All published articles of this journal are available on ScienceDirect.
Outcome of Percutaneous Sacroiliac Joint Fixation with Porous Plasma-Coated Triangular Titanium Implants: An Independent Review
Abstract
Design:
Independent retrospective review of a single surgeon’s experience with a new technique of SI fixation.
Objective:
Examine results of percutaneous fixation of the SI joint with porous coated triangular titanium implants.
Background:
Diagnosis and treatment of a dysfunctional sacroiliac joint is challenging as well as controversial. Recently, percutaneous stabilization techniques have been implemented for fixation. There is minimal literature published on this technique.
Methods:
Charts, radiographs, and CT scans of 31 patients operated on by a single surgeon were de-identified and randomized and then reviewed by investigators not involved with the care of the patients. Reviewers had no relationship with the implant manufacturer at the time of the review. Outcome Measures: intraoperative and postoperative complication, EBL, hospital stays, postoperative image location and number of lucent implants, ingrowth into implants, and bone across SI joint.
Results:
27 patients expressed satisfaction, 4 patients did not. Pain relief was noted to be Complete (16 patients), Excellent (5 patients), Good (9 patients), and Fair (1 patients). Four patients had postoperative complications. These were infected hematoma (2), L5 nerve root irritation (1), and L5-S1 discitis (1). One patient required revision. On 6 month postop CT scan, 18/19 patients had radiographic evidence of bone ingrowth and bone into or across the SI joint was evident in 8/19 patients. Lucency was noted around at least one implant in 5/19 patients.
Conclusions:
Results are promising for the use of this novel implant for a carefully selected group of patients with disabling SI dysfunction.
INTRODUCTION
Complexity of diagnosis and controversy in treatment make sacroiliac (SI) joint pain a challenging condition to manage. Literature has shown that the SI joint is a legitimate pain generator in patients with low back pain (LBP) although still underappreciated [1]. Some authors have opined that 15-25% patients who presented with LBP had SI joint etiology [2].
The majority of patients with SI joint pain can be treated non operatively. When these treatments fail, some investigators have advocated for SI joint arthrodesis for patients with chronic and debilitating SI joint pain [3]. However, SI joint arthrodesis in the absence of joint destruction from disease process, trauma, or other causes of severe instability remains controversial [4]. SI joint arthrodesis studies exist that report a varying degree of success, most being satisfactory, for treating chronic and debilitating SI joint pain.
Open and percutaneous approaches have been described in literature for SI joint arthrodesis. Studies have shown the benefits of percutaneous approach to be smaller exposure, less blood loss, preservation of the inherent stability of the SI joint, reduced length of hospital stay, and little wound-related morbidity [3, 5-8].
The aim of this study is to independently review the radiographic and surgical results of a new technique of SI fixation. The procedure involves percutaneous placement of triangular titanium implants with a porous plasma spray coating across the SI joint (Figs. 1, 2).

Porous plasma-coated triangular titanium implants (SI-Bone, San Jose, CA). *
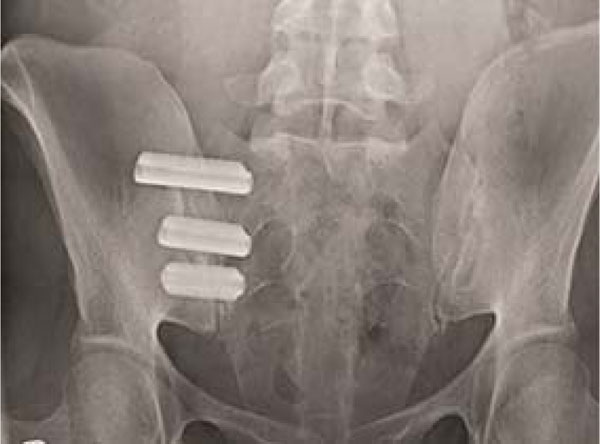
Postoperative X-ray at 12 months following SI fixation using iFuse (SI-Bone, San Jose, CA) implants.
MATERIALS AND METHODS
Patient Selection
31 patients under the care of a single surgeon underwent sacroiliac joint fixation between 10/24/2007 to 10/14/2009. There were 7 men and 24 women. Their mean age was 54.3 years at the time of surgery (range 34-85). Mean follow-up period was 13.7 months (range 6-30). 29 of 31 patients had a minimum of 12 months of follow-up. The demographic information is summarized in Table 1. 23/31 patients had one or more comorbidities with hypertension and hyperlipidemia being most common.
Demographic Information
| Description | Number |
|---|---|
| Number of patients | 31 |
| Mean age (years) | 54.3 |
| Gender (male/female) | 7/24 |
| Mean follow-up (months) | 13.7 |
| Patients with previous spine surgery | 15 |
| Patients with previous iliac crest bone graft (n) | 3 |
| Patients with smoking history (n) | 10 |
| Workmans Comp | 3 |
On initial presentation, the chief complaint was posterior SIJ pain in 18 patients, low back pain (LBP) in 10 patients, and combination of SIJ pain and LBP in 3 patients. History was consistent with possible SI joint pain in all patients. 25/31(81%) patients were tender to palpation over posterior SI area. 28/31 (90%) patients had positive SIJ provocative maneuver exam. The mechanism of SI joint injury was identified in 8 patients (falling, car accident, lifting, twisting).
All patients who underwent surgery had chronic sacroiliac pain unresponsive to prolonged nonoperative treatment. Although there were no strict criteria in place for length of time, symptoms were present to decide upon surgery, symptoms were almost universally present for a minimum of six months. All patients had failed a trial of medication and decreased activity. Medications routinely included non steroidal anti inflammatory drugs (NSAIDS) and often narcotic medication as well. Most had also had a trial of physical therapy. No attempt was made to standardize pre operative treatment protocols prior to surgery. After a trial of nonoperative treatment, patients received SI joint injections of local anesthetic and steroid under CT guidance. All patients had complete or near complete pain relief with sacroiliac joint injections. The diagnosis of sacroiliac disease was based on the history, clinical exam, radiological evaluation, and confirmed as best as possible with diagnostic injections. Only after meeting the above criteria were patients offered and treated with percutaneous SI joint fixation using porous plasma-coated triangular titanium implants (SI-Bone, San Jose, CA). Every procedure was performed by one orthopaedic surgeon. The treating physician has an equity interest in the company manufacturing this implant (estimated $100,000) and is a paid consultant for the company. The other authors had no financial ties to the company at the time of the review. After concluding the study and presentation of the results, one of the other authors has since given an educational talk on diagnosis and treatment of sacro iliac problems. His travel expenses were paid by the company manufacturing this implant (estimated $1000).
Surgical Technique
The patients were placed prone with the hips flexed. The operative site was sterilely prepped and draped exposing the iliac spine and lateral buttock on affected side. The image intensifier was used to line the site of the incision. A 3 cm incision was made over the superior posterior portion of the sacrum. Dissection was carried down through the skin and subcutaneous tissue. The fascia of the gluteal muscles was perforated to allow for pin and broach placement.
A guide pin was then passed into the superior sacrum. This was checked in the AP and lateral planes. The length of iFuse Implant (SI-Bone, San Jose, CA) was determined. A tissue guide was placed over the superior pin to drill to the desired depth corresponding to the length of the fusion rod. With drill removed, a broach was impacted across SI joint using a slap hammer under radiographic visualization. Then, the appropriate sized implant was inserted. This was repeated, as needed, for additional implant placement. With image intensifier, AP, inlet, outlet, and lateral views were checked to evaluate the implant position. Twenty seven out of thirty one patients had three implants placed.
Post operative management consisted primarily of protected, partial weight bearing ambulation. Initially this was for eight weeks but after the first six months of doing the procedure, this was shortened to six weeks. Physical therapy was prescribed if the treating physician felt it necessary.
Outcome Assessment
After appropriate Institutional Review Board approval, medical charts, plain radiographs, and CT scans were reviewed retrospectively by investigators to determine the radiographic and surgical outcomes. The reviewers had no relationship with the patients or with the company producing the implants.
Plain radiographs and CT scans were evaluated to assess radiographic outcome of the procedure. Each patient obtained x-ray and CT scan at 6 and 12 months post-operatively. These were de-identified and randomized prior to radiographic assessment. Radiographic outcome consisted of evaluating presence and extent of osseous ingrowth into the implant surface (Fig. 4), lucency that may imply loosening. (Fig. 3A, B), bone growth across the sacroiliac joint (Fig. 4), and radiographic complications such as fracture, violation of the sacral foramina or evidence of loosening. A single practicing spinal Orthopaedic surgeon evaluated all of the studies. A single Orthopaedic resident reviewed and documented all records.
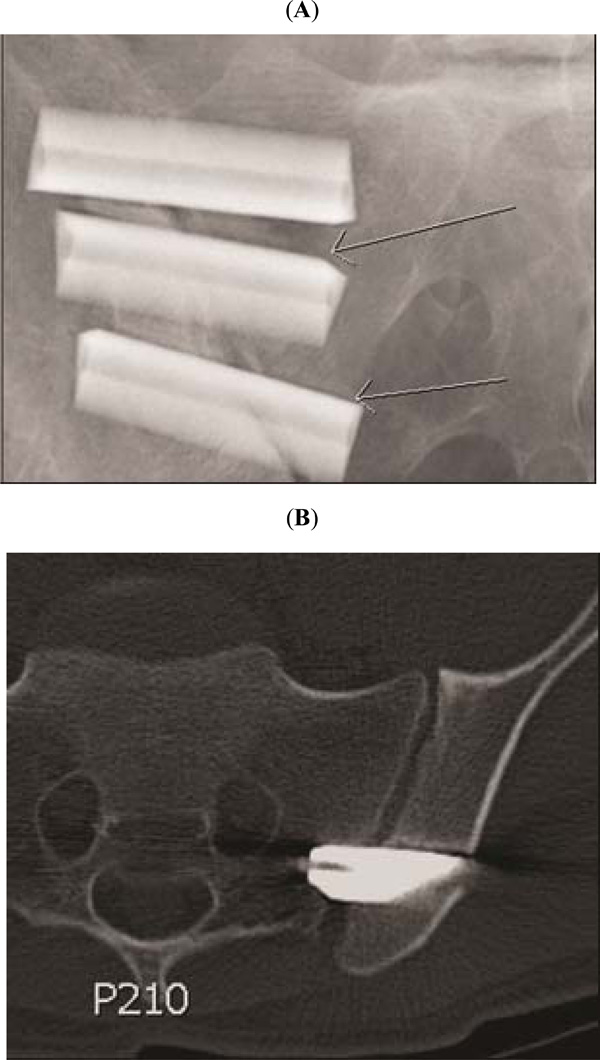
(A, B) AP radiograph and axial CT demonstrating lucencies around implants.

CT showing near complete bone bridging.
Medical charts including operative notes were retrospectively reviewed to assess surgical outcome of the procedure. Surgical outcome consisted of identifying intra-operative/postoperative complications, patient satisfaction, postoperative pain relief, EBL, and hospital stay.
RESULTS
There were no intraoperative complications. Estimated blood loss was minimal in each case. Every patient was discharged home on post-operative day 1. One patient (3%) required a revision due to nerve root irritation by an implant. Two (6%) developed incisional hematomas that resolved with observation and one developed de novo L5-S1 discitis. At the most recent follow up, 16 (52%) patients reported no pain after the procedure, and 14 (45%) patients reported good to excellent pain relief. All walked full weight-bearing by 16 weeks. 27/31 (87%) patients expressed satisfaction with the procedure. Surgical outcomes are summarized in Table 2 and Fig. (5).
Surgical Outcomes in 31 Patients
| Description | Number |
|---|---|
|
|
|
| Right/Left | 23/8 |
|
|
|
| Number of Implants | |
| Three | 27 |
| Two | 3 |
| Four | 1 |
|
|
|
| Intraoperative Complication | 0 |
|
|
|
| Estimated Blood Loss | |
| Minimal | 31 |
|
|
|
| Hospital Stay | |
| One day | 31 |
|
|
|
| Patients With Revision | 1 |
|
|
|
| Satisfied Patients/Unsatisfied Patients | 27/4 |
|
|
|
| Postsurgical Pain Relief | |
| No Pain | 16 |
| Excellent | 5 |
| Good | 9 |
| Fair | 1 |
|
|
|
| Walking Full Weight-Bearing | |
| By 8-9 weeks | 8 |
| By 12 weeks | 21 |
| By 16 weeks | 2 |
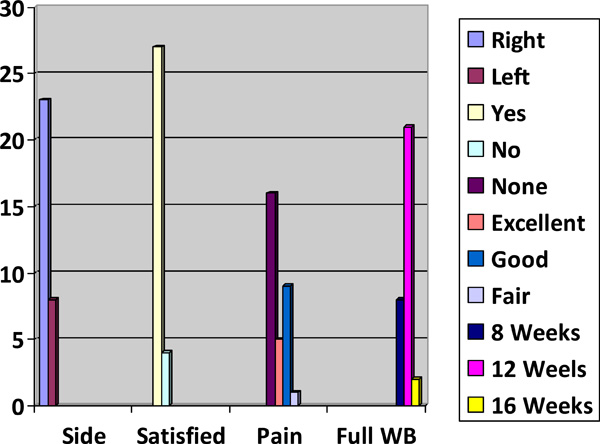
Graphic representations of outcomes.
26 patients had immediate postoperative imaging reviewed. Of these, 21 (81%) had implants fully within the bone of the ilium and sacrum (Table 3). With the exception of the patient who underwent revision, extra osseous position did not seem to correlate with outcome. 19 patients had imaging available at 6 months after surgery (Table 4). Of these, 18/19 (95%) patients had radiographic evidence of bone ingrowth into at least one side (sacral or iliac) of the implant on CT scan. Bone growth into or across the SI joint was evident in 8/19 (42%) patients although definite bony arthrodesis was not seen. There also was noted to be a lucency around at least one side of an implant in 5/19 (26%) patients. 15 patients had imaging available at one year after surgery (Table 4). 4/15 (27%) patients had continued lucency around at least one implant. None had lucency around all three. Somewhat more bone was seen within the joint when compared to the six month imaging but clear bony arthrodesis remained uncommon. 4/31 (13%) patients were not satisfied with their result although three of them reported good pain relief. Details are given in Table 5.
Immediate Postoperative Radiographic Images for 26 Patients
| Description | Number |
|---|---|
|
|
|
| All implants fully in bone | |
| YES (number of patients) | 21 |
| NO (number of patients) | 5 |
|
|
|
| Total number of implants not fully in bone | 6 out of 72 |
| Upper Implant | 5 |
| Second Implant | 1 |
| Third Implant | 0 |
|
|
|
| Location of implants not fully in bone | |
| Foramen | 2 |
| Anterior Sacrum | 4 |
|
|
|
| Other complication* | 1 |
* Third implant in one patient was not completely across SI joint.
6 and 12 Month Postoperative CT Scans
| Description | 6 Months N =19 | 12 Months N=15 |
|---|---|---|
|
|
||
| Patients with lucent implant | 5 /19 | 4/15 |
|
|
||
| Total number of implants with lucency | 8 /55 | 7/45 |
| Complete | 0 | 2 |
| Incomplete | 8 | 5 |
|
|
||
| Implants with lucency | ||
| Upper Implant | 0 | 4 |
| Second Implant | 3 | 1 |
| Third Implant | 5 | 2 |
|
|
||
| Location of implant lucency | ||
| Sacral Side | 7 | 3 |
| Iliac Side | 1 | 2 |
| Both | 0 | 2 |
|
|
||
| Patients with ingrowth into implants | 18/19 | 12/15 |
|
|
||
| Total number of implants with ingrowth | 43/55 | 33/45 |
| Sacral Side | 1 | 1 |
| Iliac Side | 11 | 5 |
| Both | 31 | 27 |
|
|
||
| Bone across SI Joint | 8/19 | 8/15 |
| None | 11 | 7 |
| Non-contiguous | 4 | 3 |
| Contiguous <1cm | 4 | 4 |
| Contiguous >1cm | 0 | 1 |
Unsatisfied Patients
| Description | Number |
|---|---|
|
|
|
| Total Number | 4 |
|
|
|
| Mean Age (years) | 55.3 |
| Gender (male/female) | 0/4 |
| Previous Spine Surgery | 3 |
| Workmans Comp | 1 |
| Previous iliac crest bone graft | 1 |
|
|
|
| Postsurgical Pain Relief | |
| No Pain | 0 |
| Excellent | 0 |
| Good | 3 |
| Fair | 1 |
|
|
|
| NWB Compliance Postop | |
| Yes | 2 |
| No | 2 |
|
|
|
| Postop Complication | |
| Infected Hematoma | 1 |
| Traumatic Fall | 1 |
|
|
|
| Radiographic Lucency | 4 |
|
|
|
| Implant Fully in Bone | |
| Yes | 2 |
| No | 2 |
|
|
|
| Bone Ingrowth | 4 |
|
|
|
| Bone Across SI Joint | |
| None | 3 |
| Non Contiguous | 1 |
| Contiguous <1cm | 0 |
| Contiguous >1cm | 0 |
DISCUSSION
The SI joint was widely viewed as a potential source of low back pain and dysfunction until 1930’s when the idea that facet arthrosis and lumbar disc disease can cause low back pain arose [9,10]. As this idea gained popularity and acceptance, it seemed to push the SI joint pain and dysfunction theory into obscurity [11]. While SI joint pain and dysfunction remain a controversial and challenging topic, it appears that SI joint may be an underappreciated etiology of low back pain [4]. Currently, it is felt that dysfunctional SI joint is the culprit in 15-25% patients who present with low back pain [2].
The published literature on surgical treatment of chronic painful SI joint dysfunction dates back to early 20th century. A literature search yielded 11 articles describing open procedure [11-21] and 5 articles describing percutaneous procedure [3, 5-8] for surgically treating chronic SI joint problems. These studies, most of them being a small retrospective case series, reported well to excellent improvement in pain and/or function in 168 out of 211 patients (79.6%). When divided further into open procedure and percutaneous procedure studies, the satisfactory clinical results were 77.2% and 88.6%, respectively. Every open procedure study needed bone graft harvest for SI joint arthrodesis while six out of 11 studies required external immobilization postoperatively. On the other hand, only one out of five percutaneous procedure study required bone graft harvest and external immobilization.
Treating a chronic SI joint dysfunction surgically still remains controversial, but it appears that SI joint arthrodesis or fixation can produce favorable and clinically satisfactory outcome with acceptable rate of complications. Based on the published studies, surgical arthrodesis or fixation is a viable option for patients with chronic debilitating SI joint dysfunction. Because most patients can be managed non operatively, surgical procedures should be considered for a carefully selected group of patients not responding to non operative management [1].
Percutaneous SI fixation using porous plasma-coated triangular titanium implants has not been previously described in literature. This has the advantage of being minimally invasive and potential advantage of not requiring the use of bone graft to achieve long term stabilization. The surgical outcome of this new procedure has been positive in most patients in this study. There were no intraoperative complications. EBL was minimal in each case. Every patient was discharged on post-operative day 1. 27 out of 31 patients reported satisfaction with the procedure. Postoperative pain relief was good, excellent, or complete in 30 out of 31 patients. However, there were 4 postoperative complications in which one patient with L5 nerve root irritation required revision. The other three patients had an uneventful postoperative course despite having infected hematoma and discitis, which was treated appropriately.
It is unclear from the radiographic review whether these patients will go on to develop a bony arthrodesis of the SI joint. Although a significant percentage did show some evidence of bone growth in to the joint, we do not have enough longitudinal radiographic information to know if this process continues. It is also unclear at present whether radiographic evidence of foramenal violation, cortical violation, or lucencies seen on CT scan at 6 and 12 months has an effect on clinical outcome. A much larger sample will be needed to determine this.
In our study, there were 4 patients who were not satisfied with this procedure. They were all female patients with mean age of 55.3 years, and three of them had previous spine surgery. Only one patient was involved in a worker’s compensation case. Postoperatively, two patients were not compliant with non-weight bearing status until the first postoperative clinic visit. One patient was doing well postoperatively until sustaining a fall down a full flight of stairs. After the fall, the preoperative SI pain returned. One of the unsatisfied patient’s postoperative courses was complicated by superficial infected hematoma that required 4 weeks of intravenous antibiotics. This patient reported persistent pain in the lumbosacral junction region although this pain was relieved close to 100% by preoperative CT-guided injection.
The radiographic and surgical outcomes of this new technique of percutaneous SI fixation were independently reviewed. The result of this new novel percutaneous SI fixation using porous plasma-coated triangular titanium implants is promising and compares well with other published clinical studies. SI fixation with this novel implant provides advantageous bony interference fit to decrease motion postoperatively as well as probable bony ingrowth into porous biologically friendly implant surface for long term stability. Literature to date has shown that percutaneous approach to SI fixation or arthrodesis has a higher rate of clinical success, less need for bone harvest, infrequent postoperative immobilization requirement, shorter length of hospital stay, and less wound-related morbidity [3, 5-8].
CONCLUSION
When patients with chronic disabling SI joint pain fail conservative treatments, we feel that percutaneous SI fixation and/or arthrodesis is an option for a carefully selected group of patients in the hands of meticulous and experienced surgeon. In this study the selection process included; diagnosis of the sacroiliac joint as being a likely pain generator by history, physical examination, imaging and diagnostic intra articular injection as well as lack of response to prolonged non operative measures.
CONFLICT OF INTEREST
Dr. Kim - No conflicts.
Dr. Glaser - Consultant Depuy Spine $500, Travel Expenses SI bone (after completion of this study) $1000.
Dr. Rudolf Stock ownership $100,000, and paid consultant SI Bone.
DSICLOSURE
The implant discussed in this manuscript is FDA approved for the diagnoses of degenerative sacro-iliitis and sacro-iliac disruption.
ACKNOWLEDGEMENTS
Declared none.


