3/8” Steinmann pin is placed from medially to laterally across the posterior and inferior aspect of the calcaneus. This is then wrapped sterilely with Kling dressing and the pin is connected to the fracture table to provide an axial distraction. The contralateral limb is placed in a 90/90 position with a well-leg holder to facilitate fluoroscopic imaging. The entire operative flank and limb is then sterilely prepared and draped with care to include the malleolar region distally. Using fluoroscopic guidance, an incision is made over the greater trochanter extending proximally about 5-7 cm. We then dissect down to the proximal tip of the greater trochanter, using electrocautery to achieve hemostasis. A guide wire is inserted into the piriformis fossa and confirmed with AP and lateral imaging. This step may be difficult in patients with a thick soft tissue envelope and a more rigid awl can be used as an alternative method to provide access to the femoral canal. A curved ball-tipped guide wire is advanced to a center-center position in the distal femur.
Attention is now focused on the knee joint. Given that all these patients have had previous knee surgery, we recommend using the most lateral skin incision to provide access to the knee joint and limit wound healing issues related to disruption of vascular supply to the cutaneous tissues. Skin flaps are elevated and a medial parapatellar approach is employed to expose knee joint. Soft tissue releases may be needed to adequately expose the knee. Previous implants or cement are removed carefully to avoid excessive bone loss. A drill bit is used in retrograde fashion to open up the canal of the femur distally and the guide wire is then passed distally through to the knee.
The femur is sequentially reamed anterograde using custom, flexible reamers in 0.5 to 1.0 mm increments to 1.5-2.0 mm up-sized from the true diameter of the femoral intramedullary implant. When inserting the intramedullary reamer, the surgeon uses a medializing manual force to prevent lateralizing the nail entry site.
The surgeon then addresses the tibia directly through the knee arthrotomy. The medullary canal is exposed proximally using either drill bits or a curette. The guide wire is inserted down the anatomic axis to the tibia to the level of the distal physeal scar. Central positioning of the guide wire in two planes is confirmed by AP and lateral imaging. Reaming is performed over this wire from the hip to the ankle beginning with a 9mm end cutting reamer, upsizing in 0.5 to 1.0 mm increments, and ending with a diameter 1.5mm larger than the pre-designated tibial nail diameter. Once the reaming of the femur and tibia is completed, the nail is ready to be inserted.
The intramedullary nail is assembled to the jig on the back table and the recon interlocking screw trajectory is verified to pass through the nail prior to insertion. The nail is inserted to an appropriate depth and rotation so that an interlocking screw can pass through the lateral femoral cortex and end centrally in the femoral head. Coaxial traction can be applied through the calcaneus pin to optimize leg length and rotation. The proximal recon screw is inserted into the femoral head without violating subchondral bone and 2 interlocking screws are inserted into the distal tibia (Fig. 1).
Finally, attention is turned back to the knee joint to complete the rebar and cement technique. Two bags of 40g of polymethylmethacrylate are mixed with 4g of vancomycin and 6.75g of piperacillin/tazobactam or other antibiotics as indicated based upon available sensitivities. Once doughy, the cement is packed into a dry wound bed around the nail to fully fill the bone defect. The image intensifier confirms the correct positioning of cement spacer. All wounds are copiously irrigated and closed in layers. An intra-articular knee drain can be used as indicated. The calcaneal pin is removed and a sterile dressing is applied to all skin incisions. In general, operative time for definitive surgery was between 3-4 hours. Postoperatively, the patient is made weight bearing as tolerated immediately and routine perioperative intravenous antibiotics are administered for 24 hours. Patients were monitored on an outpatient basis with serial examination for signs of infection i.e., increased erythema, edema, pain or calor, and wound drainage. If there was a concern for recurrent deep infection, the patient returned to the operating room for repeat debridement with intraoperative cultures taken for confirmation.
4. RESULTS
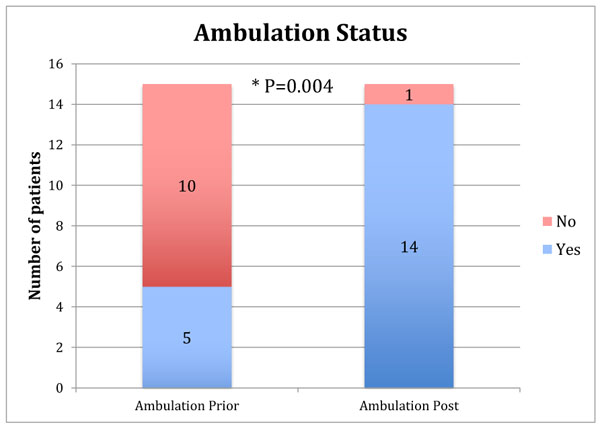
The average age of patients at the time surgery was 68 (range 50-81) years with an average follow-up of 3.2 (range 1-6) years. Patients’ demographic data, co-morbidities, complications, number of previous ipsilateral knee surgeries, and index infection organism are summarized in Appendix 2. Concern for persistent infection upon presentation to the treating surgeon was present in 73% (11/15) of patients who therefore underwent the 2 stage arthrodesis procedure. For the remaining 27% (4/15) of patients, arthrodesis was performed in a single stage. On average, patients had 9 (range 2-30) prior ipsilateral knee procedures. A total of 67% (10/15) of patients were unable to ambulate before arthrodesis. At final follow-up, 93% (14/15) of patients were able to ambulate which was a statistically significant difference (Fig. 2, p=0.004).
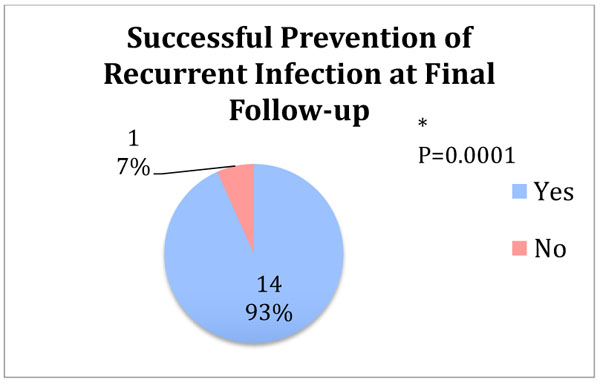
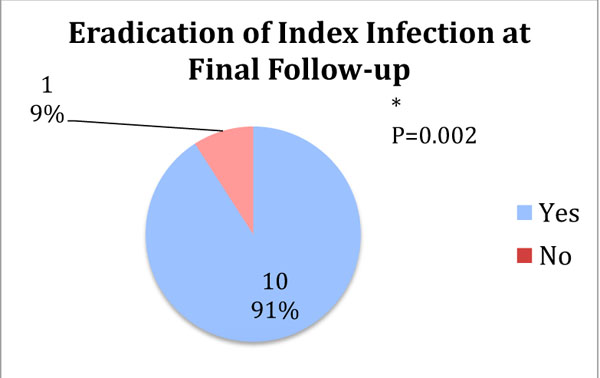
Overall eradication rate of index infection at final follow-up was 93% (14/15) which was a statistically significant difference (Fig. 3, p=0.0001). Amongst the patients that presented to the senior surgeon with an active PJI, 91% (10/11) had their index infection eradicated at final follow-up, without chronic antibiotic suppression (Fig. 4, p=0.002). The overall complication rate was 20% (3/15). Two patients required a return to the operating room for a superficial wound dehiscence that subsequently healed uneventfully after debridement, revision wound closure, and systemic antibiotic administration. One patient ultimately underwent amputation for persistent methicillin-resistant Staphylococcus aureus infection. There were no postoperative periprosthetic hip, femur or tibia fractures. Average SF-12 Physical and Mental scores were 33±7 and 43±8, respectively, at final follow-up.
Anecdotally, 5 out of the 6 patients excluded from analysis returned to ambulation from preoperative immobility with successful prevention or eradication of their index infection. Including these patients, 76% (16/21) were unable to ambulate prior to cement arthrodesis, 90% (19/21) returned to ambulation. 92% (11/12) had eradication of their index infection at final follow-up, and 95% (20/21) had prevention of index infection recurrence, overall.
5. DISCUSSION
Our knee arthrodesis protocol utilizing a custom knee spanning recon nail improves ambulation status in patients with failed TKA. The majority of patients in this study were unable to ambulate upon presentation to our clinic. Almost all patients returned to ambulation at final follow-up. This functional improvement is a fundamental goal of our cement arthrodesis procedure and offers a distinct benefit over above knee amputation, which results in lower rates of ambulation [24]. In addition to improving function, utilization of our protocol successfully prevents or eradicates infection after PJI in the majority of patients. All of our patients had a history of ipsilateral PJI after their primary TKA. Upon presentation to the treating surgeon, there was a concern for persistent infection in most of our study group. . For these patients, a 2-stage strategy was employed. The first stage focused on eradication of infection with thorough debridement and insertion of a static antibiotic eluting spacer to augment systemic antibiotic therapy. These patients underwent definitive arthrodesis when antibiotics were completed for at least 2 weeks and inflammatory markers normalized. A minority of patients with adequate prior debridement and normal inflammatory markers at the time of presentation underwent definitive knee arthrodesis in a single stage. Their PJI was presumed to be adequately treated by the referring surgeon. Overall, utilization of our protocol showed a statistically significant infection eradication and prevention rate. Only one patient with chronic methicillin-resistant Staphylococcus aureus infection had a recurrence of their index infection and required an amputation. Notability, this patient’s arthrodesis procedure was performed in 2 stages given active infection was suspected upon her initial presentation.
On average, patients underwent 9 reconstructive procedures on their knee prior to arthrodesis, with one patient undergoing 30 prior procedures. Such a high number of knee surgeries leads to a combination of significant bone loss, stiffness, and extensor mechanism dysfunction. Once replantation is no longer deemed a reasonable option, the patient is generally faced with a difficult choice to proceed with an above knee amputation or a knee arthrodesis. Considering the results of this study, we recommend a knee arthrodesis for improved function in patients who are medically fit for the procedure.
In addition to improving ambulation and preventing or treating PJI, another clear benefit with respect to our cement arthrodesis technique lies in the fact that it is accomplished utilizing a novel, custom recon nail design with prophylactic fixation into the femoral neck. This presents a significant benefit to the patient, who is often osteoporotic and at increased risk for fragility fractures due to the amount of prior immobilization, lack of activity secondary to the prior bouts of PJI, and multiple prior limb surgeries. To this point, it should be noted that our protocol has successfully prevented postoperative ipsilateral hip, femur or tibia periprosthetic fracture in all patients despite our high-risk geriatric population. Furthermore, the method re-establishes more normal limb lengths, generally avoiding the very cumbersome and embarrassing shoe lifts necessary when traditional arthrodesis is performed with the severe bone loss.
Other groups have described alternative arthrodesis protocols after failed TKA using intramedullary implants [2, 4, 16]. McQueen reported survey results among 32 surgeons who treated 44 total patients with knee arthrodesis after failed TKA with the Wichita Fusion Nail® (Stryker, Kalamazoo, MI, USA) [32]. This system uses a short modular intramedullary nail designed to generate compression across the bony surfaces of the knee and bone graft to promote fusion. Authors report 100% fusion rate with average fusion time of 15.5 weeks and a comparable complication rate of 20%. The design of this particular nail, however, creates a stress riser predisposing to fracture in the diaphysis of the femur and tibia where the nail terminates. The periprosthetic fracture was observed in 2 patients with this implant. Furthermore, active infection and insufficient bone stock are listed as contraindications to using the Wichita Fusion Nail® by the manufacturer. In contrast, our protocol uses an antibiotic eluting cement spacer to address infection and account for the significant bone loss, thereby limiting leg length discrepancy. In another study, Bargiotas introduced a 2-stage arthrodesis technique whereby a ball and socket joint is prepared from the femoral-tibial articulation to increase bleeding bony contact and a long intramedullary rod spans the knee joint. This technique, unlike our protocol, fails to optimize leg length and does not provide fixation in the femoral neck to prevent femoral neck fracture in osteopenic patients.
There are several limitations to this study. First, we report results from a single surgeon with extensive experience with intramedullary fixation. Given the purpose of this study is to introduce our technique, more investigation is warranted to determine the reproducibility of our results amongst other practitioners. Second, a limited number of patients were available for inclusion in this study. There were 6 patients who were deceased or unable to be reached for enrollment and were thus, excluded from statistical analysis. Our results, however, reached statistical significance without including these patients. Third, if active infection remains a concern upon presentation, we strongly recommend a 2-stage protocol whereby the first stage focuses on thorough debridement and placement of a static antibiotic spacer before the definitive procedure. To clarify, our protocol does not technically qualify as an arthrodesis procedure in its traditional definition, given the lack of bony fusion. We employ an intercalary cement spacer to facilitate restoration of limb length and limit the need for shoe lifts. Perhaps the term “pseudofusion” more accurately describes our technique.
CONCLUSION
We introduce a procedure utilizing a long knee spanning recon nail combined with an antibiotic eluting spacer to improve ambulation and prevent or treat recurrent infection in patients with failed TKA secondary to PJI. Our series confirms that this procedure accomplishes these goals in the vast majority of patients.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study has been approved by the Institutional Review Board of University.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this research.
CONSENT FOR PUBLICATION
Patient Informed consent were obtained before research.
CONFLICT OF INTEREST
The authors report no relevant conflict of interests related to this study. There was no funding for this study
ACKNOWLEDGMENTS
We would like to acknowledge Dr. Amy Ladd for providing radiograph of ancient knee fusion.
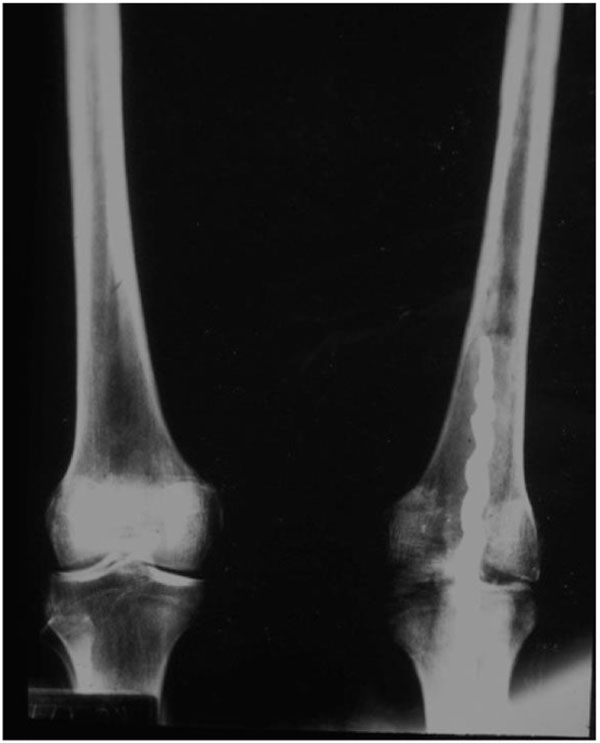
APPENDIX 1
Radiograph of knee arthrodesis in Egyptian mummy ~2000 years old. (Printed with permission from Dr. Amy Ladd, Rosicrucian Museum, San Jose, CA)
APPENDIX 2
Patient Data
| Patient | Age at Surgery | Age Currently | Follow up | Gender | Ambulation Prior | Ambulation Post | Number of Prior Surgeries | BMI | Comorbidities | Charleston Cormorbidity Score (adjusted for age at sux) | Staged | Index Organism | Complications | Complication Notes | Recurrent Deep Infection | Recurrent Infection Organism | SF-12 Physical | SF-12 Mental |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 68 | 69 | 1 | F | n | y | 2 | 27 | Hypertention, Chronic Kidney Disease, Coranary Artery Disease, Asthma | 5 | y | MSSA, ESBL | n | n | 28 | 35 | ||
| 2 | 72 | 74 | 2 | F | n | y | 8 | 38 | Hypertention, Hypothyroidism, Hyperlipidemia, Asthma | 3 | y | Enterobacter Cloacae | y | Superficial wound dehisence, resolved with I&D and systemic antibiotics | n | 40 | 51 | |
| 3 | 64 | 70 | 6 | M | n | y | 14 | 30 | Diabetes Mellitus Type 2, Atrial fibrillation, Hyperlipidemia, Coranary Artery Disease, | 4 | y | MRSA | n | Superficial wound dehisence, resolved with I&D and systemic antibiotics | n | 46 | 49 | |
| 4 | 71 | 74 | 3 | M | y | y | 30 | 32 | Diabetes Mellitus Type 2, Atrial fibrillation, Coronary Artery Disease, Hypertension | 5 | y | Serratia, MRSA | n | n | 27 | 28 | ||
| 5 | 81 | 86 | 2 | M | n | y | 2 | 23 | Tobbaco use | 4 | n | Nocardia | n | n | 32 | 33 | ||
| 6 | 78 | 81 | 3 | F | n | y | 4 | 29 | Hypertension, Parkinson's disease, Depression | 4 | n | MRSA | n | n | 27 | 40 | ||
| 7 | 61 | 65 | 4 | M | y | y | 5 | 39 | Hypertension, Hyperlipidemia, Depression, | 2 | y | MSSA | n | n | 28 | 29 | ||
| 8 | 68 | 82 | 4 | F | y | y | 12 | 25 | Hypertension, Tobbacco Use, Hypothyroidism | 2 | y | Staphylococcus epidermidis | n | n | 34 | 36 | ||
| 9 | 69 | 75 | 6 | F | n | y | 5 | 40 | Diabetes Mellitus Type 1, Hypertension | 4 | n | Pseudomonas aeruginosa | n | n | 36 | 45 | ||
| 10 | 77 | 81 | 4 | M | n | y | 5 | 27 | Diabetes Mellitus Type 2, Coranary Artery Disease, Hypertension, Hyperlipdemia, Gout | 5 | n | Polymicrobial | n | n | 31 | 44 | ||
| 11 | 80 | 85 | 5 | M | y | y | 6 | 35 | Rheumatoid Arthritis, Hypertension, Coronary Artery Disease, Hyperlipidemia | 5 | y | Culture negative | n | n | 28 | 41 | ||
| 12 | 64 | 65 | 1 | F | y | y | 4 | 23 | None | 2 | y | Enterococcus faecali, Staphylococcus epidermidis | n | n | 48 | 52 | ||
| 13 | 58 | 60 | 2 | F | n | y | 7 | 21 | Tobbaco use, Hypertension, Depression | 1 | y | Polymicrobial | n | n | 28 | 52 | ||
| 14 | 50 | 53 | 2 | M | n | y | 17 | 30 | Diabetes Mellitus Type 2, Hypertension | 2 | y | Serratia, Candida albicans | n | n | 40 | 53 | ||
| 15 | 53 | 56 | 3 | F | n | n | 7 | 35 | Chronic MRSA host, Hyperlipidemia, Hypertension | 1 | y | MRSA (chronic carrier) | Y | Persistant infection requiring amputation | Y | MRSA | 22 | 52 |
| Mean | 67.60 | 72.86 | 3.21 | - | - | - | 8.53 | 30.27 | - | 3.27 | - | - | - | - | - | - | 33.00 | 42.67 |
| SD | 9.44 | 9.80 | 1.67 | - | - | - | 7.32 | 6.10 | - | 1.49 | - | - | - | - | - | - | 7.56 | 8.84 |
| Range | 50-81 years | 53-85 years | 1-6 years | - | - | - | 2-30 surgeries | 21-40 | - | 1-5 | - | - | - | - | - | - | 27-48 | 29-53 |
| Patient | Age at surgery | Age currently | Follow up | Gender | Ambulation Prior |
|---|---|---|---|---|---|
| 1 | 68 | 69 | 1 | F | n |
| 2 | 72 | 74 | 2 | F | n |
| 3 | 64 | 70 | 6 | M | n |
| 4 | 71 | 74 | 3 | M | y |
| 5 | 81 | 86 | 2 | M | n |
| 6 | 78 | 81 | 3 | F | n |
| 7 | 61 | 65 | 4 | M | y |
| 8 | 68 | 82 | 13 | F | y |
| 9 | 69 | 75 | 6 | F | n |
| 10 | 77 | 81 | 4 | M | n |
| 11 | 80 | 85 | 5 | M | y |
| 12 | 64 | 65 | 1 | F | y |
| 13 | 58 | 60 | 2 | F | n |
| 14 | 50 | 53 | 2 | M | n |
| 15 | 53 | 56 | 3 | F | n |
| Mean | 67.60 | 72.86 | 3.86 | - | - |
| SD | 9.44 | 9.80 | 3.11 | - | - |
| Range | 50-81 years | 53-85 years | 1-13 years | - | - |
| Ambulation Post | Number of prior surgeries | BMI |
|---|---|---|
| y | 2 | 27 |
| y | 8 | 38 |
| y | 14 | 30 |
| y | 30 | 32 |
| y | 2 | 23 |
| y | 4 | 29 |
| y | 5 | 39 |
| y | 12 | 25 |
| y | 5 | 40 |
| y | 5 | 27 |
| y | 6 | 35 |
| y | 4 | 23 |
| y | 7 | 21 |
| y | 17 | 30 |
| n | 7 | 35 |
| 8.53 | 30.27 | |
| 7.32 | 6.10 | |
| 2-30 surgeries | 21-40 |
| Charleston Comorbidity Score (adjusted for age at sx) | Staged | Index Organism | Complications |
|---|---|---|---|
| 5 | y | MSSA, ESBL | n |
| 3 | y | Enterobacter Cloacae | y |
| 4 | y | MRSA | y |
| 5 | y | Serratia, MRSA | n |
| 4 | n | Nocardia | n |
| 4 | n | MRSA | n |
| 2 | y | MSSA | n |
| 2 | y | Staphylococcus epidermidis | n |
| 4 | n | Pseudomonas aeruginosa | n |
| 5 | n | Polymicrobial | n |
| 5 | y | Culture negative | n |
| 2 | y | Enterococcus faecalis, Staphylococcus epidermidis | n |
| 1 | y | Polymicrobial | n |
| 2 | y | Serratia, Candida albicans | n |
| 1 | y | MRSA (chronic carrier) | y |
| 3.27 | |||
| 1.49 | |||
| 1-5 |
| Complication notes | Recurrent deep infection | Recurrent infection organism |
|---|---|---|
| n | ||
| Superficial wound dehiscence, resolved with I&D and systemic antibiotics | n | |
| Superficial wound dehiscence, resolved with I&D and systemic antibiotics | n | |
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| n | ||
| Persistent infection requiring amputation | y | MRSA |
| SF-12 Physical | SF-12 Mental |
|---|---|
| 28 | 35 |
| 40 | 51 |
| 46 | 49 |
| 27 | 28 |
| 32 | 33 |
| 27 | 40 |
| 28 | 29 |
| 34 | 36 |
| 36 | 45 |
| 31 | 44 |
| 28 | 41 |
| 48 | 52 |
| 28 | 52 |
| 40 | 53 |
| 22 | 52 |
| 33.00 | 42.67 |
| 7.56 | 8.84 |
| 27-48 | 29-53 |


