All published articles of this journal are available on ScienceDirect.
Timing of Femoral Shaft Fracture Fixation Affects Length of Hospital Stay in Patients with Multiple Injuries
Abstract
Purpose :
Appropriate timing of definitive fracture care in the setting of polytrauma remains controversial. The aim of this study is to determine whether timing of definitive fixation of femur fractures impacts subsequent length of hospital stay, a surrogate for postoperative morbidity, in patients with multi-system trauma.
Methods :
Secondary analysis of data from the National Trauma Data Bank (January 1, 2000 to December 31, 2004) was performed. Adult patients who: (1) had an open or closed femoral shaft fracture, (2) had an injury severity score (ISS) greater than or equal to 15, (3) and underwent definitive internal fixation were included. Time to fixation was divided into 5 time periods based on commonly used cut-off points from the literature: (1) 12 hours or less, (2) between 12 and 24 hours, (3) between 24 and 48 hours, (4) between 48 and 120 hours, and (5) more than 120 hours. Because we consider length of stay a surrogate for adverse outcome causally affected by treatment time, the outcome variable was calculated as the duration of hospitalization following definitive treatment. Time to definitive fixation and its effect on post-treatment length of hospital stay was analyzed using median regression with inverse probability of treatment-weighting (IPTW) to control for confounding factors.
Results :
Compared to fixation during the first 12 hours after admission, median length of hospital stay was significantly higher (2.77 days; 95% confidence interval, 0.54 to 4.72) when fixation occurred between 48 and 120 hours from admission. Among the other time intervals, only treatment between twelve to twenty-four hours after admission was shown to reduce length of stay (-0.61 days; 95% confidence interval, -1.53 to 0.42) versus the referent interval of the first 12 hours, though this result did not achieve statistical significance. In order to assess the impact of shorter recorded length of stay for deceased patients, sensitivity analysis was conducted excluding all patient that underwent definitive treatment and died. Results were nearly identical for the second analysis, showing a higher post-treatment length of stay estimated for the population treated between 48 and 120 hours versus had they been treated within the first 12 hours from admission (2.53 days, 95% confidence interval, 0.27 to 4.13).
Conclusion :
Delayed fixation of femoral shaft fractures in patients with multiple injuries between 2-5 days may lead to an increase in adverse outcomes as evidenced by increased median length of hospital stay. This finding supports prior clinical reports of a perilous period where a “second hit” resulting from definitive internal fixation can occur. Whether there is an optimal window for fixation during which physiologic stress of fracture fixation does not adversely lengthen hospital stay should be the subject of future prospective study.
INTRODUCTION
Although the literature supports early isolated femoral fracture fixation [1-11], conflicting studies leave the optimal timing of long-bone fracture fixation in patients with multisystem trauma a controversial subject. The debate over the optimal timing of fixation weighs the benefits of early stabilization against the potential detrimental effects of an operation that may precipitate decompensation in an acutely injured and incompletely resuscitated patient [12]. Several [13-15] observational studies and one randomized study have suggested that early stabilization of major long bone fractures, especially those of the femoral shaft, is associated with the clinical benefits of reducing the incidence of pulmonary complications and mortality. However, other studies have suggested that early internal fixation of long-bone fractures, either with intramedullary nailing or plate osteosynthesis, introduces factors such as hypoperfusion [16] and inflammation [5, 8, 9] which may predispose the patient to end-organ injury and morbidity. A meta-analysis [11] reported that early operative fixation complications (usually within twenty-four hours) was associated with a large relative risk reduction (relative risk, 0.30; 90% confidence interval, 0.22 to 0.40) in respiratory complications, whereas two systematic reviews [4, 10] reported that early operative treatment (usually within twenty-four hours) and late operative treatment of femoral shaft fractures show no difference in morbidity or mortality, either overall or within subgroups of patients with associated head injuries or thoracic injuries. These inconsistent findings have left clinicians uncertain about what effect timing of definitive fracture care has on adverse outcomes. Differences in treatment definition (regarding time cutoffs and method of fixation), inadequate population sampling and control of confounding variables all serve to limit the validity and generalizability of previous findings. Despite the attention this topic has received, there have been no published studies to-date on the effect of early definitive fixation of femoral shaft fractures on the length of hospital stay for patients with multisystem trauma. The current study addresses the impact of timing of definitive fixation on the length of hospital stay with use of a multilevel definition of treatment time drawn from the largest available multi-center database of patients with multisystem trauma (the National Trauma Data Bank).
MATERIALS AND METHODS
We identified our study cohort with use of the National Trauma Data Bank (version 5.0), which draws from 567 trauma centers from around the United States [1] and contains nearly one million incident trauma cases that occurred over the five-year period between January 1, 2000, and December 31, 2004. The National Trauma Data Bank contains pre-hospitalization and hospitalization information compiled from medical records during admission (including injury characteristics, comorbidities, inpatient treatments, and outcomes), which are submitted to the American College of Surgeons for quality control and maintenance.
The inclusion criteria for patients in our study sample were that they (1) had a closed or open fracture (or fractures) of the femoral shaft as identified by an International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) diagnostic code of 821.0 (fracture of femoral shaft/not otherwise specified— closed), 821.01 (fracture of femoral shaft—closed), 821.1 (fracture of femoral shaft/not otherwise specified—open), or 821.11 (fracture of femoral shaft—open); (2) had an International Classification of Diseases-derived Injury Severity Score [2, 6] of at least 15; (3) were at least sixteen years old; and (4) underwent internal fixation as a definitive treatment of the femoral shaft fracture as identified by an ICD-9-CM procedure code of 78.55 (internal fixation—femur), 79.15 (closed reduction and internal fixation—femur), or 79.35 (open reduction and internal fixation—femur). Our exclusion criteria removed a patient from the study sample if (1) the patient was transferred in or was not admitted on the day of injury; (2) there was inadequate information in the record on the time from admission to definitive fracture fixation, mortality status, or length of hospitalization; (3) the patient had a negative post-operative length of stay; or (4) the patient did not undergo a definitive procedure for fixation of the fracture within two weeks after admission.
Due to the inherent potential of selection bias in an observational study, we only included subjects with all information regarding possible confounding covariates. An a priori list of baseline covariates accessible in the National Trauma Data Bank 5.0 was created based on the literature and clinical suspicion as potential confounders of the association between time of treatment and length of hospital stay. These covariates included age, sex, race, maximum Abbreviated Injury Score [6] for each of the six anatomic regions (head/neck, face, chest, abdomen, extremity/pelvis, and skin), New Injury Severity Score [3, 7], Glasgow Coma Scale score on arrival, first systolic blood pressure, blunt or penetrating trauma, the type of femoral fracture (open or closed), the number of femoral fractures, the number of serious extremity/pelvic injuries (Abbreviated Injury Score, >3), the presence of alcohol or drugs in the bloodstream at the time of admission, the year of the incident, the time of arrival at the hospital (day divided into four quarters), the modified Charlson comorbidity index [17], and the presence or history of specific comorbidities (coronary artery disease, including heart failure; chronic obstructive pulmonary disease; stroke; hematologic disease, including coagulopathy; diabetes; pregnancy; or hepatorenal disease or failure) at the time of admission. Features of the hospitals included were the mean number of femoral shaft fractures admitted to the treating facility per year, teaching status, type of facility (public or private), American College of Surgeons trauma center level, and geographic region of the United States (Northeast, Midwest, South, West). We then identified a subset of these covariates (Wl) associated with length of stay (p < 0.2) with use of appropriate nonparametric bivariate tests of association, adjusted for multiple testing with the Benjamini-Hochberg procedure [18], and excluding observations with missing values in Wl, in order to obtain a final sample with complete data in all measured potentially confounding covariates for analysis.
Treatment Variables
We studied the effect of timing of definitive treatment of femoral shaft fracture on length of hospitalization. Rather than using a simple dichotomy at twelve or twenty-four hours, we provided more clinically relevant categories with five time periods based on commonly used cut-points from the literature [10-12]: t0 (twelve hours or less), t1 (between twelve hours and twenty-four hours), t2 (between twenty-four hours and forty- eight hours), t3 (between forty-eight hours and 120 hours), and t4 (after 120 hours). While previous studies typically regard twenty-four hours as the most commonly used threshold before which “early” treatment, we defined our referent group (t0) as treatment within the first twelve hours in order to represent those subjects who were most likely to have been inadequately resuscitated and in a state of occult hypoperfusion [16, 19]. We hypothesize that additional physiologic stress from definitive fracture surgery in such patients could activate an adverse systemic response leading to end-organ injury, multiple organ failure, longer length of stay, and excess mortality compared to findings in patients managed later, when adequate resuscitation is more likely to have been achieved.
Each procedure in the dataset is recorded with a number of days, hours, and minutes after admission when it was performed. Using this information, we calculated the time from admission to definitive fracture fixation, as defined above with use of ICD-9-CM procedure codes. By excluding patients who were transferred from other facilities or were admitted one or more days after the injury, we assumed that the calculated treatment time level was a reliable surrogate for the time from the injury, underestimating the true elapsed time only by the time required to reach the hospital.
Main Outcome Measure
Length of post-operative hospitalization was our sole outcome of interest. While other studies of treatment time effect have focused on the diagnosis of acute respiratory distress syndrome (ARDS) or multiple-organ failure, the reporting of such outcomes is inherently subjective and prone to measurement error [20]. In the absence of patient-centered outcomes (i.e., health-related quality of life) and systematic assessment of morbid events after treatment, mortality is the most objective, and therefore likely valid, end point. Despite this, mortality may potentially lack sensitivity in the detection of morbid consequences of treatment. While potentially positively skewed [21, 22] and therefore difficult to analyze, length of hospital stay remains an accurate measure of immediate post-operative outcomes.
Statistical Methods
The differences in length of stay was estimated among the 5 possible treatment groups using median regression [22] while confounding bias was adjusted for using inverse probability of treatment-weighting of the sample [23]. This method uses the reciprocal of the conditional probability of a subject receiving an assigned treatment given other covariates as a means of confounding control in order to determine the effect of treatment. Unlike propensity score analysis [24, 25], inverse probability of treatment-weighted analysis can easily be adapted for use with multilevel categorical treatment assignment. The likelihood of treatment within one of the five time categories was estimated with use of data-adaptive model selection [26], and goodness-of-fit of the model was assessed with use of the Hosmer-Le Cessie test [27]. We were also interested in the potential for differences of treatment effect for different subgroups defined by the severity of associated head or neck, chest, abdominal, or additional extremity/pelvic injury. Therefore, we tested the hypothesis that patients with serious injuries (defined as an Abbreviated Injury Score [28] of greater than or equal to 3) in any one of these four anatomic regions would have a greater relative risk reduction with fixation delayed beyond the first twelve hours of hospitalization than those without such associated injuries.
Confidence intervals and p-values were non-parametrically obtained with use of a modified bootstrap approach [29, 30] that takes into account correlations between patients managed at the same hospital. The level of significance was set at p < 0.05. We tested for effect modification by obtaining bootstrap-based p values for the hypothesis that the relative risk of longer length of hospitalization associated with treatment time is identical for both levels (not serious and serious) defined by each of the four potential associated body regions injured. Because interactions of this kind are difficult to identify, the level at which significance was considered was relaxed to p < 0.2. All analyses were carried out with R software (version 2.3.1) [31, 32].
RESULTS
Fig. (1) illustrates the selection process of the study sample of 2,949 subjects from 3,506 polytrauma patients undergoing definitive femoral fixation. The average age was 32.9 (SD 14.8) years, and 2120 patients (71.9%) were men. More than half of the patients (n= 1685) were treated within 12 hours after admission, with decreasing numbers treated in each subsequent time period (Table 1). The group of patients treated between twelve and twenty-four hours (8.5 days; 95% confidence interval, 8.0 to 9.3) had the lowest crude median length of stay compared to those who were managed earlier or later. The Glasgow Coma Scale score, New Injury Severity score, Maximum Abbreviated Injury score in the head or neck region, cardiac comorbidity, and number of serious associated extremity injuries were strongly associated (p<0.001) with both Length of Stay and treatment, with a consistent trend toward more severe injury among patients who were managed later. The most common serious associated injuries, by body region, were closed C2 fracture, pulmonary contusion, lumbar vertebral fracture, and intertro-chanteric fracture. The most common serious associated injuries, by body region, were closed C2 fracture, pulmonary contusion, lumbar vertebral fracture, and intertrochanteric fracture. The in-hospital mortality over all treatment periods was 3.53%.
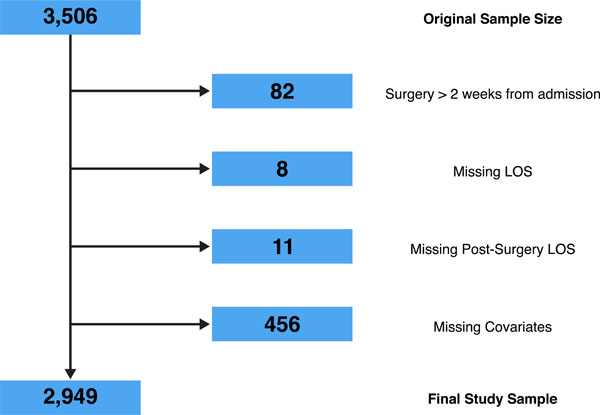
Study sample inclusion flow chart from the National Trauma Data Bank version 5.0 (2000 through 2004) (NTDB 5.0 Cohort). ISS = Injury Severity Score. Wl= covariates associated with length of stay (p < 0.2). LOS: Length of Stay.
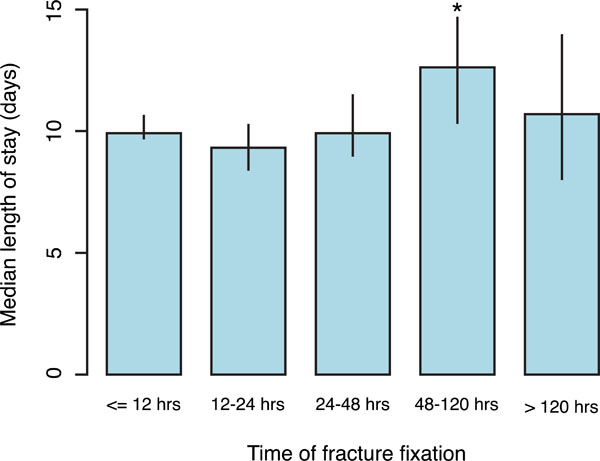
Inverse probability of treatment-weighted length of stay estimates, with 95% confidence intervals (lines). An asterisk (*) represents significant adjusted median difference in length of stay (p<0.05) versus the referent group (t0 - less than or equal to 12 hours from admission).
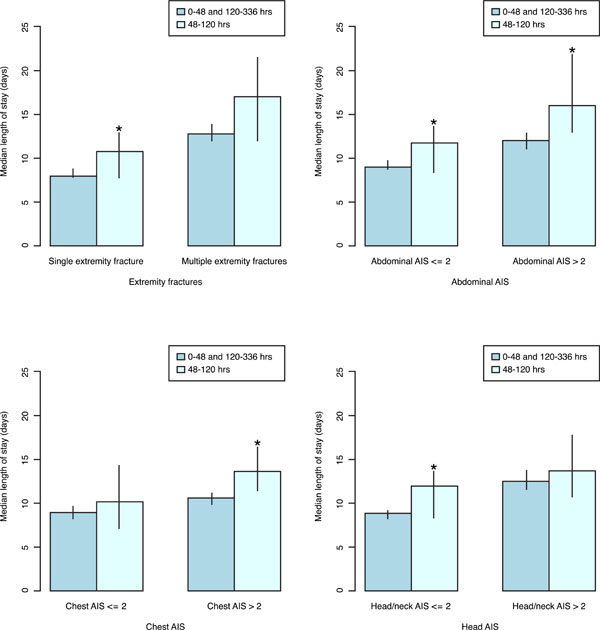
Inverse probability of treatment-weighted length of stay estimates, stratified according to the severity of associated injury (presence of serious associated extremity/pelvis, abdominal, chest, and head or neck injury), with 95% confidence intervals (lines). An asterisk (*) represents significant adjusted median difference in length of stay (p<0.05) for the 48 to 120 hour treatment group versus the combined treatment groups of 0 to 48 hours and greater than 120 hours. AIS = Abbreviated Injury Score.
Summary table of bivariate associations of covariates with length of stay and treatment group.
| Treatment Group Means and Proportions (± SD)* | P Value | ||||||
|---|---|---|---|---|---|---|---|
| t0 (n=1685)* | t1 (n=518)* | t2 (n=347)* | t3 (n=263)* | t4 (n=136)* | Association with Treatment |
Association with Length of Stay |
|
| Covariates | |||||||
| Glasgow Coma Severity Scale | 12.68 ±4.21 | 12.70±4.11 | 11.86±4.61 | 10.86±5.08 | 9.83 ± 5.16 | <0.001 | <0.001 |
| New Injury Severity Score | 27.3 ± 8.95 | 27.2 ±8.43 | 29.2 ±9.68 | 32.4±11.52 | 34.6 ±14.03 | <0.001 | <0.001 |
| Maximum Abbreviated Injury Score, head/neck region |
1.71 ± 1.65 | 1.76 ±1.69 | 2.01 ±1.68 | 2.32 ±1.83 | 2.50 ±1.94 | <0.001 | <0.001 |
| Cardiac comorbidity | 0.13 ± 0.34 | 0.17 ±0.37 | 0.20 ±0.40 | 0.28 ±0.45 | 0.27 ±0.45 | <0.001 | <0.001 |
| Number of serious associated extremity injuries |
1.64 ± 0.94 | 1.39 ±0.71 | 1.50 ±0.79 | 1.67 ±1.01 | 1.68 ±0.96 | <0.001 | <0.001 |
| Arrival between 6AM and 12 PM | 0.24 ± 0.43 | 0.07 ±0.26 | 0.20 +0.40 | 0.18 ±0.39 | 0.22 ±0.42 | 0.001 | 0.03 |
| Age | 31.9 ± 13.7 | 32.7 ±15.8 | 34.2 ±15.9 | 34.5 ±16.4 | 33.4 ±15.1 | 0.01 | <0.001 |
| Bilateral fracture | 0.02 ± 0.14 | 0.00 ±0.06 | 0.01 ±0.12 | 0.02 ±0.12 | 0.02 ±0.15 | 0.03 | 0.001 |
| Teaching hospital | 0.56 ± 0.50 | 0.67 ±0.47 | 0.58 ±0.50 | 0.53 ±0.50 | 0.63 ±0.49 | 0.38 | 0.02 |
| Hospitals from Northeast region | 0.08 ± 0.27 | 0.10 ±0.30 | 0.09 ±0.29 | 0.11 ±0.32 | 0.07 ±0.26 | 0.54 | 0.07 |
| Treated at level-1 trauma center | 0.39 ± 0.49 | 0.39 ±0.49 | 0.45 ±0.50 | 0.45 ±0.50 | 0.48 ±0.50 | 0.69 | 0.07 |
| Cerebrovascular comorbidity | 0.00 ± 0.04 | 0.00 ±0.04 | 0.01 ±0.08 | 0.00 ±0.06 | 0.00 ±0.00 | 0.74 | 0.7 |
| Unadjusted Median Length of Stay** |
9.8 (9.0,10.0) | 8.5 (8.0,9.3) | 10.1 (9.0,11.3) | 14.7 (12.8,17.1) | 14.0 (12.1,18.4) | ||
* Means and proportions (+ SD).
** Median (+ 95% confidence interval).
Unadjusted and adjusted estimates of effect of treatment time on median difference in length of Stay.
| Estimate | >12 to 24 Hr* | >24 to 48 Hr* | >48 to 120Hr* | >120 Hr* |
|---|---|---|---|---|
| Unadjusted Difference* | ||||
| Point estimate | -1.33 (-1.82, -0.42) | 0.30 (-0.69, 1.73) | 4.91 (3.10, 7.40) | 4.19 (2.26, 8.58) |
| P-value | 0.0149 | 0.562 | 0.0001 | 0.0353 |
| IPTW Difference | ||||
| Point estimate | -0.61 (-1.53, 0.42) | -0.00 (-1.00, 1.47) | 2.77 (0.54, 4.72) | 0.86 (-2.00, 4.15) |
| P-value | 0.2949 | 0.9984 | 0.0080 | 0.7351 |
| IPTW Difference Deaths excluded | ||||
| Point estimate | -0.64 (-1.53, 0.3.8) | 0.24 (-0.96, 1.61) | 2.53 (0.27, 4.13) | 0.55 (-2.04, 4.08) |
| P-value | 0.2949 | 0.6346 | 0.0167 | 0.7674 |
| IPTW Difference Death imputed to 220 days | ||||
| Point estimate | -1.18 (-1.53, 0.38) | 0.33 (-0.91, 2.00) | 2.28 (0.28, 4.42) | 0.18 (-2.63, 4.00) |
| P-value | 0.1261 | 0.6708 | 0.0317 | 0.8899 |
IPTW: Increased Probability Treatment Weighted.
With the possible exception of the >120-hour (t4) time frame, the Hosmer-Le Cessie test showed acceptable fit of the selected treatment model (p values for goodness-of-fit: 0.65, 0.47, 0.78, and 0.025, respectively.
*Estimates of effect use the early treatment group (t0) as the referent for comparison, with statistical adjustment performed through inverse probability of treatment weighted analysis using a treatment model incorporating the following covariates: hospital arrival time, New Injury Severity Score, cardiovascular disease, cerebrovascular disease, number of severe (AIS > 3) extremity injuries, age, maximum head region AIS, teaching status of treating facility, Glasgow Coma Score, trauma center designation.
Inverse probability of treatment.
| Low Severity (AIS < 3) | High Severity (AIS > 3) | P-Value* | |||
|---|---|---|---|---|---|
| Median Difference in Length of Stay (95% Confidence Interval) |
N | Median Difference in Length of Stay (95% Confidence interval) |
N | ||
| Fractures | 2.77(-0.26,4.72) | 1785 | 4.21(-0.76,8.80) | 1164 | 0.585 |
| Abdominal AIS | 2.69(-0.49,4.14) | 2177 | 4.00 (1.00,9.59) | 772 | 0.526 |
| Chest AIS | 1.27(-1.86,5.38) | 1332 | 3.05 (1.00,5.96) | 1617 | 0.4835 |
| Head AIS | 3.14(-0.48,4.89) | 1846 | 1.19(-1.88,5.13) | 1103 | 0.395 |
AIS= Abbreviated Injury Score. *The p values test the equality of treatment effects between low and high-severity associated injury subgroups.
The estimated median length of stay if all subjects had been managed during each one of the five time periods is shown in Fig. (2), controlling for measured confounders. Median length of stay was estimated to be highest if all subjects were managed between forty-eight and 120 hours after admission, and 2.77 days longer (95% CI: 0.54-4.72) than patients treated within 12 hours of admission (the largest group chosen to serve as the referent, Table 3). There is some suggestion that treatment between 12 and 24 hours after admission may lead to a reduction in median length of stay (-0.61 days; 95% CI: -1.53 to 0.42). While this reduction did not reach statistical significance it, like the increased length of stay associated with treatment between 48 and 120, was consistently estimated in the sensitivity analyses reported below.
Since surgery between forty-eight and 120 hours is estimated to lead to a lower mortality risk than surgery within 12 hours [33], we tested whether lower mortality in this time period could have resulted in more survivors that would drive up the average length of stay. This was done by repeating our analysis among the 2844 subjects who did not die after surgery, which resulted in a similar statistically significant increase of 2.53 days (95% CI: 0.27 to 4.13) in the median length of stay for surgery between forty-eight and 120 hours versus the early referent group (Table 2). The second form of sensitivity analysis considers that mortality must be considered the worst possible outcome. The recorded hospital stay in such instances may be considerably shorter than the patients who survived their surgery. In order to adequately reflect a patient’s death as the worst possible outcome of surgery, the patients who died were assigned a the maximum length of stay in our study, 222 days. The results of an IPTW analysis based on this outcome, summarized in Table 2 show a statistically significant increase of 2.28 days (95% CI: 0.28 to 4.42) in the median length of stay for surgery between forty-eight and 120 hours versus the early referent group.
These results support the hypothesis that surgery between forty-eight and 120 hours after admission leads to worse clinical outcomes than surgery at other times. In an effort to identify subpopulations of patients that experience particularly strong increases in length of stay if surgery is performed between 48 and 120 hours after admission, we consider a dichotomized version of treatment time that compares surgery between 48 and 120 hours to surgery at any other time. For all patients, surgery between 48 and 120 hours is estimated to increase the median length of stay by 2.50 days (95%CI: 0.37 to 4.35; p-value: 0.015). Table 3 summarizes the median change estimates within groups defined the number of extremity fractures as well as by severe abdomen, chest, and head injury. Fig. (3) shows the corresponding estimated median lengths of stay. Despite suggestions that more severely injured patients experience an increased length of stay if treated between forty-eight and 120 hours after admission, the results were not significant for modification of the effect of treatment time by presence of these associated injuries.
DISCUSSION
We conducted an analysis of the importance of timing of definitive fixation of femoral shaft fracture among subjects with multisystem trauma in the National Trauma Data Bank. Using an inverse probability of treatment-weighted analysis to adjust for differences in case mix among patients treated at categorically defined time intervals following admission, we found that treatment delay of forty-eight to 120 hours after admission resulted in a significant increase in length of stay versus treatment within 12 hours or any other time within two weeks admission. These findings strongly endorse a careful approach to the timing of definitive femoral shaft fracture fixation among patients with multisystem trauma, and specifically avoiding the forty eight to 120 hour period from admission as a particularly high risk time for major orthopaedic intervention like definitive femoral fixation.
Brundage et al. [12] assembled a large single center cohort with multisystem trauma (ISS > 15) and femoral shaft fracture with comparable demographics, associated injuries, and crude mortality rates to our sample from the NTDB. They studied the effect of timing of definitive fixation of femoral shaft fractures controlling for measured confounders and discovered a significant increase in mean length of stay for patients treated from forty-eight to 120 hours after admission compared to all other treatment groups, especially among patients with chest trauma (AIS > 2). They reported significant increases in respiratory complications like pneumonia and acute respiratory distress syndrome among patients who were treated between two and five days after the injury, potentially explained these patients’ longer stays though time to surgery was not subtracted from length of stay as it was in our study. Brundage et al. also found patients treated within 24 hours to have the shortest length of stay. We split the first 24 hours at the hospital into two periods and found that there may be a protective effect from delaying fixation even if only by twelve hours. Although this finding failed to achieve statistical significance, the short delay may provide time for some level of resuscitation thereby reducing complications and improving outcomes.
Pape et al. [34] reported on a cohort of 128 polytrauma patients with femoral shaft fractures (Injury Severity Score >18). Definitive fixation of femoral fractures between 2 and 4 days after injury was associated with higher IL-6 levels and higher rates of multi-organ dysfunction than among those treated between 5 and 8 days post injury (47% versus 16%, p-0.01). While neither this study nor that of Brundage et al. demonstrated a higher mortality within the 2 to 5 day window following injury, both demonstrated notably higher morbidity consistent with our findings. Moreover, unlike those previous studies, we were able show that the 2 to 3 day median increase in length of stay associated with definitive femoral fixation in the 2 to 5 day window was not sensitive to the hospital stays of those patients who died after definitive fixation.
Numerous studies have supported the notion that there are particular subgroups of polytrauma patients defined by severe associated head [35-37], chest [38, 39] or abdominal [33] injuries whose survival or morbidity experience may be particularly sensitive to timing of fixation. However, this subject of effect or treatment time modification by associated injuries is debated with contradictory evidence suggesting that in many case, it is the severity of that particularly associated injury that dictates post-treatment morbidity and mortality more than the type of fixation or timing. Stratified analysis by presence of associated severe head, chest, abdomen or additional extremity injury demonstrated consistency of median increase in length of stay inside of the 48 to 120 hour window among all subgroups. However, none of these associated severe injuries disposed patients to significantly more or less benefit from femoral fixation outside of this treatment interval.
Early treatment (t0) in our study likely represents treatment of subjects in an under-resuscitated state when they were prone to excess mortality [40-43], but not longer lengths of stay. In a study by Crowl and colleagues [16] of femoral shaft fracture patients with multisystem trauma,, early intramedullary fixation of femoral shaft fracture (less than twenty-four hours after admission) in the setting of occult hypoperfusion (serum lactate, > 2.5 mmol/L) was associated with a significant increase in postoperative complications. Hypoperfusion resulting from trauma may prime the immune system for an inflammatory response leading to end-organ damage if adequate resuscitation is not achieved prior to performing such treatment [44, 45]. The realization of this phenomenon has led to the description of so-called “damage-control orthopaedics”, whereby definitive treatment is delayed until resuscitation of the patient has been adequately achieved [5, 38, 46, 47]. O’Toole et al. [48] were able to adequately resuscitate (arterial lactate of 2.5mmol/L or less) and definitively fixate femurs in 88% of patients presenting to a single trauma center within 24 hours of admission with low rates of ARDS (1.5%) and mortality (2.0%). Our findings are consistent with this approach and indicate the likely benefits that may be achieved with delays in operative femoral fracture fixation of just twelve hours that allow for adequate resuscitation, but before the perilous window of 48 to 120 hours when patients may be parti-cularly disposed to a “second hit” and systemic inflam-matory response.
The retrospective observational nature of the present study prevents attributing a causal effect to the timing of treatment. Unmeasured confounding factors such as time from sustaining the injury to hospital admission may bias estimates of the effect of treatment time. Moreover, excluding otherwise eligible subjects from the sample study (Fig. 1) due to missing information on measured covariates may have introduced selection bias. While the National Trauma Data Bank includes a very large sample of trauma centers from all over the United States, it is a convenience sample. Still, this is the largest and most nationally representative cohort used for investigation of this study question, allowing for extensive generalizability of these results. The National Trauma Data Bank data provided extensive covariate information, which was used for comprehensive covariate adjustment, and robust analytical methods were used to optimize model fit and to properly estimate confidence intervals in the setting of potential correlations by treatment center. The discrepancy between crude and adjusted estimates (Table 2), in light of more severe injury and higher mortality in the later treatment groups (Table 1), demonstrates the degree to which confounding by disease severity may threaten valid inferences in studies similar to ours. We employed statistically efficient analytical methods to address this bias, and these methods provided unconditional estimates of median difference in length of hospital stay.
CONCLUSION
In conclusion, we have conducted an observational study assessing how the timing of definitive fixation of femoral shaft fracture in patients with multisystem trauma affects hospital length of stay. We estimate a 2 to 3 day increase in the median length of stay when treatment occurs between forty-eight and 120 hours after admission; a non-significant reduction is estimated when treatment occurs between twelve and twenty-four hours. These results provide strong empirical evidence in support of a delayed or “damage-control” approach to definitive fixation of femoral shaft fracture among multisystem trauma patients. Our findings suggest that patients who are not adequately resuscitated by their 2nd hospital day should likely not undergo definitive femoral fixation until the fifth hospital day as this period corresponds to peaking of systemic inflammatory response and susceptibility to “second hit” from a major surgical intervention. In the future, better measures of systemic inflammation and hypoperfusion will guide more rational decision-making on the optimal timing of major orthopaedic procedures in multisystem trauma patients. While a randomized controlled trial is needed to prove the treatment effects estimated here, debate is necessary to further define a population in which such a trial would be ethical.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.
DISCLOSURE
“Part of this article has already been published in J Bone Joint Surg Am, 2009 Jan 01; 91 (1): 3-13. http://dx.doi.org/ 10.2106/JBJS.H.00338”.


