All published articles of this journal are available on ScienceDirect.
Femoral Stem Displacement in a Patient Suffering Recurrent Dislocations After Hip Hemiarthroplasty: Case Report
Abstract
Displacement of the femoral component during attempt to closed reduction of a dislocated hip arthroplasty is an exceptionally rare, catastrophic event, which renders operative management obligatory. We report the proximal migration of a femoral stem during attempt to closed reduction in a patient with recurrent postoperative dislocations after hip hemiarthroplasty, and describe successful management by conversion to a standard total hip arthroplasty, retaining the same stem in the existing cement mantle. This illustrative case is reported not only as an extremely rare event, but also to highlight and discuss pitfalls and efficient measures in the management of this complex issue.
INTRODUCTION
Hemiartroplasty of the hip (HH) is a very common procedure in the treatment of displaced cervical fractures of the femur in senile patients, as well as those suffering from multiple comorbidities or cognitive impairment. Dislocation, which is reported in a frequency of up to 16 % [1], is a well known complication. However, not much is reported on the management of recurrent dislocations. Repeated attempts to closed reduction or even decision to leave the prosthesis dislocated can be considered for patients with low demands [2]. Other methods, such as injection of botulinum toxin [3], or conversion to a Girdlestone excision arthroplasty or to a total hip arthroplasty (THA) have been proposed, and remain to be validated [2].
One devastating event during closed reduction, which anecdotally appears in the literature, is displacement of the femoral component. This renders open surgery necessary, and choice of the appropriate procedure even more demanding. Dislocation of the stem was previously reported in five cases [4-8] where a highly polished femoral component was used, and in one case of a textured implant [9]. In the case of tapered polished stems, cementing a new prosthesis in the existing cement mantle or revision may be considered. Simple reinsertion in the cement mantle has once been tried and proposed as an alternative method [8].
A case of a femoral stem migration during attempt to closed reduction in a patient that experienced recurrent dislocations early after HH is reported. Relocation of the stem in the same cement mantle was inefficient as the patient continued to dislocate the hip, although the stem did not redisplace. Definitive management was accomplished by converting to a THA.
CASE REPORT
An 88-year old female patient, with multiple comorbidities, namely hypertension, angina, heart failure, atrial fibrillation and diabetes was admitted to the emergency department after a fall. She was shown to have sustained a dislocated cervical fracture of the hip (Fig. 1). The patient was operated the next day. A HH was performed, using the anterolateral surgical approach. The femoral component consisted of a polished Exeter stem, which was cemented using standard surgical technique. A 47,5 mm head was used. Considerable degeneration of the gluteal muscles and a manifest trochanteric bursitis were apparent, but every effort was done to adapt the muscles firmly to the femur. Control of ROM during the operation did not reveal any instability of the prosthesis and tension of the soft tissues was evaluated as adequate. Radiographs taken after the procedure showed an adequately placed HH (Fig. 2). She was discharged from the ward a week later. Approximately five weeks after the operation the patient sustained a spontaneous dislocation (Fig. 3). Closed reduction was performed under fluoroscopy control and general anaesthesia, with manual traction of the extremity in the recumbent position. During the procedure, range-of-motion (ROM) was evaluated, and the patient was judged to have a stable implant. The next day the patient was found to have dislocated again. However, attempt to closed reduction in the same manner as described above resulted in the displacement of the femoral component from the cement mantle and its proximal migration (Fig. 4).
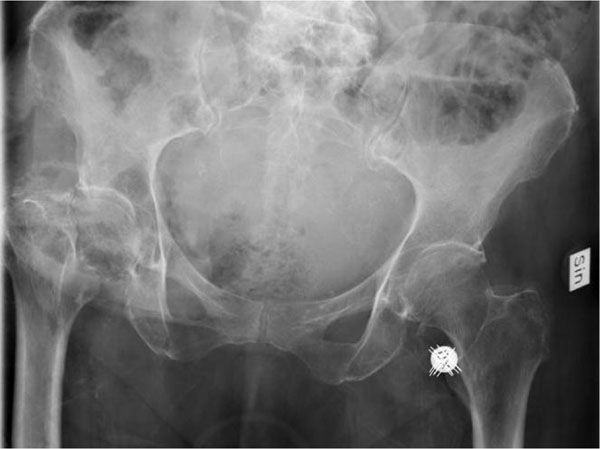
Anteroposterior radiograph of the pelvis during admission of the patient, showing a displaced femoral neck fracture on the right side.
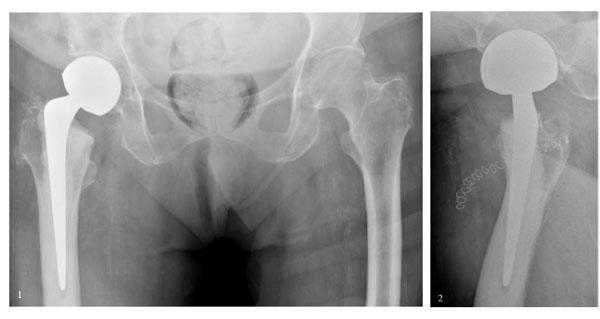
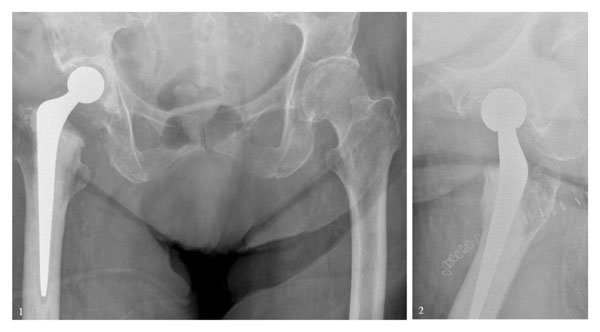
(1) Anteroposterior radiograph of the pelvis and (2) lateral radiograph of the right hip after conventional hemiarthroplasty.
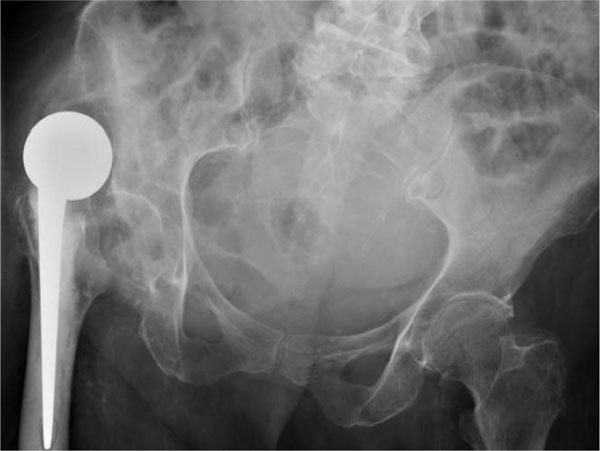
Anteroposterior radiograph of the pelvis showing proximal dislocation of the hip.
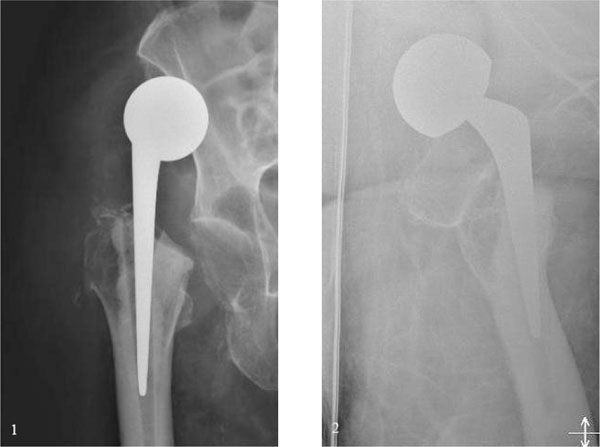
(1) Frontal and (2) lateral radiograph of the right hip showing proximal migration of the femoral stem that has dislocated from its cement mantle.
Taking into account the functional needs of the patient as well as the underlying comorbidities, an attempt to open reduction with reinsertion of the implant in the same cement mantle was considered as the first-choice solution. During operation, the gluteal muscles were found to have detached from the femur. The stem was freed, removed from the cement socket, which inspected free of any macroscopical damages. It was estimated to have an adequate placement in the femur, although it lacked a cement shoulder, which eventually hinders displacement during attempt to closed reduction. After thorough washing, the implant was reinserted and gently tapped in the cement mantle. The soft tissues were adapted carefully. Control of ROM did not reveal any instability. The patient was allowed to weight-bear without any brace. Five days later, she experienced another spontaneous dislocation while ambulating. Radiographs showed a cranial dislocation, with the stem stable in its mantle. Conversion to THA was the solution of choice in this stage, with every effort to intraoperatively identify and compensate for anatomical factors that predisposed to the recurrent dislocation.
During the operation, the stem and head was found to have dissected through the gluteal muscles, and were entrapped in this position. The muscles were partially detached from the femur. The stem was firmly positioned in the cement mantle, and did not detach even when substantial force in order to remove the head was exerted. The acetabulum was small and shallow, and this was apparently the main anatomical factor contributing to instability. Revision of the stem was deemed as unnecessary, and the prosthesis was subsequently converted to THA by cementing a Marathon 40-28 mm polyethylene cup. A standard 28-mm cobalt chrome head was used. ROM revealed that the prosthesis was stable, without any impingement. Radiography revealed a well-placed THA, with the cup in 40 degrees of inclination and approximately 15 degrees of anteversion (Fig. 5). The patient recovered uneventfully, and no functional impairment or dislocation was observed during follow-up.
(1) Anteroposterior radiograph of the pelvis and (2) lateral radiograph of the right hip after conversion to a total hip arthroplasty.
DISCUSSION
HH is reserved for elderly patients with substantial comorbidities. There are only few previous studies that address the problem of the recurrent dislocator. Conservative measures usually fail, and various invasive procedures have been proposed. In one previous study [2], successful restoration with minimum morbidity was accomplished by conversion to THA. Theoretically, conversion of a hemiarthroplasty to a THA would result in an increased risk of dislocation, since a head of substantially smaller diameter is used. In our case, a standard 28-mm head was used, as the acetabulum was too small to receive a cup that allowed use of a larger head. This however proved safe, as the key anatomic factor, namely a shallow acetabulum, was efficiently addressed. In general, use of the lar-gest head possible, or a constrained prosthesis, is definitely encouraged. It is of imperative importance that the surgeon identifies the predisposing factor(s) that result in dislocation, and has a clear strategy in order to cope with the problem. In our hands, intraoperative control of stability proved to be unreliable. Although the hemiarthroplasty was evaluated as stable after both closed and open reduction, it readily dislocated when it was subjected to weight bearing.
Displacement of the femoral component during attempt to close reduction is an extremely rare event, which has sporadically been reported in the literature [4-9]. This is, to our knowledge, the first report of a stem displacement during reduction of a unipolar hemiarthroplasty. Thus far, this complication was mainly observed during reduction of a dislocated THA [4-7, 9], and once in a bipolar hemiarthroplasty [8]. It is possible that the simplicity of the design, render unipolar HA less susceptible to this event. We report for the first time that dissection of the friable gluteus muscles and proximal entrapment of the large HA head was the anatomical factor responsible for irreducibility of the prosthesis and subsequent stem displacement. Thus far, other factors, namely entrapment in the psoas or rectus femoris muscles [10, 11], as well as capsule interposition [12], have been recognised. In line with previous reports, displacement happened during forceful traction manoeuvre in the recumbent position. The Stimpson method has been suggested as a safer alternative [9], although it is quite hard to believe that an anatomical hinder as the one encountered in our case can be overcome with any closed reduction method.
Of notice, as in previous reports, displacement happened in the absence of a cement mantle over the shoulder of the femoral component. This has been proven to offer mechanical stability and is strongly recommended in the case of highly polished stems, such as the Exeter design, which are inherently more susceptible to displacement [7, 13]. We also argue that simple reinsertion of the polished component in the cement mantle is a safe procedure, and does not result in loss of mechanical stability. The surgeon has an advantage in comparison to textured implants, which often have to be re-cemented in a cement-within-cement procedure. The latter obviously results in longer operative time, and raises questions about the longevity of the inner cement mantle, which is often thin and thus prone to fracturing in the long term.
We have recently performed the same procedure in another patient that displaced his polished stem from the cement mantle during attempt to closed reduction of a dislocated THA. Short-term follow up has been uneventful.
In conclusion, recurrent dislocation after hip hemiarthro-plasty is a serious complication, which requires thorough identification of the predisposing mechanism in order to be addressed efficiently. Conversion to a THA offers an effective alternative in selected patients. The eventual displacement of the femoral component is an extremely rare event, and can be safely managed with simple reinsertion in the cement mantle in the case of highly polished tapered designs.
CONFLICT OF INTEREST
None declared.
ACKNOWLEDGMENT
None declared.


