All published articles of this journal are available on ScienceDirect.
Is the Use of Biodegradable Devices in the Operative Treatment of Avulsion Fractures of Fingers, the So-Called Mallet Finger Advantageous? A Feasibility Study with Meniscus Arrows®
Abstract
Purpose:
Treatment of Mallet fingers or fractures remains a controversial topic. No evident preference can be distilled from the reports of the clinical results obtained by conservative treatment with splints and internal fixation. If operative treatment is indicated, several techniques can be used. However, each technique has disadvantages like the risk of comminution of the fragment, the risk of infection and necrosis, a demanding operative technique and-or the necessity of removing the metallic devices. This can be avoided by the use of biodegradable devices. The purpose of this feasibility study was to evaluate the outcome of internal fixation of a Mallet fracture with a biodegradable device, the Meniscus Arrow®.
Methods:
We treated nine consecutive patients with a Mallet fracture by fixation of the fragment with a biodegradable Meniscus Arrow®, at this moment the smallest device available, with an average operation time of 14 minutes.
Results:
Postoperatively, no complications were found. All patients were satisfied by the results after surgery, with a restored range of motion in the distal interphalangeal joint as previously and good alignment with full consolidation of all fractures at radiological evaluation.
Conclusions:
The operative treatment of bony mallet fingers with the Meniscus Arrow® is a fast procedure without complications in our prospective series of nine patients and without the need of a second operation to remove the implant.
INTRODUCTION
Intra-articular fractures at the dorsal base of the distal phalanx are usually referred to as Mallet fingers or Mallet fractures. The injury occurs during a forced flexion of the distal interphalangeal (DIP) joint. Treatment of mallet fractures remains a controversial topic. No differences in the clinical results between conservative treatment with splints and operative fixation are reported [1].
However, operative treatment has been suggested for fractures involving more than 30% of the articular surface or those with palmar subluxation [1].
Many surgical techniques have been described, such as the reduction and fixation with Kirschner (K-) wire under direct vision [2], tension wire fixation [3], extension block fixation (the Ishiguro method) [4], micro screw fixation [5] and interosseus wiring [6]. However, each technique has disadvantages like the risk of fragmentation or infection, a demanding operative technique and necrosis and-or the necessity of removing the metal devices.
The use of a small, easy to insert biodegradable device has several advantages: an easy method, no further damage of the fragment and no need for a removal procedure.
This paper describes the technique and results of the open reduction and internal fixation of mallet fractures with a small biodegradable device, the Meniscus Arrow® (Bionix Implants Ltd Tampere, Finland) in a consecutive series of nine patients.
MATERIALS AND METHODS
Between May 2005 and July 2007 we included in a prospective series nine patients with a Mallet-fracture. The indication for surgery was a displaced fracture involving more than one-third of the articular surface, or palmar subluxation.
All operations were performed by one surgeon in day surgery. The mean over all operation time was 22 minutes (range 16-33 minutes).
Postoperatively, a Mallet splint immobilisation was applied for four weeks. All patients were seen in the out-patient clinic, one week postoperatively, for removal of the stitches and wound control. They were allowed to start exercises after splint removal and consolidation of the fracture. The mean time of follow-up was two months.
Six of the nine patients were men the average age was 38 years (range 16-56 years). Five fractures occurred during sports activities and four during work. In seven patients the injury occurred in the dominant hand. Mostly the thumb or dig. 5 were involved (three times respectively four times). The mean time from injury to surgery was 14 days (range 5 - 30 days) (Table 1).
Demography of Included Patients
* Time between trauma and surgery (days).
** Operation time (minutes).
Surgical Technique
Under general or regional anaesthesia and bloodless field open reduction was performed through a small incision dorsally of the DIP joint (Fig. 1). In case of widely displaced fractures reposition was accomplished with a small reposition forceps. A hole was drilled through the shaft with the hand instrument of 1.0 mm in diameter under image intensifier control and a biodegradable Meniscus Arrow® of 10 mm in length was inserted in the shaft and inserted into the drill hole by gently hammering (Figs. 2, 3). Finally the reposition and fixation of the fracture were verified by X-Ray.
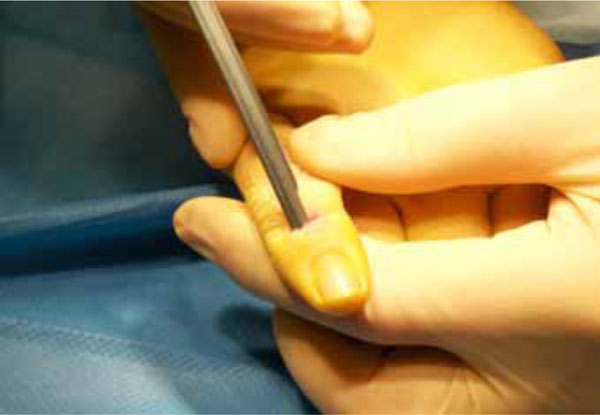
Position of the shaft.
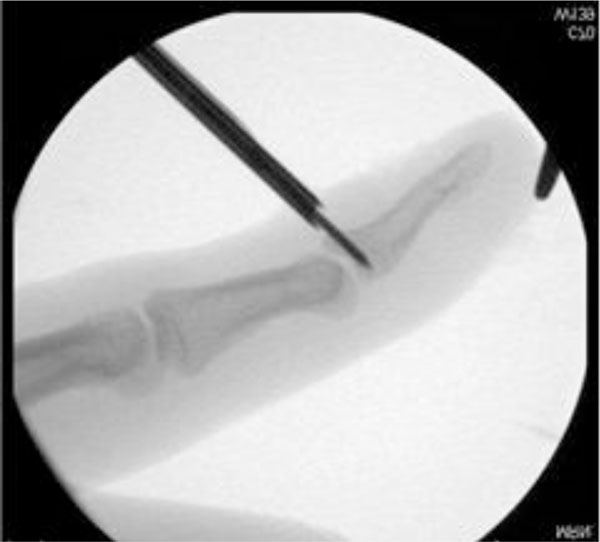
Position of the hand drill in de distal phalanx.
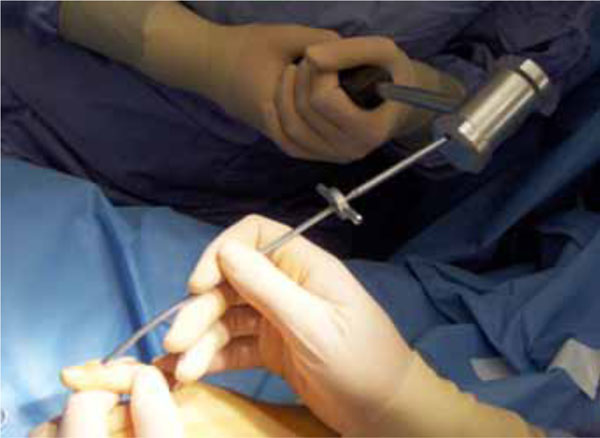
Gently hammering the Meniscus Arrow® in place.
Evaluation
All patients returned at the out-patient clinic for follow-up, including examination, radiographs and a patient-satisfaction at 1, 4 and 6 weeks.
The following data were analysed: consolidation of the fracture, alignment, range of motion, presence of deformity, nail bed deformity, pain, satisfaction and level of activity.
RESULTS
Clinical Data
One patient showed a limitation of flexion in the distal interphalangeal joint of 10º, but this existed preoperatively due to arthrosis. No extension lag was found. All patients had a full range of motion in de proximal interphalangeal joint as well as in the metacarpophalangeal joint.
Another patient developed a period of decreasing pain during flexion in the distal interphalangeal joint at the site of the fracture, until two months after surgery, finally she was able to perform all daily activities without any pain. All patients were satisfied about the results after surgery. The time to return to daily work was about 2 weeks, in which the Mallet splint was still in place for another 2 weeks.
Radiographic Data
After 6 weeks all fractures showed good alignment with full consolidation on X-Ray examination (Fig. 4).
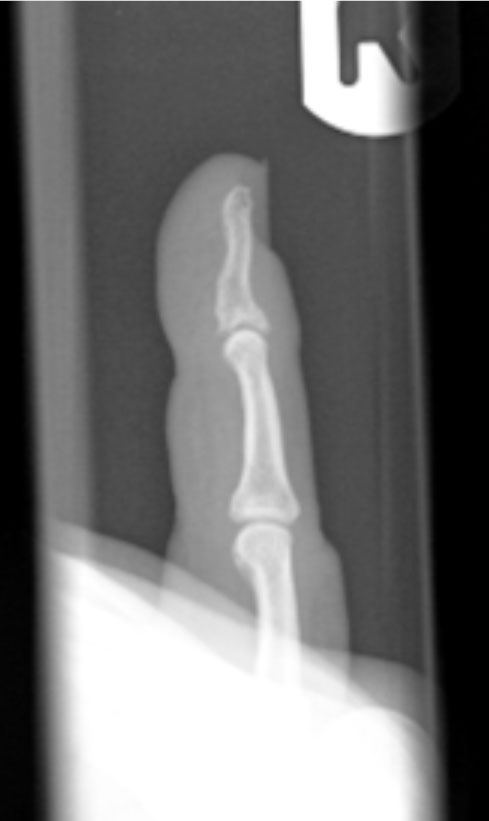
X-ray, 4 weeks postoperatively.
Complications
On physical examination no nail bed deformities or dorsal bumps were found. All wounds healed without complications. No patient had a second procedure related to the Mallet injury or surgery.
DISCUSSION
Literature of Mallet Fracture Treatment
Non-operative treatment has proved to be relative effective in Mallet finger deformity due to disruption of the extensor tendon [7], but Mallet fractures should be considered as a different entity.
Treatment of mallet fractures remains a controversial topic. Standard treatment consists of a Mallet-splint for six weeks [1], after which patients are treated functionally. Indications for operative treatment are failure of conservative treatment with persistent pain, fractures involving more than 30% of the articular surface or those with palmar subluxation.
Several surgical techniques for mallet fractures have been reported; however, each technique has disadvantages like the possibility of fragmentation, a demanding operative technique and the necessity of removing the metal devices. Complications of operative treatment, like infection, skin slough and nail deformity have been reported [8, 9].
We found no large series of Mallet fractures in the literatue, treated either operatively or non-operatively.
Introduction of the Meniscus Arrow
Meniscus Arrows® have been shown to have a remarkable hold in bone [10].
Smart Nails® could be used as well, but have the disadvantage of a considerable larger head and diameter [11].
This series of nine patients showed satisfaction of all patients. There were no cosmetic or other complications. Radiographic results showed alignment and full consolidation of all fractures with a full range of motion in all but one patient. However, the flexion limitation in this patient was pre-existent due to arthrosis.
Special attention must be paid during this procedure to maintain the exact position and angle of the shaft, otherwise the Meniscus Arrow® will bend against the intact bone instead proceeding into the drill hole.
Limitations of this Study
This is a feasibility study using Meniscus Arrows® for Mallet fracture treatment with a small study population. Moreover, there was no data to compare with other operative or conservative methods. These are two limitations of this study and we recommend a prospective study to compare Mallet fracture treatment by Meniscus Arrow® with other operative or conservative treatments.
IN CONCLUSION OF THIS STUDY
In conclusion, the operative treatment with the Meniscus Arrow® is a fast, successful procedure without complications in our consecutive series of nine patients and without the need of a second, implant removal, procedure.


