All published articles of this journal are available on ScienceDirect.
Arthrodesis of the Distal Interphalangeal Joint and the Thumb Interphalangeal Joint: A Retrospective Comparison of Kirschner Wires and the Acutrak 2 Headless Compression Screw
Abstract
Background:
Headless compression screws have become first choice for achieving arthrodesis in the distal interphalangeal joint and thumb interphalangeal joint. Only few comparisons between headless compression screws and other methods have been published.
Objective:
To assess healing and complication rate after arthrodesis of the distal interphalangeal joint or the thumb interphalangeal joint using a headless compression screw or Kirschner wires.
Methods:
A retrospective analysis of 148 consecutive primary fusions performed with the Acutrak 2 headless compression screw (n=107) or K-wires (n=41) was conducted. Healing was assessed clinically and radiographically at 6 to 8 weeks postoperatively.
Results:
In 89% of cases fusion had been achieved at 6 to 8 weeks postoperatively using the headless compression screw. 7 cases healed after 8 weeks. Secondary surgery with screw removal was required in 11 cases due to screw prominence, infection or non-union.
In 71% of cases fusion had been achieved at 6 to 8 weeks postoperatively using Kirschner wires showing a lower fusion rate at this stage as compared to the headless compression screw group (p<0.05). 9 joints in the Kirschner wire group fused at some point after 8 weeks of follow up yielding a total fusion rate of 93% which was similar to 96% in the headless compression screw group (p>0.05). One infection occurred in the Kirschner wire group.
Conclusion:
Arthrodesis can be achieved with either a headless compression screw or Kirschner wires both showing equivalent total fusion rates though fusion may occur earlier using a headless compression screw.
1. INTRODUCTION
Arthrodesis of the thumb interphalangeal joint (IP) and the Distal Interphalangeal Joint (DIP) is a well-documented method for reducing pain in the small joints of the finger. The most common indications for arthrodesis are osteoarthritis, rheumatoid arthritis, trauma or painful instability. Several treatment modalities have been described, including Kirschner wires (KW) [1, 2], intraosseous wiring [3], compression screws [4] and headless compression screws(HCS) [5]. Over the last few decades, the use of HCS has become the most favoured method of arthrodesis, as judged by the number of published papers using this technique. No results on the KW have been published since 1996. This may represent a shift of surgeons’ preference or publication bias, as stated by Dickson et al. [6].
The purpose of this study is to compare KW and HCS for arthrodesis of the DIP of digits 2-5 and the IP of the thumb in regard to time to fusion, fusion rate, complications including infection, revision surgery and non-union.
2. METHODS
A retrospective review of patients operated upon between January 2005 and December 2015 with fusion of a DIP or the IP has been included. The only exclusion criterion was prior arthrodesis. Of the 148 patients who met the inclusion criteria, 107 joints were operated upon with Acutrak 2 Headless Compression Screw (A2HCS) arthrodesis (Fig. 1) and 41 joints with KW arthrodesis (Fig. 2). Osteoarthritis was the main reason for receiving A2HCS arthrodesis, constituting diagnosis in 64% of the cases followed by rheumatoid arthritis (9%), trauma (8%), mallet finger (7%) and tendon lesions or gout (19%). Primary osteoarthritis was the main reason for receiving KW arthrodesis, constituting diagnosis in 77% of the cases, followed by trauma (10%), mallet finger (8%), and rheumatoid arthritis (3%). Choosing between A2HCS and KW was entirely up to the individual surgeon. One joint in the KW group was excluded because of a prior attempt to perform arthrodesis using a headless compression screw. Patient diagnosis, type of surgery, time to fusion, complications and reoperations were retrieved searching patient charts and radiographs. Healing was assessed clinically and radiographically at 6 to 8 weeks postoperatively. Minimum follow up was at least 12 months. Chi square test was calculated to compare healing rates between groups. P < 0.05 was considered statistically significant.
3. SURGICAL TECHNIQUE
The surgical procedure has previously been described in several other papers. The surgical exposure of the joint was the same whether performing arthrodesis using KW or HCS. We used a dorsal H- or S-shaped skin incision. Subsequently, the tendon was cut, thus exposing the joint. As regards performing KW arthrodesis, we used a technique similar to the one described by Burton et al. [7]. As regards performing HCS arthrodesis we used the technique described by Jean-Paul Brutus et al. [8]. Position of the KW arthrodesis was decided upon in agreement with the patient in slight flexion or straight alignment. When performing HCS arthrodesis the position was in always in straight alignment, as flexion is difficult to achieve when using a screw.
4. RESULTS
4.1. Acutrack 2 Headless Compression Screw
A total of 100 patients representing 107 joints were treated with A2HCS. Of these, 95 joints (89%) went on to fusion within 8 weeks postoperatively. Seven joints fused after 8 weeks postoperatively. Total fusion rate was 95%. Five joints did not fuse. Of the 107 joints treated with the A2HCS, 11 joints received revision surgery. Five screws were removed due to prominence of the screw in the pulp of the digit. Four screws were removed due to non-union but later went on to fusion after KW arthrodesis. In one patient, the joint did not fuse but the patient declined any further surgery. Two screws were removed because of infection.

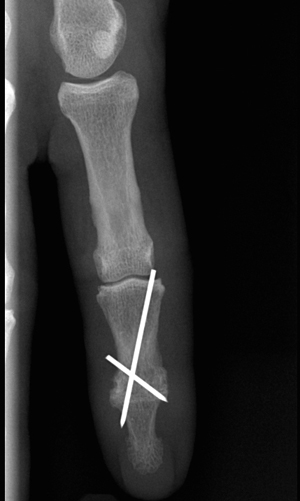
4.2. Kirschner Wires
A total of 40 patients representing 41 joints were treated with KW. Of these, 29 joints (71%) went on to fusion within 8 weeks postoperatively. Nine joints fused after 8 weeks postoperatively. Total fusion rate was 93%. Three joints did not fuse. Of the 41 joints treated with the KW, wires were removed at some point postoperatively in 26 cases (65%). The wires were removed in 24 joints as a result of loosening and prominence of the wires. Wires were removed in one patient after failure to fuse and the patient was not interested in further surgery. In one patient the wires were removed because of infection.
4.3. Comparison Of Acutrack 2 Headless Compression Screw And Kirschner Wires
More joints treated with A2HCS reached fusion within the 8 weeks postoperatively than in the group treated with KW (p < 0.05). There was no difference in total fusion rate between the two groups (p > 0.05). There were no differences in regard to complications, infections reoperation and non-union (p > 0.05).
5. DISCUSSION
In the present study, arthrodesis using A2HCS resulted in faster fusion compared to KW but there was no difference in the total fusion rate. It has been stated that time to fusion is a key factor in a good arthrodesis [2]. The present study suggests that early fusion is achieved more frequently when using A2HCS as compared to KW. To the best of our knowledge, a comparison of KW and a compression screw was last published in 1977 [4]. They treated 15 digits in each group and found that earlier mobilisation and return to work was achievable using the compression screw. Due to the relatively small number of joints treated and the fact that they used a headed compression screw, comparison of their results with the present study should be made with some caution.
In a systematic review from 2014, KW, tension band and headless compression screws were compared statistically using pooled data from several studies showing that headless compression screw was superior to KW in regard to total fusion rate [6]. Statistical power can be expected to increase when pooling data, thus enhancing the probability of detecting a significant difference between treatment modalities.
In the same review, it is also stated that using a compression screw for small joint arthrodesis comprises complications that are solely related to this technique. Thus, screw migration, fracturing of a bone [9] and screw prominence [10] necessitating further surgery have been reported after the use of headless compression screws. In 2012, Villani et al. [5] published on a series of 102 digits which all went on to union after treatment with headless compression screws. They stated that a learning curve is related to this technique. Two screws (2%) in that study were removed due to hardware prominence. Out of 19 surgeries performed previously at the same institution, seven screws were removed due to mal-placement of the screw. These cases, however, were excluded because of varying levels of experience amongst surgeons and more surgeons being involved. In our study, five screws (5%) were removed because of screw prominence. All cases were operated upon by experienced surgeons and we did not exclude any cases. Consequently, our relatively high percentage of screw prominence may partly reflect a learning curve for the procedure.
Postoperative infection necessitating revision surgery including hardware removal was seen in one joint (2%) following the KW arthrodesis and in two (2%) joints following A2HCS arthrodesis. These rates of infection are equivalent to the percentages seen in other studies [6].
In the present study, KW were removed in 24 joints of a total of 41 procedures. Seventeen of these cases were handled in our outpatient clinic while in seven cases the wires were removed in the theatre. All wires were removed under local anaesthesia. We consider the removal of wires an inherent part of KW arthrodesis. Nonetheless, the removal of wires entails some discomfort to patients, thus being a disadvantage compared to modalities where hardware removal is uncommon. We suggest that future studies report the prevalence of wire removal when performing KW arthrodesis.
Conclusion from this study must be drawn with considerable caution due to the retrospective and non-randomised design. There is a potential for selection bias due to the fact that each surgeon chose a procedure type on an individual basis.
Future randomised studies are needed to overcome this risk of bias and confounding.
CONCLUSION
This study found fusion to be achieved earlier when using A2HCS compared to using KW. However, total fusion rates were similar. Complication rates were low in both modalities.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used in this study that are basis of this research.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
Rights to data belongs to Hand Clinic, Herlev and Gentofte University, Copenhagen, Denmark.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


