All published articles of this journal are available on ScienceDirect.
Negative Pressure Wound Therapy – A Review of its Uses in Orthopaedic Trauma
Abstract
The use of Negative Pressure Wound Therapy (NPWT) for complex and large wounds has increased in popularity over the past decade. Modern NPWT systems consisting of an open pore foam sponge, adhesive dressing and a vacuum pump producing negative pressure have been used as an adjunct to surgical debridement to treat tissue defects around open fractures and chronic, contaminated wounds. Other uses include supporting skin grafts and protecting wounds at risk of breaking down. This review outlines the current and emerging indications for negative pressure wound therapy in Orthopaedic trauma and the existing preclinical and clinical evidence base for its use.
INTRODUCTION
The use of Negative Pressure Wound Therapy (NPWT), most commonly provided with the Vacuum Assisted Closure (V.A.C. KCI, TX, USA) system using a sealed open-pore sponge or gauze, is now common place within orthopaedic and trauma departments. Since their introduction, 18 years ago, modern NPWT systems have enjoyed an increasing popularity, despite a comparative paucity of reliable clinical evidence. More recently, randomised controlled trials and larger studies have been published studying the clinical benefits of NPWT in orthopaedic trauma setting. This allows clinicians such as those in the International Negative Pressure Wound Therapy Expert Panel (NPWT-EP), who have met annually since 2009, to establish an international consensus that allows the formulation of clinical guidelines.
MECHANISM OF ACTION
The advent of modern NPWT systems is attributed to Argentas and Morykwas [1, 2], who developed several prototypes to facilitate wound healing by distributing suction across wounds to help draw the skin edges together. They developed a system, whereby, an open-pore polyurethane foam sponge was placed within a wound, covered by a semi-occlusive dressing and then connected to a device producing suction. NPWT facilitates wound healing through multiple mechanisms of action both at the macroscopic and microscopic level [3, 4]. The primary mechanisms of action include:
- Macrodeformation of the wound when, depending on the deformability of the surrounding tissues, the wound edges are brought closer together by the suction distributed through the foam sponge. This reduces the space required to be healed by primary closure or secondary granulation (see Fig. 1).
- Microdeformation of the wound surface at the microscopic level. Finite element computer models have shown that NPWT produces 5-20% strain across the healing tissues, that promotes cell division and proliferation, growth factor production and angiogenesis [5].
- Extraction of oedematous fluid and exudate from the extracellular space, removing inflammatory mediators and cytokines whose prolonged effect can hinder the ability of the microcirculation to support damaged tissue. This can lead to further tissue necrosis frequently seen at further debridement.
- A warm and moist environment that prevents desiccation of the wound and enhances formation of granulation tissue [6] (see Fig. 1).

NPWT dressings can bring wound edges closer together and promote the production of granulation tissue in large wounds.
COMPONENTS OF A NPWT SYSTEM
There are a number of systems now available on the market. They all share a similar design with a base unit pump to provide negative pressure, a canister to collect wound drainage, and a segment of tubing connecting this to the sealed wound. The NPWT device works by providing and distributing negative pressure evenly across the wound bed either through the application of an open cell foam or a gauze dressing [7]. Both foam and gauze have been shown to be equally effective at wound contraction and stimulation of blood flow at the wound edge [8]. Foam has been shown to provide rapid granulation [9], but this can be offset by in-growth with potential to disturb the epithelialisation process and also be painful when the foam is changed [10-13]. An example of multiple large wounds being treated with foam NPWT dressings can be seen in Fig. (2).
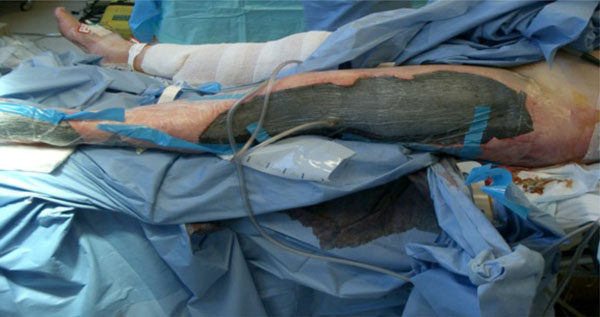
Multiple large wounds caused by a suicide bombing treated with NPWT dressings.
Base unit pumps can be set to various pressures and usually have two settings: continuous and intermittent. Wounds with high drainage require continuous suction and lower pressure settings tend to be indicated when wound edges are fragile, have low perfusion, are painful, or where a skin graft is being used [7]. A continuous pressure of -80 mmHg to -125 mmHg is therefore most commonly used in traumatic orthopaedic wounds.
CLINICAL INDICATIONS
As of January 2014, V.A.C. therapy has been used in over 861 peer-reviewed journals across all medical and surgical specialties, demonstrating its potential in acute and chronic wounds and post-operative recovery [14]. The evidence for its use in orthopaedic trauma departments initially focused on open fractures with soft tissue defects, but usage is frequently seen in contaminated wounds and more recently increasing evidence is emerging on its ability to aid closed incisions which have a high risk of wound breakdown. The evidence for its use on skin grafts is now well established.
Open Fractures with Soft Tissue Defects
Open fractures are at risk of developing complications; infection and nonunion are often the most common and can cause the most significant morbidity [15]. Published deep infection rates for open tibial fractures range from 8-12% [16-18]. NPWT dressings were first described in the medical literature for use with open fracture wounds [19].
The primary surgical treatment of an open fracture must always start with thorough debridement and stabilisation of the fracture before addressing the soft tissue defects [20]. Following the British Orthopaedic Association Standards for Trauma (BOAST) and British Association of Plastic & Aesthetic Surgeons (BAPRAS) guidelines ensures that a thorough exploration of the wound is performed that facilitates diagnosis of the extent of damage. A subsequent careful debridement of non-viable tissue and contaminants followed by irrigation reduces the risk of infection. Careful haemostasis and coverage of all vital structures such as vessels or nerves prepares the wound for the application of NPWT. Further debridement of tissue that subsequently declares itself non-viable may be required prior to healing by secondary intention with granulation tissue, wound closure or plastic surgical coverage [21]. It is these periods between operative interventions where NPWT is most commonly used and where it shows advantages over the standard wet to dry (WTD) dressings. This is particularly relevant to open fractures with extensive soft-tissue injury with reported infection rates as high as 66%, mainly caused by nosocomial bacteria [22, 23]. By sealing the wound between sterile theatre visits, NPWT offers protection from nosocomial contaminants as well as promoting local wound perfusion and drainage.
A number of studies have compared NPWT with WTD dressings in this setting. Stannard et al. [24] studied 62 severe high-energy open fractures, all receiving an initial irrigation and debridement and returning to theatre every 48-72 hours until wound closure. 37 fractures were randomised to interval NPWT and 25 had standard fine mesh gauze dressing. The NPWT group showed significantly less infections than the control (0 acute and 2 delayed versus 2 acute and 5 delayed, p=0.024). Of the entire study group of 58 patients, 21 had either a rotational, free flap or skin graft; but the infection rate in this group was not separately analysed.
A further study by Sinha et al. [25] randomised 30 open musculoskeletal injuries to NPWT dressings changed every 3-4 days or standard dressings daily. Each time the dressings were changed, measurements were taken and at day 4 and 8 post-initial debridement, tissue biopsies were taken for histopathological analysis. They found a significantly reduced wound size in the NPWT group over the 8 days (mean 13.24 mm versus 3.02 mm, p=0.0001), a reduction in bacterial growth by day 8 (60% no growth versus 20%), and significantly increased angiogenesis, granulation tissue and fibrosis (Wilcoxon signed-rank test p<0.05). All patients healed without infection, one required a free flap.
As a demonstration of the ability of NPWT to encourage the formation of granulation tissue over longer periods, Lee et al. [26] prospectively treated 16 patients with open wounds in the foot and ankle region demonstrating exposed tendon or bone. After initial debridement NPWT was applied and changed every 3-4 days for 11-29 days, 15 of the 16 patients healed by secondary intention (production of granulation tissue), a free flap was required in a single case. There were no reports of infection.
Blum et al. [18] retrospectively reviewed 229 open tibial fractures with 72% receiving NPWT and 28% conventional dressings. They found a significantly reduced deep infection rate in the NPWT group (8.4% versus 20.6%, p=0.01). When adjustment was made for the severity of the injury using the Gustilo classification, that was a univariate predictor of deep infection, NPWT was found to reduce the risk of deep infection by almost 80%. This is an extremely high figure even when taking into account the significantly higher rate of free flaps in the NPWT group (28% versus 14%, p=0.03). Over a similar retrospective period and in the same trauma centre, Liu et al. [15] from the Department of Plastics and Reconstructive Surgery found that following open lower limb trauma, soft tissue coverage within 3 days of injury and immediately following fracture fixation with exposed metalware minimised pre-flap wound infection and optimised surgical outcomes. NPWT provided effective temporary wound coverage, and did not delay definitive free-flap reconstruction.
Infected Wounds
The randomised clinical trial findings of, Stannard et al. [24] with NPWT patients a fifth less likely to develop infection, and Sinha et al. [25] with a reduction in positive bacterial cultures after 8 days of NPWT, are encouraging. There is some dispute, however, whether NPWT actually reduces bacterial load. Whilst the sealed environment and infrequent dressing changes reduces the potential for nosocomial contamination, the effect on initial contamination is unclear. An early NPWT animal model study by Morykwas et al. showed reduced bacterial loads of Staphylococcus aureus and Staphylococcus epidermis [2]. Conversely, a retrospective review of 25 patients undergoing NPWT showed an increase in bacterial load throughout the duration of treatment, although beneficial effects on wound healing were noted in most cases [27]. Lalliss et al. [28] used animal models to create complex open fractures contaminated with either Pseudomonas aeruginosa or Staphylococcus aureus. After a period of 6 days with 48 hourly debridements, a significant reduction in Pseudomonas levels compared to WTD dressings was seen, but there was no reduction in Staphylococcus aureus in either group. A further animal study has shown reduced bacterial loads of both Pseudomonas and Staphylococcus when comparing silver impregnated gauze with standard sponges after 6 days (43% versus 21% reduction in Pseudomonas contamination and 25% versus 11.5% in Staphylococcus aureus) [29].
NPWT therapy may reduce the effectiveness of antibiotic loaded polymethylmethacrylate (PMMA) bone cement beads. Stinner et al. [30] used a live animal wound model to demonstrate a reduction in effectiveness of vancomycin-impregnated cement beads when used in conjunction with NPWT. The wounds not subjected to NPWT showed a 6-fold reduction in bacteria after 2 days of treatment. Large, et al. [31] also used a live animal model to compare the effect of NPWT on antibiotic loaded PMMA beads but chose to measure antibiotic concentration rather than bacterial count. Sponges were placed directly on the beads or over a closed fascia prior to application of NPWT and compared to a group who had primary wound closure over the beads. All wounds had a deep drain inserted to measure eluted anti-biotics. Whilst those wounds with open fascia and NWPT showed significantly less eluted antibiotic in the drains, implying that the action of NWPT reduced antibiotic release, periosteal samples taken at 72 hours from the corticotomy sites to determine tissue antibiotic concentration were similar in all groups.
Incisions at Risk of Breakdown
There is emerging evidence to support the use of NPWT on closed surgical incisions and closed wounds that are deemed to be at high risk of wound complications such as breakdown or haematoma formation.
Meeker et al. [32] used a porcine model to demonstrate that wounds appeared significantly healthier and were stronger after 3 days of NPWT, with a significantly higher tensile strength. Stannard et al. [33] looked at the action of NPWT to treat haematomas and surgical incisions following high-energy trauma. 44 patients with post-surgical haemato-mas with wound drainage for more than 5 days were rando-mised to be treated with NPWT or compression bandaging. The NPWT group settled quicker, with a lower infection rate (1.6 versus 3.1 days; 8% versus 16% infection). 44 separate patients who had internal fixation of high risk fractures (calcaneus, tibial plateau, tibial pilon) were also randomised. Whilst the NPWT group had better post-operative drainage (1.8 versus 4.8 days to achieve grade 3 status–defined as drainage <2 quarter American dollar coin size drops, p=0.02), there were similar rates of wound breakdown and infection. A further paper from Stannard et al. [34], with a larger cohort of 263 high risk fractures, added to these findings. In this study infection rates in the NPWT group were shown to be lower than a control group (14 versus 23, p=0.049), with the relative risk of developing an infection calculated to be 1.9 times higher in the control group than in patients treated with NPWT (95% confidence interval 1.03-3.55). The use of NPWT for wounds at risk of breakdown has also been supported in a systematic review by the NPWT-EP [35].
Skin Grafts
The application of NPWT to a newly laid down skin graft is common practice, with a number of studies showing an improvement in graft incorporation using a pressure range between -50 to -80 mmHg [1, 36, 37]. Loss of partial-thickness skin graft has been shown to be consistently lower when compared to standard bolstering [38-40].
COMPLICATIONS
Despite the increasing clinical support for the use of NPWT seen in this article, very few studies have commented on the rate of complications in their series or the impact that the therapy has had on the patient. Failure of the vacuum pump has been shown to affect the efficacy of the therapy. In a series looking at 123 consecutive orthopaedic trauma patients treated with NPWT, 12 (10%) experienced the device unexpectantly powering off causing an initially unrecognised interruption of therapy. Despite 11 of those patients undergoing early (<6 hours) wound debridement and reapplication of NPWT, 7 patients experienced wound complications with an overall significantly higher rate of infection and graft loss (p<0.05) [41].
Pain and skin trauma have been noted in a number of studies when reviewing all applications of NPWT across all specialties. A recent systematic review of these identified 30 papers where this was noted. The article went on to indicate that a gauze-based dressing rather than foam may reduce both of these issues [42]. A randomised study on the use of NPWT versus sterile gauze dressings on closed total knee arthroplasty incisions had to be abandoned early as 15 of the 24 patients undergoing NPWT developed blistering [43].
In 2011, the US Food and Drug Administration (FDA) reviewed NPWT use over the previous 4 years both in hospitals and in the community [44]. In total, 12 deaths and 174 injury reports were attributable to NPWT. The most severe complications were seen in excessive bleeding from wounds near the groin, presternal region and over vascular grafts. They also noted that patients on anticoagulation or where there were significant adhesions between sponge and wound bed could excessively bleed at the time of dressings changes. They highlighted 27 reports that indicated worsening infection when treating infected wounds with NPWT and infection resulting from pieces of dressing that remained in the wound, and 32 reports that noted injury from foam dressing pieces and foam sticking to tissues or clinging to the wound.
The FDA subsequently released guidelines for healthcare providers using NPWT devices [45]. Quoting their online reference users are recommended to:
‘Undergo appropriate training on device use, including its indications and contraindications, and recognition and management of potential complications. NPWT training for patients and their caregivers who will be using the device at home should include how to:
- Safely operate the device; provide a copy of printed instructions for patient use from the specific device manufacturer;
- Respond to audio and visual alarms;
- Perform dressing changes;
- Recognise signs and symptoms of complications, such as redness, warmth, and pain associated with possible infection;
- Contact appropriate healthcare providers, especially in emergency situations;
- Respond to emergency situations; for instance, if bright red blood is seen in the tubing or canister, to immediately stop NPWT, apply direct manual pressure to the dressing and activate emergency medical services.’
CONCLUSION
NPWT is an attractive alternative to standard dressings in a number of orthopaedic trauma related wounds. Benefits include maintaining a seal against contamination and reducing the number of dressing changes. There appears to be a reduction in the rate of infection, but whether this is due to a decrease in nosocomial infection or due to the environment created by the NWPT is unclear and there may be a difference in effectiveness across types of bacteria. Routine NWPT practice should always include regular wound re-evaluation with debridement and irrigation as required.
With increasing adoption of NPWT and some good evidence for its efficacy, research centres may now not be willing to subject patients to standard dressings as control groups for trials. Further studies are, however, still required in a number of areas such as the duration of therapy, the effect on antibiotic concentration, and the effect on the type of dressing subjected to NWPT; for example silver impregnated, or gauze versus sponge.
As an emerging indication, there are some encouraging early results from the use of NPWT on post-traumatic surgical incisions. It will be fascinating to see whether further research can demonstrate whether NPWT can improve wound healing or reduce the impact of a post-surgical wound complication.
CONFLICT OF INTEREST
There are no financial or personal relationships between the contributing authors and any other people or organisations that could inappropriately influence or bias this review article.
ACKNOWLEDGEMENTS
Declared none.


